Dermatological History - Clue Collector
- Presenting Complaint (PC):
- Site, Symptoms (itch, pain), Severity
- Onset, Duration, Course (progression, recurrence)
- Aggravating/Relieving factors
- Associated systemic symptoms (fever, malaise)
- Previous episodes, treatments, response
- Past Medical History (PMH):
- Atopy (eczema, asthma, rhinitis)
- Other skin diseases, chronic illness (diabetes, immunosuppression)
- Drug History:
- Current/recent medications (esp. new)
- Allergies, prior adverse drug reactions
⭐ Drug history is key; some drugs cause severe reactions (SCARs) like Stevens-Johnson Syndrome (SJS).
- Family History: Similar conditions, hereditary disorders (ichthyosis, neurofibromatosis).
- Personal/Social History: Occupation, travel, sun exposure, pets, stress.
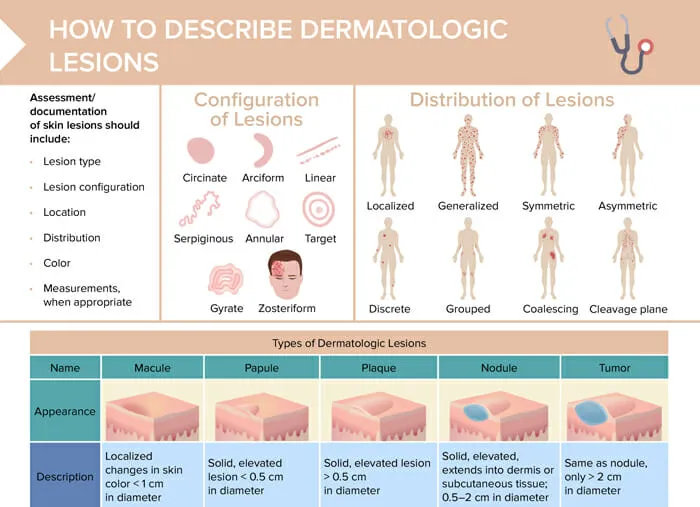
Skin Lesion Morphology - Skin Speak
Accurate lesion description is key. Primary lesions arise on normal skin; secondary lesions evolve or result from trauma (e.g., scratching).
- Primary Lesions: (Initial skin changes)
- Macule: Flat, color change, <1cm. Patch: Larger macule, >1cm.
- Papule: Solid, raised, palpable, <1cm. Plaque: Raised, flat-topped, >1cm (confluent papules).
- Nodule: Solid, raised, deeper & firmer than papule, often >1cm.
- Vesicle: Fluid-filled (serous), raised, <1cm. Bulla: Larger vesicle, >1cm.
- Pustule: Vesicle/bulla containing pus.
- Wheal: Transient, edematous, erythematous papule/plaque (e.g., urticaria).

- Secondary Lesions: (Evolved or trauma-induced)
- Scale: Flakes of stratum corneum.
- Crust: Dried exudate (serum, blood, pus).
- Erosion: Superficial epidermal loss; heals without scar.
- Ulcer: Deeper loss (dermis/subcutis); heals with scar.
- Fissure: Linear crack in skin.
- Lichenification: Thickened skin, exaggerated markings (chronic rubbing).
- Atrophy: Thinning of skin layers.
⭐ Koebner Phenomenon (Isomorphic Response): Development of new lesions of a pre-existing dermatosis (e.g., psoriasis, lichen planus, vitiligo) at sites of skin trauma or injury.
Dermatological Examination - Dermo Detective Kit
- Inspection:
- Good lighting; Magnifying lens/Dermatoscope.
- Examine: skin, hair, nails, mucosa.
- Distribution:
- Symmetry, sites (flexural, extensor, acral, dermatomal).
- Configuration:
- Linear, annular, arcuate, grouped, serpiginous, reticular.
- Palpation:
- Consistency, tenderness, temperature, depth.
- Key Signs & Tools:
- Diascopy: Blanching (vascular).
- Nikolsky's sign: Epidermal shear.
- Auspitz sign: Bleeding on scale removal (psoriasis).
- Darier's sign: Urtication on rubbing (mastocytosis).
- Koebner phenomenon: Lesions at trauma sites.
- Wood's Lamp: Fluorescence (e.g., Microsporum).
⭐ Auspitz sign: Characteristic pinpoint bleeding when scales are scraped off a psoriatic plaque; reveals underlying elongated, dilated dermal papillae.
Diagnostic Procedures - Lab Lens
- KOH Mount: Fungal elements (dermatophytes, Candida). 10-20% KOH.
- Tzanck Smear: Multinucleated giant cells (Herpes), acantholytic cells (Pemphigus). Giemsa.
- Gram Stain: Bacteria.
- AFB Stain (ZN): Mycobacteria (leprosy, cutaneous TB).
- Wood's Lamp (UV-A 365nm):
- Microsporum: Blue-green.
- C. minutissimum: Coral-red (Erythrasma).
- Malassezia: Yellow-orange (P. versicolor).
- Diascopy: Blanching (vascular) vs. non-blanching (hemorrhagic).
- Skin Biopsy: Punch, shave, excision for histopathology.
⭐ Wood's lamp: Corynebacterium minutissimum in erythrasma fluoresces coral-red.
High‑Yield Points - ⚡ Biggest Takeaways
- Thorough history and lesion morphology (type, shape, distribution) are paramount.
- Diascopy differentiates blanchable erythema from non-blanchable purpura.
- Wood's lamp detects specific fungal infections (e.g., Microsporum green fluorescence) and erythrasma (coral red).
- KOH mount is vital for confirming superficial fungal infections by visualizing hyphae.
- Tzanck smear identifies multinucleated giant cells in herpetic infections.
- Skin biopsy is often the gold standard for definitive diagnosis, especially for tumors.
- Dermoscopy improves melanoma detection by visualizing subsurface structures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

