Geriatric Dermatology: Skin Aging & Xerosis - Wrinkles & Itches
- Skin Aging Mechanisms:
- Intrinsic (chronological): Genetically programmed, gradual.
- Extrinsic (e.g., photoaging): Environmental; UV radiation is key, causing most visible changes.
- Pathophysiological Changes:
- Dermis: ↓ Collagen, ↓ elastin → wrinkles, laxity.
- Epidermis: Thinning, ↓ melanocytes (uneven pigmentation), ↓ Langerhans cells (↓ immune surveillance).
- Overall: Impaired barrier function, ↓ sebum & sweat production → xerosis (dryness).
- Clinical Manifestations: Fine wrinkles, skin laxity, xerosis, pruritus (itching), delayed wound healing, senile purpura.
- Xerosis Management: Regular emollients, humidifiers, lukewarm (not hot) baths, mild soaps.

⭐ Extrinsic aging, primarily photoaging, accounts for most visible age-related skin changes and is largely preventable.
Geriatric Dermatology: Common Benign Lesions - Spots & Bumps
| Lesion | Appearance | Common Location | Malignant Potential |
|---|---|---|---|
| Seborrheic Keratosis (SK) | Waxy, "stuck-on", brown/black, verrucous | Trunk, face, extremities | Generally none |
| Cherry Angioma | Bright red papules, blanchable | Trunk, extremities | None |
| Senile Lentigo (Liver Spot) | Flat, brown macules, well-demarcated | Sun-exposed areas | None |
| Skin Tag (Acrochordon) | Soft, pedunculated, skin-colored/brown | Neck, axillae, groin | None |
⭐ The Sign of Leser-Trélat, characterized by the sudden onset and rapid increase in size and number of seborrheic keratoses, can be a cutaneous marker of internal malignancy.
Geriatric Dermatology: Pruritus, Eczemas & Bullous Pemphigoid - Itchy Inflammations
- Pruritus: Intense itch, common in elderly.
- Causes: Xerosis (most frequent), systemic diseases (CKD, liver), drugs, psychogenic.
- Eczemas:
- Asteatotic (Craquelé): "Crazy paving" cracks on dry skin, esp. shins.
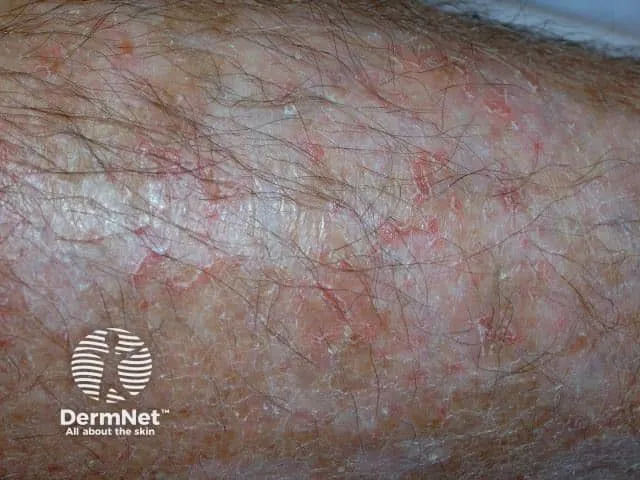
- Nummular: Coin-shaped, itchy, erythematous plaques.
- Asteatotic (Craquelé): "Crazy paving" cracks on dry skin, esp. shins.
- Bullous Pemphigoid (BP): Commonest autoimmune blistering disease.
- Elderly; prodromal itch/urticaria → tense bullae.
- Antibodies: 📌 BPAG1 (BP230), BPAG2 (BP180).
- Dx: Biopsy (subepidermal), DIF (linear C3/IgG at BMZ).
⭐ Bullous pemphigoid is the most common autoimmune blistering disease, typically affecting the elderly, and often presents with intense pruritus weeks to months before blister formation.
- Management (Pruritus/Eczemas):
- Emollients (liberal use).
- Topical corticosteroids.
- Oral antihistamines.
Geriatric Dermatology: Skin Cancers & Actinic Keratosis - Sun's Scars
Cumulative sun exposure significantly ↑ risk in geriatrics. Atypical presentations are common.
⭐ Actinic keratoses are common, sun-induced premalignant lesions that have the potential to transform into squamous cell carcinoma.
Key Skin Lesions in the Elderly:
| Feature | Actinic Keratosis (AK) | Basal Cell Carcinoma (BCC) | Squamous Cell Carcinoma (SCC) | Malignant Melanoma |
|---|---|---|---|---|
| Type | Pre-malignant (for SCC) | Most common | ↑ Metastatic risk (vs BCC) | Most aggressive |
| Geriatric Focus | Rough, scaly; sun-exposed | Pearly papule/nodule; slow growth | Crusted/ulcerated lesion; faster | New/changing mole; atypical; 📌ABCDE (Diameter >6mm) |
| Treatment | Cryo, topical (5-FU) | Excision, Mohs | Excision, Mohs, RT | Excision, SLNB, systemic therapy |
- Key: Sun protection (broad-spectrum sunscreen, protective clothing).
High-Yield Points - ⚡ Biggest Takeaways
- Senile purpura: Benign ecchymoses on extensor surfaces from capillary fragility and dermal atrophy.
- Xerosis cutis: Most common cause of geriatric pruritus; treat with emollients.
- Stasis dermatitis: From chronic venous insufficiency; causes lower leg eczema, pigmentation, ulcers.
- Seborrheic keratoses: Common benign "stuck-on" epidermal tumors; no malignant potential.
- Herpes zoster: Incidence and post-herpetic neuralgia risk ↑ with age.
- Skin cancers (BCC, SCC, Melanoma): Risk ↑ significantly with age and sun exposure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

