Lyme Disease - Bug's Beginnings
- Etiology: Spirochetes:
- Borrelia burgdorferi sensu lato complex (main cause):
- B. burgdorferi sensu stricto (N. America)
- B. afzelii, B. garinii (Europe, Asia)
- Borrelia mayonii (N. America, less common)
- Borrelia burgdorferi sensu lato complex (main cause):
- Vector: Transmitted by Ixodes ticks (e.g., deer tick - I. scapularis, I. ricinus, I. persulcatus).

- Reservoirs: Primarily small rodents (e.g., white-footed mice); deer are important tick hosts.
- Epidemiology:
- Endemic in USA (Northeast, Upper Midwest). Increasing incidence in Europe & Asia.
- India: Rare. Awareness crucial for imported cases or potential misdiagnosis.
⭐ Borrelia burgdorferi is a Gram-negative spirochete transmitted by Ixodes ticks.
Word Count: 79
Lyme Disease - Rash Report
- Early Localized Stage (3-30 days post-tick bite): Characterized by:
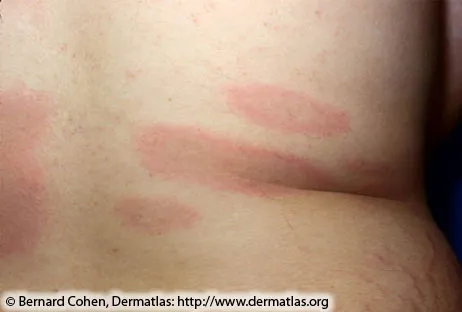
- Erythema Migrans (EM): The hallmark rash.
- Site: Appears at/near tick bite location.
- Appearance: Expanding, annular (ring-like) red patch or macule.
- Classic: Central clearing common, creating a "bull's-eye" (targetoid) appearance.
- Size: Typically enlarges to >5 cm in diameter.
- Symptoms: May feel warm to touch; usually not painful or pruritic.
- 📌 Mnemonic: EM = Expanding Macule.
⭐ Erythema migrans (EM) is the pathognomonic skin lesion of early Lyme disease, seen in 70-80% of US cases.
- Associated Systemic Symptoms (Flu-like):
- Fever, chills, fatigue, headache.
- Myalgias (muscle pain), arthralgias (joint pain).
- Erythema Migrans (EM): The hallmark rash.
Lyme Disease - Spreading Symptoms
Early Disseminated (Weeks to Months)
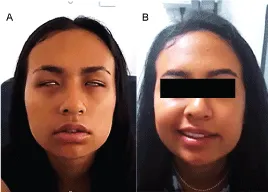
- Neurologic (Lyme Neuroborreliosis - LNB): Aseptic meningitis, cranial neuritis (esp. facial nerve palsy - CN VII, can be bilateral), radiculoneuritis.
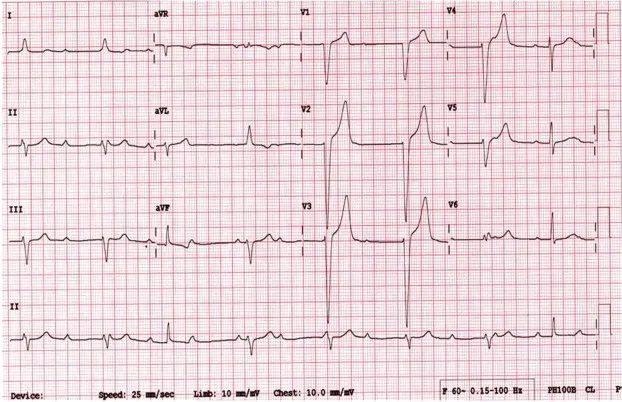
- Cardiac: Carditis (AV block - 1st, 2nd, 3rd degree), myopericarditis.
- Musculoskeletal: Migratory arthralgias/myalgias.
- Ocular: Conjunctivitis, uveitis.
Late Disseminated (Months to Years)
- Arthritis: Mono- or oligoarticular, large joints (esp. knee).
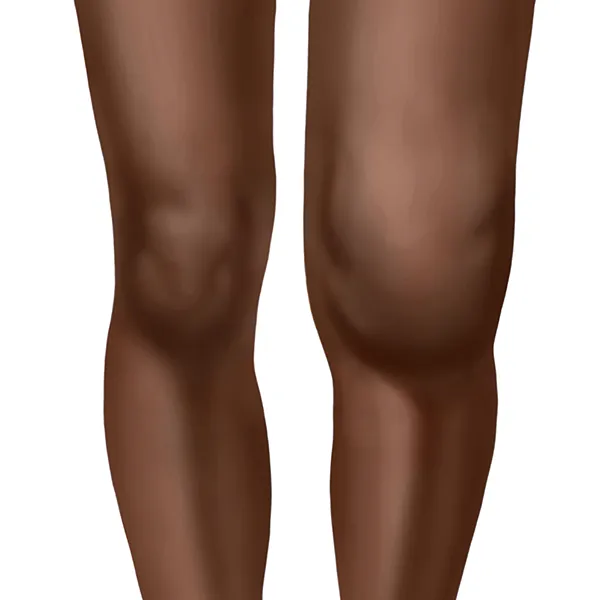
- Chronic LNB: Encephalopathy, polyneuropathy.
- Skin: Acrodermatitis Chronica Atrophicans (ACA) - primarily Borrelia afzelii (Europe).
📌 Mnemonic: 'ABC of Lyme': Arthritis, Bell's Palsy (Facial), Carditis.
⭐ Lyme carditis most commonly manifests as fluctuating degrees of atrioventricular (AV) block.
| System | Early Disseminated (Weeks-Months) | Late Disseminated (Months-Years) |
|---|---|---|
| Neuro | Meningitis, CN VII palsy, radiculoneuritis | Encephalopathy, polyneuropathy |
| Cardiac | Carditis (AV block), myopericarditis | - |
| MSK | Migratory arthralgia/myalgia | Arthritis (esp. knee) |
| Skin | - | Acrodermatitis Chronica Atrophicans (ACA) |
Lyme Disease - Test & Treat Tactics
Diagnosis:
- Clinical: EM endemic = diagnostic.
- Serology (Two-tier): EIA/IFA → Western Blot (IgM/IgG <30d; IgG >30d).
- CSF (LNB): Pleocytosis, intrathecal Ab.
- PCR: Biopsy (EM), CSF, synovial (low blood sensitivity).
⭐ For Lyme disease diagnosis, serologic tests are not recommended for patients with EM if they reside in a high-prevalence area, as diagnosis is clinical; testing may be falsely negative early on.
CDC Two-Tier Serological Testing:
Treatment Regimens:
| Manifestation | Drug(s) of Choice (Dose) | Duration | Alternatives (Child/Preg) |
|---|---|---|---|
| Early Localized | Doxycycline (100mg BID) | 10-21d | Amoxicillin, Cefuroxime |
| Neuro (Facial Palsy) | Doxycycline (100mg BID) | 14-21d | Amoxicillin, Cefuroxime |
| Severe Neuro/Cardiac | IV Ceftriaxone (2g OD) | 14-28d | IV Pen G, IV Cefotaxime |
| Arthritis | Doxycycline (100mg BID) / Amox (500mg TID) | 28d | Amox, Cefuroxime. Refractory: IV Ceftriaxone |
Prophylaxis:
- Doxycycline 200mg (1 dose): tick ≥36h, high-risk, within 72h removal.
PTLDS:
- Persistent symptoms; unclear mechanism; no prolonged antibiotics.
High‑Yield Points - ⚡ Biggest Takeaways
- Causative agent: Borrelia burgdorferi, a spirochete.
- Vector: Transmitted by Ixodes ticks (deer ticks).
- Stage 1 (Early Localized): Hallmark is Erythema migrans (targetoid or bull's-eye rash).
- Stage 2 (Early Disseminated): Neurologic (e.g., bilateral Bell's palsy, meningitis) and cardiac (e.g., AV block) manifestations.
- Stage 3 (Late Disease): Arthritis (especially large joints like the knee) is common; chronic encephalopathy.
- Diagnosis: Clinical diagnosis supported by two-tier serology (ELISA followed by Western blot).
- Treatment: Doxycycline is standard; Amoxicillin for children/pregnant women. IV Ceftriaxone for severe/late manifestations_.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

