Photosensitive Eczemas - Sunny Skin Sorrows
- Photosensitive eczemas are abnormal, eczematous skin reactions triggered or worsened by sunlight exposure, primarily UV radiation.
- Action Spectrum: UVA (320-400nm, "Aging" rays), UVB (290-320nm, "Burning" rays), and occasionally Visible Light.
- Clinical features: Pruritic, erythematous papules, vesicles, or plaques on sun-exposed sites; sparing photoprotected areas (e.g., under chin, retroauricular).
⭐ PMLE (Polymorphic Light Eruption) is the most common idiopathic photodermatosis, characterized by delayed onset (hours to days) after sun exposure.
Photosensitive Eczemas - PMLE & CAD Spotlight
-
Polymorphic Light Eruption (PMLE):
- Most common idiopathic photodermatosis; delayed-type hypersensitivity to UV.
- Onset: Hours-days post UV exposure (UVA > UVB).
- Lesions: Itchy papules, plaques, vesicles on sun-exposed areas (often spares face, V-neck, arms).
- "Hardening" phenomenon: Tolerance ↑ with repeated exposure.
- Rx: Sun protection, topical steroids, short course oral steroids for severe cases.
-
Chronic Actinic Dermatitis (CAD):
- A.k.a. Actinic Reticuloid, Photosensitive Eczema, Persistent Light Reactivity.
- Lesions: Severely itchy, thickened, lichenified plaques on chronically sun-exposed skin.
- Often affects elderly men; may persist for years.
- Broad action spectrum: UVB, UVA, and often visible light.
- Rx: Strict photoprotection (broad-spectrum), potent topical/systemic steroids, immunosuppressants (e.g., azathioprine).
⭐ Chronic Actinic Dermatitis (CAD) often presents with persistent, lichenified eczema in sun-exposed areas, predominantly in elderly males, and may show a 'persistent light reaction'.
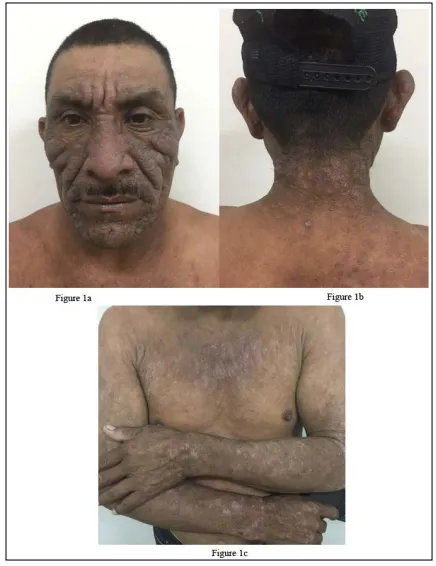
Photosensitive Eczemas - Drugs, Allergies Ahoy
- Abnormal reaction to UV radiation or visible light; eczematous changes.
- Key types: Phototoxic & Photoallergic.
- Phototoxic: More common; resembles exaggerated sunburn.
- Drugs: Tetracyclines (esp. Doxycycline), NSAIDs, Amiodarone, Thiazides.
- Photoallergic: Less common; immune-mediated (Type IV).
- Allergens: Sunscreens (PABA), fragrances, topical NSAIDs.
⭐ Photoallergic reactions are Type IV hypersensitivity, require prior sensitization, and can spread to non-exposed skin, unlike phototoxic reactions which are dose-dependent and confined to exposed areas.
- Solar Urticaria: Wheals on sun exposure; Type I hypersensitivity. Not eczematous. 📌 Remember Solar Urticaria = Sudden Urticaria.
- Actinic Prurigo: Familial, chronic, intensely itchy papules/nodules on sun-exposed skin; often starts in childhood.
- Chronic Actinic Dermatitis (CAD): Persistent eczema on sun-exposed sites, often in older men; can have ↓ MED (Minimal Erythema Dose).
Photosensitive Eczemas - Unmasking Sun's Mischief
- Eczematous reaction to UV/visible light on sun-exposed areas. Pruritus, erythema, papules, vesicles.
- Key Types:
- Polymorphic Light Eruption (PMLE): Common; delayed onset.
- Actinic Prurigo: Childhood; itchy nodules; HLA-DR4.
- Chronic Actinic Dermatitis (CAD): Older men; lichenified; ↓MED.
- Drug/Chemical-induced: Phototoxic/Photoallergic (drugs, chemicals).
- Key Approach:
⭐ Phototesting (including Minimal Erythema Dose - MED determination) and photopatch testing are key investigations to identify the causative wavelength and specific photosensitizer.
- Core Management: Strict photoprotection, topical corticosteroids/calcineurin inhibitors, systemic therapy (severe), hardening.
High‑Yield Points - ⚡ Biggest Takeaways
- PMLE: Most common; delayed itchy papules/plaques on sun-exposed areas.
- Spares photoprotected sites like under the chin and behind ears.
- Chronic Actinic Dermatitis (CAD): Persistent, lichenified eczema in older men; broad photosensitivity (UVA, UVB, visible light).
- Key symptom is intense pruritus; eruptions are typically symmetrical.
- Photopatch testing identifies photoallergens, differentiating from photoallergic contact dermatitis.
- Management: Strict sun protection, topical corticosteroids; phototherapy (hardening) for PMLE recurrence prevention.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

