CTB: Introduction & Classification - Skin's Silent Siege
Cutaneous Tuberculosis (CTB): Chronic, specific skin infection by Mycobacterium tuberculosis complex (MTBC). Incidence varies with systemic TB prevalence.
Routes of Infection:
- Exogenous: Direct inoculation into skin/mucosa (e.g., trauma, abrasion).
- Endogenous: From an internal TB focus via:
- Haematogenous spread
- Lymphatic extension
- Contiguous spread (e.g., from infected lymph node or bone).
Classification (Simplified):
| Type | Origin & Pathogenesis | Common Examples |
|---|---|---|
| Exogenous | Direct inoculation (low immunity host) | Tuberculous chancre, Tuberculosis verrucosa cutis (TVC) |
| Endogenous | Spread from internal focus (variable immunity) | Lupus vulgaris (LV), Scrofuloderma, Orificial TB, Acute miliary TB |
| Tuberculids | Hypersensitivity to M.tb antigens (strong immunity) | Papulonecrotic tuberculid (PNT), Lichen scrofulosorum, Erythema induratum |
⭐ Lupus vulgaris, the most common CTB form, classically shows "apple-jelly" nodules (yellowish-brown lupus follicles) on diascopy.
CTB Forms (1): Lupus Vulgaris & Scrofuloderma - Lesions Unmasked
- Lupus Vulgaris (LV)
- Most common CTB in India; chronic, progressive, paucibacillary. Often on face.
- Source: Hematogenous, lymphatic, direct extension.
- Lesions: Reddish-brown, soft plaques/nodules; active border, central atrophic scarring.
- Diascopy: "Apple-jelly" nodules (yellowish-brown). (📌 AJELLY: Apple JElly LupY).
- Sites: Face (nose, cheeks, earlobes), neck, extremities.
- Complications: Disfigurement, contractures, ↑ risk SCC (Marjolin's ulcer) in chronic lesions.

- Scrofuloderma (SD)
- Subcutaneous TB; from underlying focus (lymph node, bone, joint).
- Lesions: Firm, painless nodules → soften, adhere to skin → ulcers & discharging sinuses.
- Overlying skin: Bluish-red/violaceous.
- Features: "Cord-like" tracts, keloidal/puckered scars.
- Sites: Neck (cervical lymphadenitis - common), axilla, groin.
⭐ "Apple-jelly" nodules on diascopy are a hallmark of Lupus Vulgaris.
CTB Forms (2): TBVC, Gumma & Tuberculids - Diverse Disguises
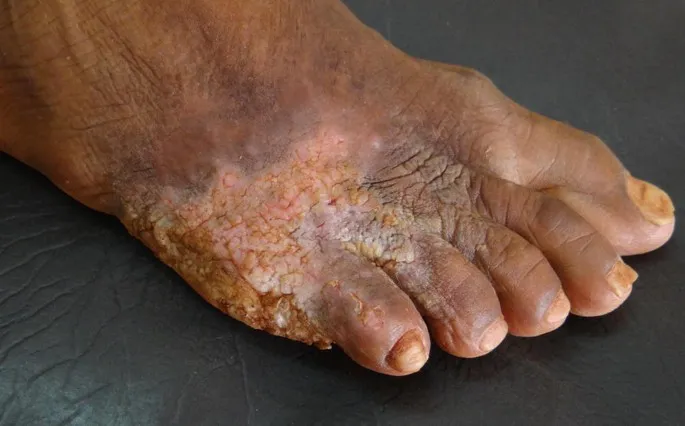
- Tuberculosis Verrucosa Cutis (TBVC)
- Warty, hyperkeratotic plaques ("butcher's/prosector's wart").
- Sites: Hands, buttocks, knees (trauma).
- Patho: Exogenous reinfection in sensitized (high immunity).
- AFB: Scanty. Histo: Pseudoepitheliomatous hyperplasia.
- Tuberculous Gumma (Metastatic Abscess)
- Subcutaneous nodules → cold abscess → ulcers, sinuses.
- Patho: Hematogenous spread from internal focus.
- Often in immunocompromised. AFB: May be positive.
- Tuberculids (Hypersensitivity Reactions)
- Symmetrical eruptions; immune reaction to M. tb antigens.
- AFB: Absent in lesions. Tuberculin test: Strongly positive. Respond to ATT.
- Types:
- Papulonecrotic Tuberculid (PNT): Crusted papules → varioliform scars. Extensors.
- Lichen Scrofulosorum: Minute, grouped, lichenoid papules. Trunk. Asymptomatic.
- Erythema Induratum of Bazin (EIB): Tender nodules, posterior calves; may ulcerate. Nodular vasculitis.
⭐ EIB is strongly associated with an underlying tuberculous focus, often occult; requires ATT.
CTB: Diagnosis & Management - Cracking & Conquering
- Diagnosis:
- Mantoux test: Usually positive (PPD).
- Skin Biopsy: Cornerstone for confirmation.
- HPE: Tuberculoid granulomas; caseation varies.
- AFB stain (ZN): Often negative (paucibacillary forms).
- Culture (LJ): Gold standard, low sensitivity.
- TB-PCR: Rapid, aids early diagnosis.
- Management:
- Multi-drug Anti-Tubercular Therapy (ATT).
- Regimen (New Cases): 2 months (HRZE) + 4 months (HR).
- H: Isoniazid 5 mg/kg
- R: Rifampicin 10 mg/kg
- Z: Pyrazinamide 25 mg/kg
- E: Ethambutol 15 mg/kg
- Surgery: Adjunctive for specific lesions (e.g., non-healing ulcers, sinuses).
⭐ Rifampicin is pivotal in ATT, offering potent bactericidal and sterilizing effects against M. tuberculosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Lupus vulgaris is the most common form of cutaneous TB, presenting with apple-jelly nodules on diascopy.
- Scrofuloderma arises from direct extension of underlying tuberculous foci, commonly lymph nodes or bones.
- Tuberculosis verrucosa cutis (TBVC) is a warty plaque from exogenous inoculation in previously sensitized individuals.
- Erythema induratum of Bazin is a nodular vasculitis or lobular panniculitis, often on the posterior calves.
- Diagnosis involves biopsy for granulomas, AFB staining, and PCR for M. tuberculosis.
- Standard Anti-Tuberculous Therapy (ATT) is the mainstay of treatment for all forms.
- BCG-osis can occur post-vaccination in immunocompromised individuals, presenting as a localized or disseminated infection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

