Cutaneous Immunology - Skin's Guardian Squad

- Skin-Associated Lymphoid Tissue (SALT): Integrated system for cutaneous immune surveillance.
- Innate Immunity (Rapid Defense):
- Keratinocytes: Barrier; cytokines (IL-1, TNF-α), antimicrobial peptides (AMPs).
- Langerhans Cells (LCs): Epidermal dendritic cells; potent antigen-presenting cells (APCs).
- Others: Dermal Dendritic Cells (DDCs), Macrophages, Mast cells, NK cells.
- Adaptive Immunity (Specific & Memory):
- T-lymphocytes: CD4+ Helper (Th1, Th2, Th17, Treg), CD8+ Cytotoxic.
- B-lymphocytes: Antibody production via plasma cells.
- Key Cytokines (Cellular Messengers):
- Pro-inflammatory: TNF-α, IL-1, IL-6, IL-17, IFN-γ.
- Anti-inflammatory: IL-10, TGF-β.
⭐ Langerhans cells, key epidermal APCs, uniquely contain Birbeck granules (tennis-racket shape on EM), crucial for initiating skin immune responses.
Cutaneous Immunology - Antigen Alert System
- Skin's surveillance: Detects pathogens via Pattern Recognition Receptors (PRRs) e.g., Toll-like Receptors (TLRs).
- Key Antigen Presenting Cells (APCs):
- Langerhans Cells (LCs): Epidermal; migrate to lymph nodes.
- Dermal Dendritic Cells (DDCs): In dermis.
- Keratinocytes: Can express MHC-II; produce cytokines (TNF-α, IL-1).
- Process: APCs capture, process, and present antigens on MHC molecules to T-cells, initiating adaptive immunity.

⭐ Langerhans cells uniquely contain Birbeck granules (tennis-racket shaped organelles on EM) and express CD1a & Langerin (CD207). 📌 Birbeck = Tennis Racket shape on EM for LCs!
Cutaneous Immunology - Itch & Scratch Saga
- Hypersensitivity Reactions: Immune overreactions causing tissue damage & pruritus. 📌 Mnemonic: ACID
- Type I (A - Allergic/Anaphylactic): IgE-mediated; mast cell degranulation (histamine).
- Urticaria, angioedema. Intense itch.
- Type II (C - Cytotoxic): IgG/IgM vs. cell-bound antigens.
- Ex: Pemphigus.
- Type III (I - Immune Complex): Ag-Ab complex deposition.
- Ex: Cutaneous vasculitis.
- Type IV (D - Delayed): T-cell mediated (Th1, CTLs).
- Ex: Allergic contact dermatitis (ACD). ACD: severe itch.
- Type I (A - Allergic/Anaphylactic): IgE-mediated; mast cell degranulation (histamine).
- Pruritus Mediators: Histamine, serotonin, Prostaglandins (PGs), Leukotrienes (LTs), Substance P, IL-31.
- Itch-Scratch Cycle: Itch → Scratch → Skin barrier disruption → Inflammation → ↑Itch → Lichenification.
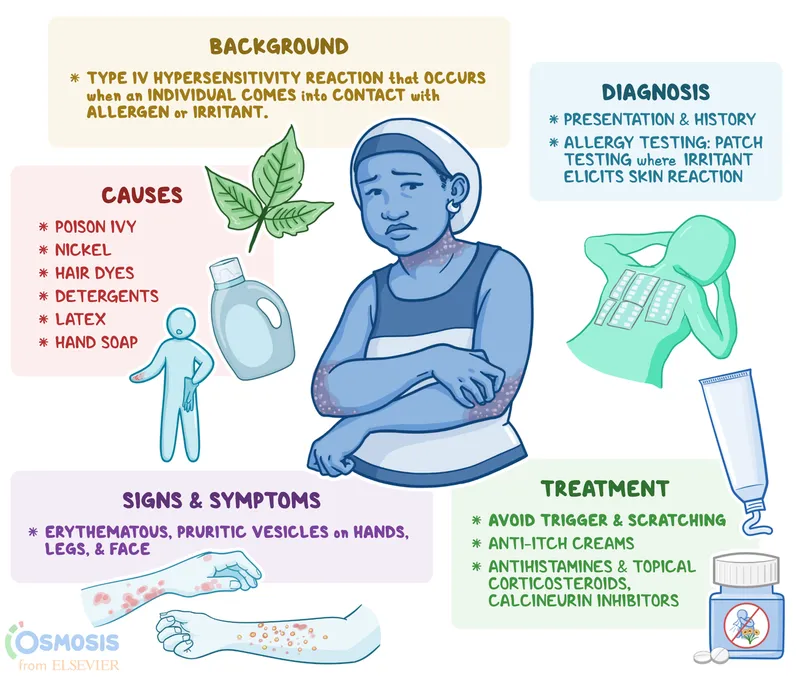
⭐ Type IV hypersensitivity is the mechanism behind allergic contact dermatitis, a common cause of severe, T-cell driven itch and eczematous skin changes.
Cutaneous Immunology - Self-Sabotage Stories
- Autoimmunity: Immune system attacks skin's self-antigens due to failed self-tolerance.
- Key Mediators:
- Autoantibodies: Target skin structures (e.g., desmogleins in Pemphigus).
- Autoreactive T-cells: Drive inflammation/damage (e.g., Lichen Planus).
- Cytokines (TNF-α, IL-17): Amplify response.
- Damage Mechanisms:
- Type II Hypersensitivity: Antibody-driven (Pemphigus, Bullous Pemphigoid).
- Type IV Hypersensitivity: Cell-mediated (Lichen Planus).
- Common Autoimmune Skin Diseases:
- Pemphigus Vulgaris (PV): Anti-desmoglein 3, 1. Intraepidermal.
- Bullous Pemphigoid (BP): Anti-BPAG1 (BP230), BPAG2 (BP180). Subepidermal.
- Lupus Erythematosus (LE): ANA, anti-dsDNA.
- Dermatomyositis (DM): Anti-Mi-2, anti-Jo-1.
⭐ Pemphigus vulgaris often presents with oral mucosal erosions before skin lesions develop.
High‑Yield Points - ⚡ Biggest Takeaways
- Langerhans cells: Epidermal APCs; crucial for initiating Type IV hypersensitivity.
- Keratinocytes: Active source of cytokines (IL-1, TNF-α); contribute to innate and adaptive skin immunity.
- Th1 cells: Mediate Delayed-Type Hypersensitivity (DTH) (e.g., contact dermatitis) via IFN-γ.
- Th2 cells: Key in atopic dermatitis and urticaria, producing IL-4, IL-5, IL-13.
- Mast cells: Release histamine and mediators in urticaria and anaphylaxis.
- Autoantibodies: Anti-desmoglein (Pemphigus Vulgaris), anti-BPAG1/2 (Bullous Pemphigoid) are key markers.
- CLA (Cutaneous Lymphocyte Antigen): Marker for skin-homing T lymphocytes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

