Botulinum Toxin - Wrinkle Relaxer 101
- Potent neurotoxin from Clostridium botulinum; causes flaccid paralysis.
- Serotypes: A-G.
- BoNT-A (e.g., Botox, Dysport): Most common for aesthetics.
- BoNT-B (e.g., Myobloc): Alternative, faster onset, shorter duration.
- Mechanism: Blocks acetylcholine (ACh) release at neuromuscular junction (NMJ).
- Cleaves SNARE proteins (e.g., SNAP-25 by Type A).
- Effect: Temporary chemodenervation; muscle relaxation smooths dynamic wrinkles.
- Kinetics: Onset 24-72 hrs; Peak 1-2 wks; Duration 3-6 months.
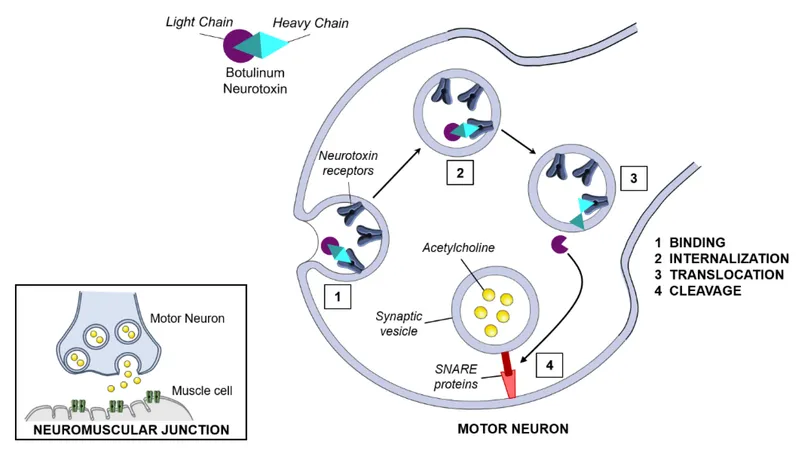
⭐ BoNT-A cleaves SNAP-25, while BoNT-B targets VAMP/Synaptobrevin, both essential for ACh vesicle exocytosis.
Botulinum Toxin - Face Freeze Frame
- Mechanism: Blocks acetylcholine (ACh) release at NMJ → temporary muscle paralysis.
- Type: BoNT-A (e.g., Botox®, Dysport®) is main.
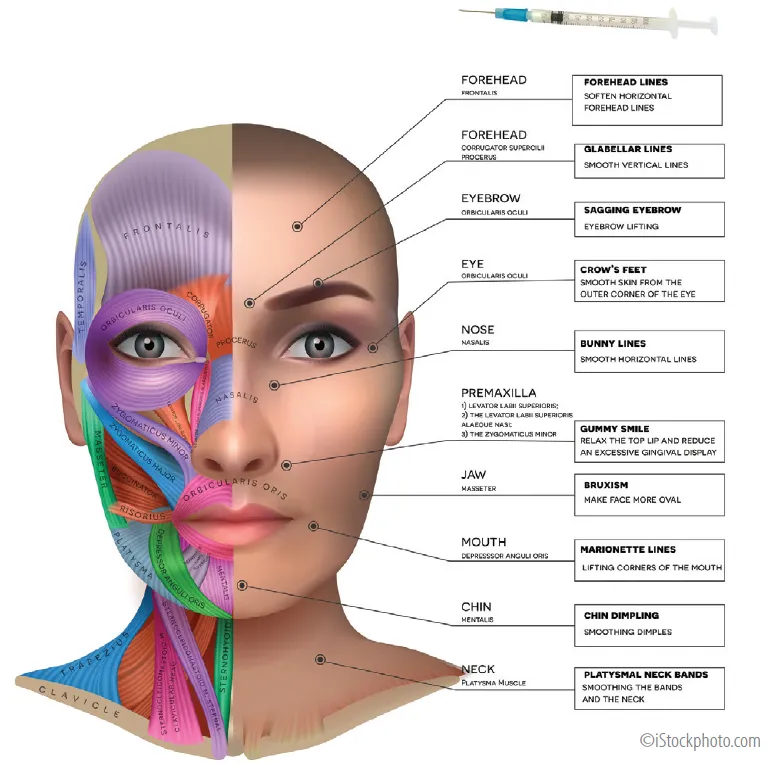
- Uses (Face):
- Glabellar lines (Corrugator supercilii, Procerus)
- Forehead lines (Frontalis)
- Crow’s feet (Orbicularis oculi)
- Effects:
- Onset: 3-7 days.
- Peak: ~2 weeks.
- Lasts: 3-4 months (can be up to 6).
- Sites:
- Glabella: Typically 5 points.
- Forehead: Avoid lateral overaction (prevents "Spock brow").
- Crow's feet: Lateral to orbital rim.
- Risks: Bruising, headache, ptosis (eyelid/brow), asymmetry.
- 📌 ACh Blocked, Creases Diminished.
- 📌 ACh Blocked, Creases Diminished.
⭐ Eyelid ptosis from BoNT injection is due to diffusion to levator palpebrae superioris; apraclonidine eye drops can offer temporary relief by stimulating Müller's muscle.
Botulinum Toxin - Toxin's Healing Touch
- Blocks acetylcholine (ACh) release at neuromuscular junctions & autonomic nerve terminals.
- Therapeutic Uses (Non-Cosmetic):
- Neurological: Spasticity (e.g., cerebral palsy, post-stroke), dystonias (blepharospasm, cervical dystonia), hemifacial spasm.
- Pain Syndromes: Chronic migraine.
- Hypersecretory: Hyperhidrosis (axillary, palmar), sialorrhea, Frey's syndrome.
- Ophthalmological: Strabismus.
- Urological: Overactive bladder, neurogenic detrusor overactivity.
- Clinical effect typically lasts 3-6 months, requiring repeat injections.
⭐ BoNT-A is an established prophylactic treatment for chronic migraine (defined as headaches on ≥15 days/month).
Botulinum Toxin - Toxin Trouble Tidbits
Contraindications:
- Neuromuscular disorders (Myasthenia Gravis, ALS)
- Pregnancy, lactation
- Infection at injection site
- Aminoglycoside use ⚠️
Common Side Effects:
- Injection site: Pain, erythema, bruising
- Headache, flu-like symptoms
Specific Complications & Management:
- Ptosis (eyelid droop):
- Cause: Spread to levator palpebrae superioris.
- Management: Apraclonidine 0.5% eye drops; resolves in weeks.
- Brow ptosis: Usually self-limiting.
- "Spock Brow" / "Mephisto Sign": Lateral brow elevation; treat with tiny BoNT dose in frontalis.
- Diplopia: Rare, transient.
- Dysphagia (neck injections): Dose-dependent, supportive care.
- ⚠️ Systemic spread (rare): Botulism-like symptoms (weakness, respiratory distress) → Emergency!
⭐ Most common cause of ptosis after BoNT for glabellar lines is diffusion of toxin to the levator palpebrae superioris muscle.
Botulinum Toxin - Toxin Admin Tips
- Reconstitution: Use sterile, preservative-free 0.9% saline. Gently swirl; avoid shaking.
- Storage: Per manufacturer; typically 2-8°C (refrigerated) before and after reconstitution. Use within 4-24 hours (varies by brand).
- Injection: Slow, steady pressure. Small gauge needles (30-32G).
- Aspiration: Generally not needed for standard facial injections.
- Post-injection: Advise patient to remain upright for 3-4 hours, avoid rubbing/massaging treated area for 24 hours.
⭐ Avoid NSAIDs/aspirin/alcohol 1 week pre-injection to ↓ bruising risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Mechanism: Blocks acetylcholine release at neuromuscular junction (NMJ), causing temporary muscle paralysis.
- Primary Type: Botulinum Toxin A (BoNT-A) is the mainstay for cosmetic use (e.g., Botox, Dysport).
- Key Uses: Treats dynamic wrinkles (glabella, crow's feet, forehead) and axillary/palmar hyperhidrosis.
- Onset & Duration: Effects appear in 3-7 days, lasting 3-6 months.
- Most Common Side Effect: Eyelid ptosis from upper face injections; bruising is also common.
- Contraindications: Myasthenia Gravis, Eaton-Lambert syndrome, pregnancy, lactation, infection at site.
- Dilution: Reconstituted with preservative-free 0.9% sodium chloride (normal saline).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

