Photoaging: Pathogenesis - Sun's Sneaky Strikes
- Primary Driver: UV Radiation (UVR) - UVA (aging) & UVB (burning).
- UVA (Deeper): Generates Reactive Oxygen Species (ROS) → oxidative stress.
- UVB (Superficial): Direct DNA damage (e.g., pyrimidine dimers).
- Key Mediators:
- ROS → ↑AP-1 → ↑Matrix Metalloproteinases (MMPs: collagenase, elastase).
- MMPs → Degrade collagen & elastin; ↓new collagen synthesis (↓TGF-β).
- Result: Impaired DNA repair, chronic inflammation, Extracellular Matrix (ECM) damage.
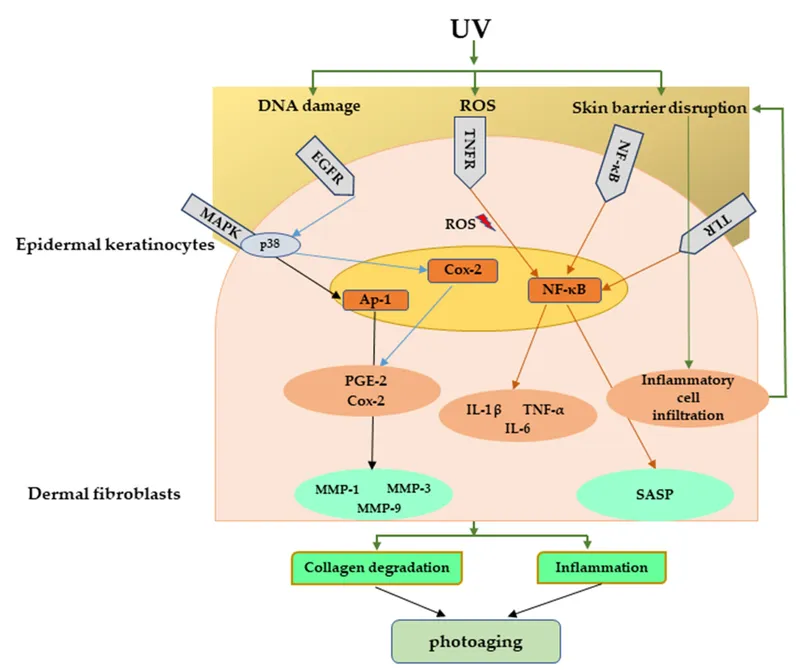
⭐ UV-induced ROS activates AP-1, which upregulates MMPs (e.g., collagenase), leading to collagen degradation and inhibiting new collagen synthesis.
Photoaging: Clinical Features & Grading - Skin's Sun Stories
- Clinical Features:
- Wrinkles: Fine to coarse.
- Texture: Rough, leathery; solar elastosis (yellow, thickened).
- Pigment: Solar lentigines, mottled hyperpigmentation, guttate hypomelanosis.
- Vascular: Telangiectasias.
- Other: Favre-Racouchot (comedones, cysts).
- Lesions: Actinic keratosis (AK), SCC, BCC.
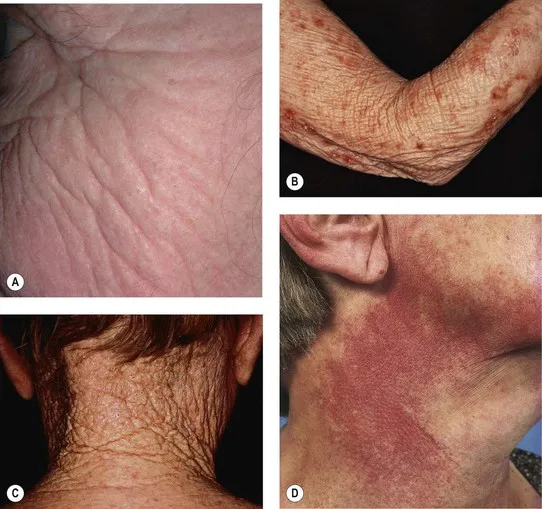
- Glogau Classification:
- Type I (Mild, 20s-30s): Minimal wrinkles; early pigment changes.
- Type II (Mod, 30s-40s): Wrinkles with motion; early lentigines, palpable AKs.
- Type III (Adv, 50s+): Wrinkles at rest; dyschromia, telangiectasias, visible AKs.
- Type IV (Severe, 60s-70s): Generalized wrinkles; yellow-gray skin, prior skin cancer.
⭐ The Glogau scale is pivotal for classifying photoaging severity, guiding treatment choices.
Photoaging: Histopathology - Dermal Deep Dive
- Solar Elastosis: Hallmark; abnormal, basophilic, tangled elastic fibers (elastotic material) in dermis.
- Verhoeff-Van Gieson (VVG) stain: Black.
- Collagen Changes:
- ↓ Type I & III collagen.
- ↑ Matrix Metalloproteinases (MMPs) (MMP-1, MMP-3, MMP-9) → collagen fragmentation.
- Glycosaminoglycans (GAGs): ↑ Hyaluronic acid (initially), later degrades; co-localizes with elastosis.
- Vascular: Dilated, tortuous vessels (telangiectasias); later ↓ vessel count.
- Inflammation: Mild, chronic perivascular infiltrate (lymphocytes, mast cells).
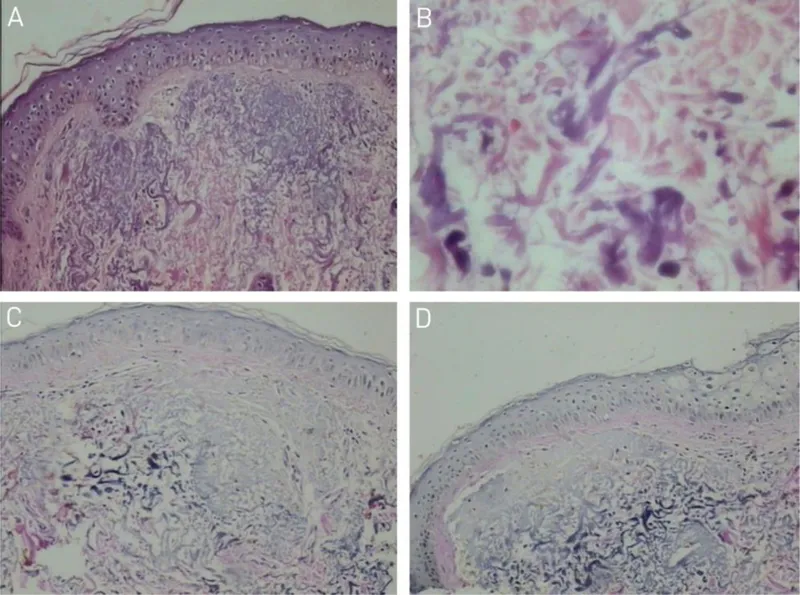
⭐ Solar elastosis, the dermal accumulation of abnormal elastic material, is the cardinal histopathological sign of photoaging.
Photoaging: Prevention - Shield & Shade
- Sunscreen: Broad-spectrum (UVA/UVB).
- SPF ≥30 (PA+++).
- Apply 15-30 min pre-exposure; reapply q2-3h.
- Protective Clothing:
- Wide-brimmed hats, tightly woven fabrics.
- UPF-rated garments.
- Seek Shade: Peak UV hours (10 AM - 4 PM).
- Avoid Tanning Beds: Absolutely.
- Antioxidants: Topical (Vit C, E); Oral (Polypodium).

⭐ Daily broad-spectrum sunscreen (SPF ≥30) is the most effective single measure against photoaging signs like wrinkles and lentigines.
Photoaging: Management - Turning Back Time
- Cornerstone: Daily broad-spectrum sunscreen (SPF ≥30) & topical retinoids (e.g., Tretinoin 0.025%).
- Topical Adjuncts: Antioxidants (Vit C, E, Ferulic acid), AHAs (Glycolic acid).
- Procedural Options (Step-up approach):
- Superficial: Chemical peels, Microdermabrasion.
- Moderate: Microneedling, Medium-depth peels.
- Advanced:
- Lasers: Non-ablative (Nd:YAG, IPL), Ablative (CO2, Er:YAG), Fractional.
- Radiofrequency (RF) for skin tightening.
- Injectables: Fillers (HA), Botulinum toxin for dynamic wrinkles.
- Systemic: Oral retinoids (severe cases, off-label).
⭐ Tretinoin remains the gold standard topical treatment, proven to reverse histological and clinical signs of photoaging.

High‑Yield Points - ⚡ Biggest Takeaways
- Photoaging is premature skin aging from chronic UVA/UVB exposure.
- Solar elastosis (abnormal elastic fibers in dermis) is the hallmark histological change.
- Key clinical features: wrinkles, solar lentigines, telangiectasias, leathery texture, actinic keratoses.
- Glogau classification is used to grade severity.
- Prevention: Broad-spectrum sunscreen, sun avoidance, protective clothing.
- Treatment: Topical retinoids (tretinoin), chemical peels, lasers.
- Favre-Racouchot syndrome: Severe photoaging with open/closed comedones and cysts_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

