Lichen Simplex Chronicus: Definition - The Itch That Rashes
- Localized, well-circumscribed area of chronic lichenification (thickened skin, exaggerated skin markings).
- Develops due to an "itch-scratch-itch" cycle: chronic, repetitive scratching or rubbing.
- Often termed "the itch that rashes" as pruritus (itching) precedes the skin changes.
- Not a primary skin disease.
⭐ LSC is a secondary skin disorder, not primary; it results from chronic physical trauma (rubbing/scratching) to the skin.

Lichen Simplex Chronicus: Pathophysiology - Skin's Vicious Loop
LSC is driven by a vicious cycle: an initial itchy stimulus provokes scratching, which traumatizes the skin. This trauma induces epidermal changes that paradoxically intensify the itch, perpetuating the cycle.
⭐ The itch-scratch-itch cycle is central to LSC, leading to epidermal hyperplasia (acanthosis), hyperkeratosis, and nerve fiber proliferation.
Lichen Simplex Chronicus: Clinical Features - Skin's Thick Story
- Intense Pruritus: Hallmark; paroxysmal, worse at night (itch-scratch cycle).
- Characteristic Lesions:
- Well-demarcated, thickened (lichenified) plaques.
- Exaggerated skin lines (Lichenification).
- Hyperpigmentation (post-inflammatory); may be hypopigmented in darker skin.
- Dry, leathery, "cobblestone" texture.
- Excoriations, fissures.
- Common Sites (accessible to scratching):
- Nape of neck, scalp.
- Ankles, lower legs.
- Wrists, extensor forearms.
- Anogenital area.
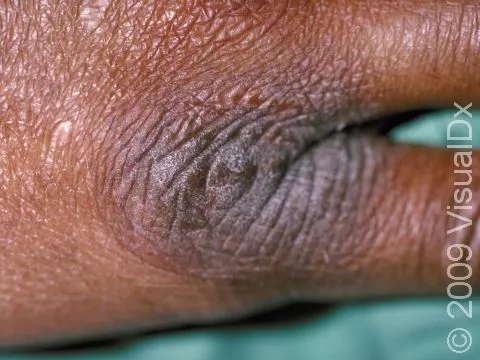
⭐ Key morphological features include well-demarcated, lichenified plaques with exaggerated skin markings and intense pruritus, often worse at night or during periods of rest.
Lichen Simplex Chronicus: Diagnosis & DDx - Not Just Any Itch
- Clinical Diagnosis:
- History: Intense, chronic, localized pruritus; habitual scratching.
- Morphology: Well-demarcated, lichenified plaques; exaggerated skin markings, excoriations, hyperpigmentation.
- Biopsy: Confirmatory; differentiates from key DDx.
- Differential Diagnosis (DDx):
- Psoriasis, Chronic Atopic Dermatitis, Nummular Eczema
- Tinea Cruris/Corporis (fungal)
- Allergic Contact Dermatitis
- Squamous Cell Carcinoma (SCC) in situ (Bowen's disease)
⭐ Diagnosis is primarily clinical based on history and morphology; biopsy (showing acanthosis, hyperkeratosis, papillomatosis, and chronic inflammation) is confirmatory and helps rule out differentials like psoriasis or fungal infections.
Lichen Simplex Chronicus: Management - Calming the Chaos
- Strategy: Interrupt itch-scratch cycle; reduce inflammation & lichenification.
- Key Pharmacotherapy:
- First-line: Potent topical corticosteroids (e.g., clobetasol propionate 0.05%).
- Refractory: Intralesional triamcinolone acetonide (2.5-10 mg/mL).
- Pruritus: Sedating antihistamines (e.g., hydroxyzine) for nocturnal relief.
- Essential Adjuncts: Behavioral modification (stop scratching!), occlusive dressings.
⭐ Management cornerstones: breaking the itch-scratch cycle (behavioral modification, occlusive dressings) and potent topical corticosteroids (e.g., clobetasol propionate). Intralesional steroids for refractory lesions.
High‑Yield Points - ⚡ Biggest Takeaways
- Localized neurodermatitis resulting from chronic, repetitive scratching/rubbing.
- Hallmark: Lichenification (thickened skin, exaggerated skin lines, leathery texture).
- Intense, paroxysmal pruritus is characteristic, often initiating the itch-scratch cycle.
- Common locations: nape of neck, ankles, wrists, extensor forearms, anogenital area.
- Skin shows hyperpigmentation and excoriations.
- Histopathology: epidermal hyperplasia (acanthosis), hyperkeratosis, chronic dermal inflammation.
- Treatment aims to break the itch-scratch cycle using potent topical corticosteroids and occlusion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

