Prophylaxis and Management - Skin Invaders ID
Key Bacterial Skin Infections:
| Infection | Organism(s) | Key Feature(s) |
|---|---|---|
| Impetigo (Non-B) | S. aureus, S. pyogenes | Honey-colored crusts |
| Impetigo (Bullous) | S. aureus (exfoliative toxin) | Flaccid bullae |
| Ecthyma | S. pyogenes, S. aureus | "Punched-out" ulcers, deeper than impetigo |
| Folliculitis | S. aureus (most common) | Pustules centered on hair follicles |
| Furuncle (Boil) | S. aureus | Deep, tender, firm erythematous nodule |
| Carbuncle | S. aureus | Multiple furuncles, draining sinuses |
| Cellulitis | S. pyogenes, S. aureus | Spreading erythema, warmth, ill-defined border |
| Erysipelas | S. pyogenes | Fiery red, raised, sharply demarcated, tender |
⭐ Honey-colored crusts are pathognomonic for non-bullous impetigo.
General Prophylaxis & Management:
- Hygiene: Handwashing, clean wounds.
- Topical antibiotics (e.g., mupirocin) for localized infections.
- Systemic antibiotics for widespread/severe infections (e.g., penicillins, cephalosporins).
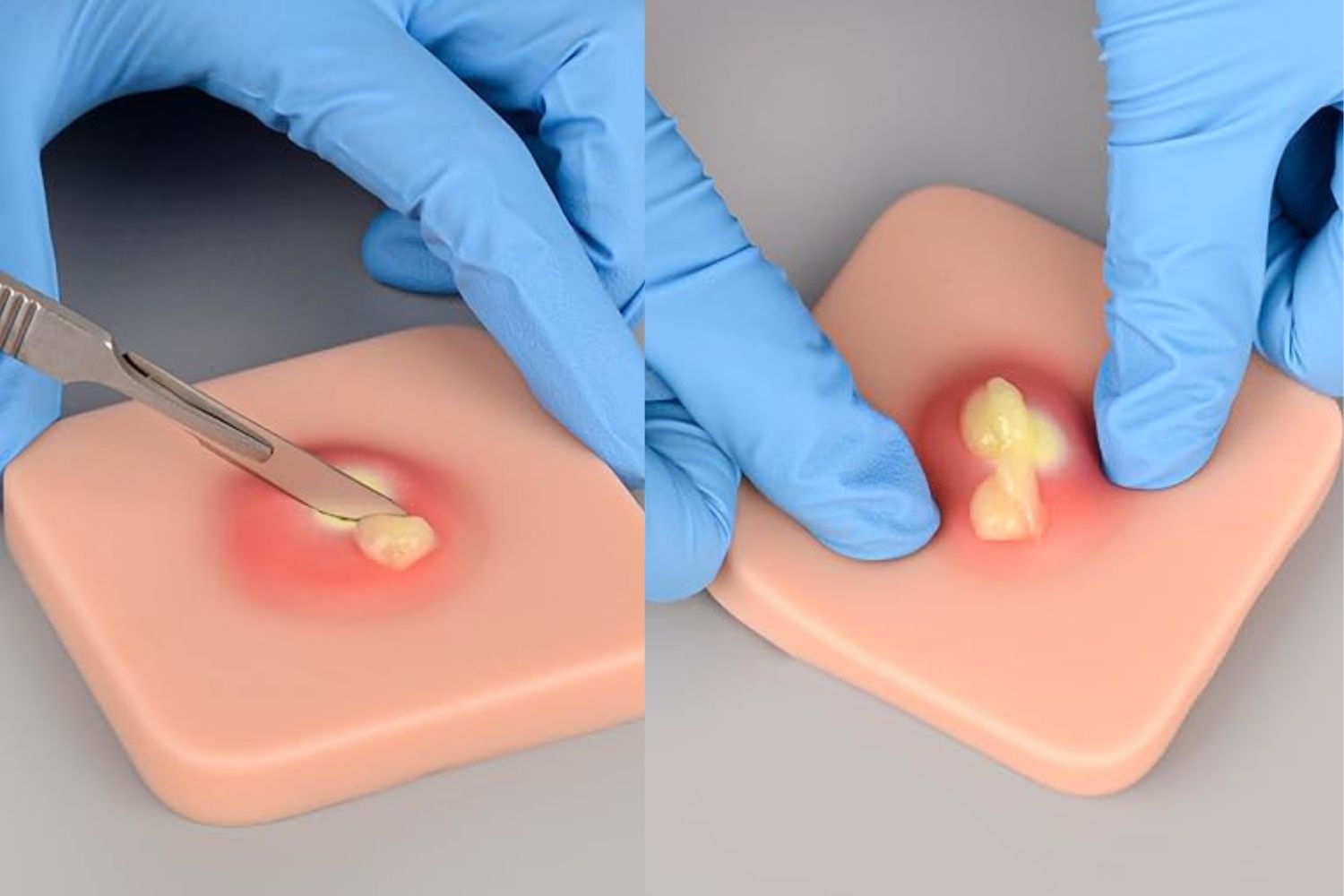
- Incision & Drainage (I&D) for abscesses (furuncles, carbuncles).
- 📌 CELLulitis: Connective tissue, Edges Loose, Lower limbs. Erysipelas: Edges Raised, Yare (sharp).
Prophylaxis and Management - Defense Tactics
- Fundamental Defense:
- Hand hygiene: Cornerstone of prevention.
- Skin antisepsis: Use chlorhexidine or povidone-iodine pre-procedure.
- Wound care: Adhere to basics - keep clean, covered, and monitor.
- S. aureus Decolonization Strategy (for identified carriers):
- Nasal mupirocin: Apply 2% ointment BID for 5-7 days.
⭐ Nasal mupirocin is a key strategy for preventing recurrent S. aureus skin infections in carriers.
- Surgical Prophylaxis (SSI Prevention):
- Pre-operative antibiotics: Cefazolin is a common choice.
- Optimal timing: Administer 30-60 minutes before surgical incision.
- Consider vancomycin/clindamycin for penicillin allergy or high MRSA risk.
Prophylaxis and Management - Bug Battle Plan
- Prevention: Hand hygiene, wound care, decolonization (e.g., mupirocin for nasal MRSA).
- Supportive Care: Elevation, analgesia, cool compresses.
- Therapy Choice: Empirical vs. Culture-directed.
- Topical Antibiotics:
- Mupirocin (Bactroban): Impetigo, MRSA decolonization.
- Fusidic acid: Staph infections.
- Retapamulin (Altabax): Impetigo.
- Systemic Antibiotics: 📌 Powerful Combatants Make Clean Tissue (Penicillins, Cephalosporins, Macrolides, Clindamycin, Tetracyclines)
| Antibiotic Class | Spectrum Highlights | Common Uses in Skin Infections |
|---|---|---|
| Penicillins | Strep, Staph (non-MRSA) | Cellulitis, Erysipelas |
| Cephalosporins | Broader G+ve, some G-ve | Cellulitis, Abscesses |
| Macrolides | G+ve, Atypicals | Penicillin allergy |
| Clindamycin | Staph (incl. some MRSA), Strep, Anaerobes | SSTIs, MRSA, Toxin-mediated |
| Tetracyclines | G+ve, G-ve, MRSA | Acne, MRSA, Tick-borne |
- Duration: Typically 5-10 days for uncomplicated SSTIs.
⭐ Clindamycin is preferred for suspected Staphylococcal or Streptococcal infections if penicillin allergy, and it also has anti-toxin effects.
Prophylaxis and Management - Resistant Rogues
- MRSA (Methicillin-Resistant S. aureus)
- CA-MRSA: Community-acquired, typically SSTIs, Panton-Valentine Leukocidin (PVL) toxin common.
- HA-MRSA: Hospital-acquired, often more invasive, higher multi-drug resistance.
- Risk Factors: Crowding, Contact (skin-to-skin), Compromised skin, Contaminated items, lack of Cleanliness.
- Treatment: 📌 MRSA Can't Dodge The Line Van (Clindamycin, Doxycycline/Minocycline, TMP-SMX, Linezolid, Vancomycin).
- D-test: Perform if S. aureus is erythromycin-resistant and clindamycin-susceptible to check for inducible clindamycin resistance.
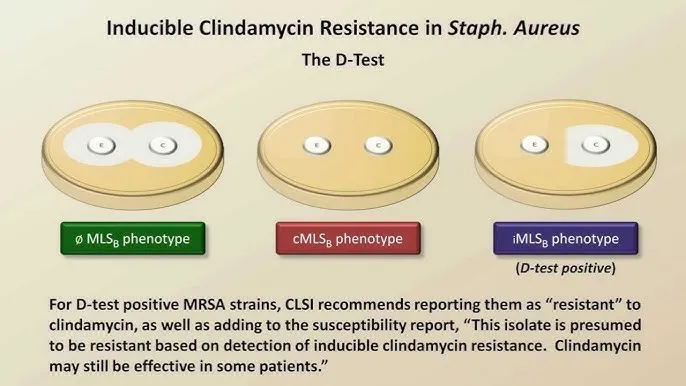
- D-test: Perform if S. aureus is erythromycin-resistant and clindamycin-susceptible to check for inducible clindamycin resistance.
- Suspected MRSA SSTI Management:
- Necrotizing Fasciitis:
- Surgical emergency! Rapidly spreading infection causing extensive soft tissue necrosis.
- Requires prompt, aggressive surgical debridement + broad-spectrum IV antibiotics (e.g., Vancomycin + Piperacillin-Tazobactam + Clindamycin).
- LRINEC score >6 indicates higher likelihood.
- Antibiotic Stewardship: Essential. Use narrowest effective spectrum for appropriate duration.
⭐ For uncomplicated CA-MRSA skin abscesses, incision and drainage (I&D) is the primary treatment; antibiotics are adjunctive and not always necessary.
High‑Yield Points - ⚡ Biggest Takeaways
- Nasal mupirocin for MRSA decolonization prevents recurrent furunculosis.
- Impetigo: Localized treated with topical mupirocin/fusidic acid; Widespread needs oral cephalexin.
- Cellulitis/Erysipelas: Manage with elevation, immobilization, systemic Penicillin (or clindamycin for allergy).
- Abscesses/Furuncles: Incision and Drainage (I&D) is primary; add antibiotics for systemic signs or large lesions.
- Necrotizing Fasciitis: Surgical emergency: prompt aggressive debridement and broad-spectrum IV antibiotics.
- SSI prophylaxis: Cefazolin administered 30-60 minutes before incision prevents infection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

