Intro & Assessment - Stage Setters
- Body Contouring: Procedures to reshape body aesthetics by ↓fat, ↑skin tightness, or ↑muscle tone.
- Ideal Candidate:
- Stable weight, good general health.
- Realistic expectations.
- Often BMI <30.
- Contraindications:
- Absolute: Active infection, pregnancy, severe systemic disease.
- Relative: Poorly controlled diabetes, smoking.
- Pre-procedure Evaluation:
- Detailed history (medical, surgical, meds).
- Physical exam: Skin laxity, fat distribution, muscle tone.
- Photographic documentation.
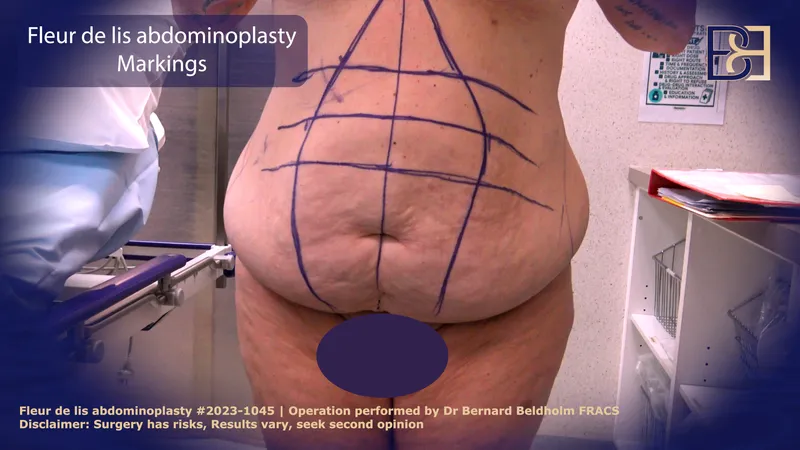
⭐ Realistic patient expectations are paramount for satisfaction in body contouring procedures.
Non-Invasive Tech - Zap & Freeze
Non-invasive body contouring techniques aim to reduce localized fat deposits and improve body shape without surgery.
| Modality | Mechanism & Key Features | Target Tissue | Efficacy | Downtime | Key Side Effect(s) |
|---|---|---|---|---|---|
| Cryolipolysis | Adipocyte apoptosis via controlled cooling. Common areas: abdomen, flanks, thighs. | Subcutaneous fat | Moderate | Minimal | Temporary numbness, erythema, bruising; Rare: PAH. |
| Radiofrequency (RF) | Bulk heating → collagen remodeling, lipolysis. Types: monopolar, bipolar, multipolar. For skin tightening, cellulite, fat reduction. | Dermis, fat | Mild-Moderate | None-Minimal | Transient erythema. |
| HIFU | Thermal ablation of subcutaneous fat via focused ultrasound; depth control. For fat reduction, skin lifting. | Subcutaneous fat | Moderate | Minimal | Temporary discomfort, bruising. |
| Injection Lipolysis | Deoxycholic acid causes adipocytolysis. Approved for submental fat (double chin). | Submental fat | Moderate | Minimal | Swelling, pain, numbness. |
⭐ Paradoxical Adipose Hyperplasia (PAH) is a rare but important adverse effect of cryolipolysis.
Surgical Options - Sculpt & Tuck
-
Liposuction: Surgical removal of localized subcutaneous fat deposits (e.g., abdomen, thighs, arms) to improve body contours. Not a weight-loss method.
- Tumescent Technique: Infiltration of large volumes of dilute anesthetic solution.
- Components: 📌 TALL SNoopy (Tumescent Anesthesia - Lidocaine, Adrenaline/Epinephrine, Saline, Sodium bicarbonate).
- Benefits: ↓Blood loss, prolonged local anesthesia, ↑safety.
- Max Lidocaine: 45-55 mg/kg (tumescent); 7 mg/kg (plain).
- Types:
- Suction-Assisted (SAL): Traditional.
- Ultrasound-Assisted (UAL): Good for fibrous areas (e.g., back, gynecomastia).
- Power-Assisted (PAL): Vibrating cannula, less surgeon fatigue.
- Laser-Assisted (LAL): Potential for skin tightening.
- Tumescent Technique: Infiltration of large volumes of dilute anesthetic solution.
-
Excisional Procedures: For significant skin laxity ± fat.
- Abdominoplasty ("Tummy Tuck"): Removes excess skin/fat from abdomen; tightens abdominal muscles (diastasis recti repair).
- Brachioplasty (Arm Lift).
- Thigh Lift.
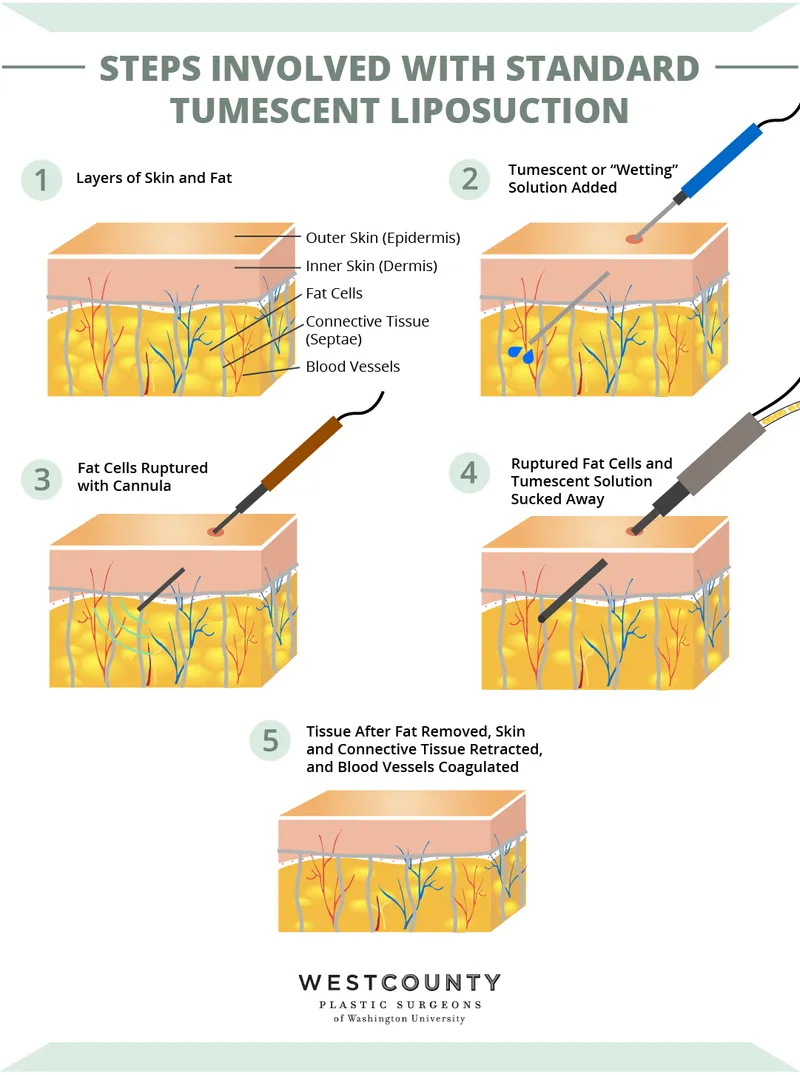
⭐ The tumescent technique revolutionized liposuction by significantly reducing blood loss and providing prolonged local anesthesia.
Aftermath & Issues - Smooth Sailing?
- General Risks: Hematoma, seroma, infection, VTE (DVT/PE - prophylaxis vital).
- Procedure-Specific Issues:
- Liposuction: Contour irregularities, skin necrosis, fat embolism, lidocaine toxicity (max dose 4.5mg/kg plain, 7mg/kg with epi).
- Cryolipolysis: Paradoxical Adipose Hyperplasia (PAH), transient sensory loss.
- RF/HIFU: Burns, pain.
- Excisional: Dehiscence, hypertrophic scars, nerve injury.
- Post-Procedure Care:
- Compression garments (reduce swelling, support).
- Pain relief, restricted activity.
- Wound care (surgical). Regular follow-up.
⭐ Contour irregularities are the most common aesthetic complication following liposuction.
High‑Yield Points - ⚡ Biggest Takeaways
- Tumescent liposuction is the most common surgical method, minimizing blood loss.
- Cryolipolysis offers non-invasive fat reduction via controlled cooling inducing apoptosis.
- Radiofrequency (RF) and HIFU utilize thermal energy for non-surgical lipolysis and skin tightening.
- Deoxycholic acid is an injectable cytolytic agent for submental fat.
- Paradoxical Adipose Hyperplasia (PAH) is a rare complication of cryolipolysis.
- Common liposuction complications include seroma, hematoma, and contour irregularities.
- Realistic expectations and proper patient selection are paramount for all procedures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

