Pilosebaceous Unit - Acne's Ground Zero
- PSU: Skin unit where acne originates.
- Comprises:
- Hair Follicle: Infundibulum (upper part) is key.
- Lined by keratinocytes; site of acne's hyperkeratinization.
- Sebaceous Gland: Attached to follicle.
- Produces sebum (lipids: triglycerides, wax esters, squalene).
- Holocrine secretion; activity androgen-influenced.
- Hair Follicle: Infundibulum (upper part) is key.
- Distribution: Face, chest, upper back (high PSU density).
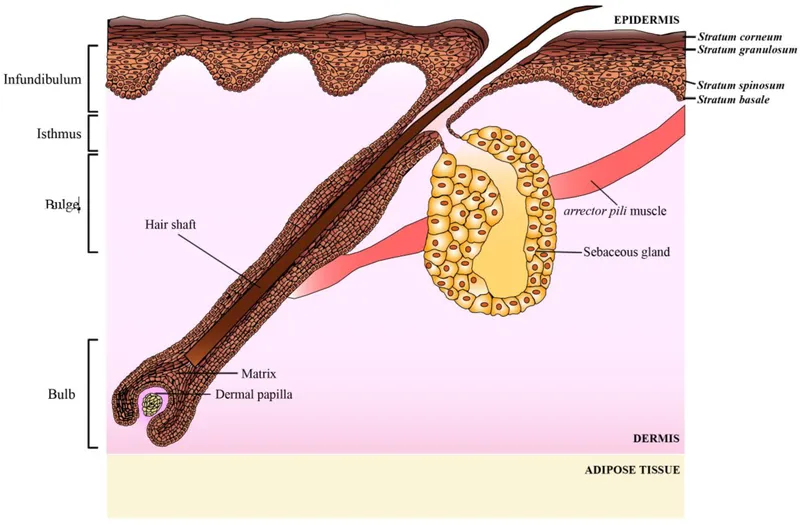
⭐ All primary pathological events of acne (follicular hyperkeratinization, sebum overproduction, C. acnes proliferation, inflammation) occur within the pilosebaceous unit.
Sebum Hypersecretion - Oily Overload
- Key pathogenic factor: ↑ sebum output from hypertrophied sebaceous glands.
- Primary Hormonal Drivers:
- Androgens (esp. Dihydrotestosterone - DHT): Major stimulants, ↑ gland size & activity. Active during puberty.
- Insulin-like Growth Factor-1 (IGF-1): Synergizes with androgens.
- Other factors: CRH, neuropeptides (e.g., Substance P).
- Sebum Alterations:
- ↑ Quantity (oily skin/seborrhea).
- ↓ Linoleic acid: May promote comedogenesis & inflammation.
- Creates lipid-rich anaerobic environment favouring Cutibacterium acnes proliferation.
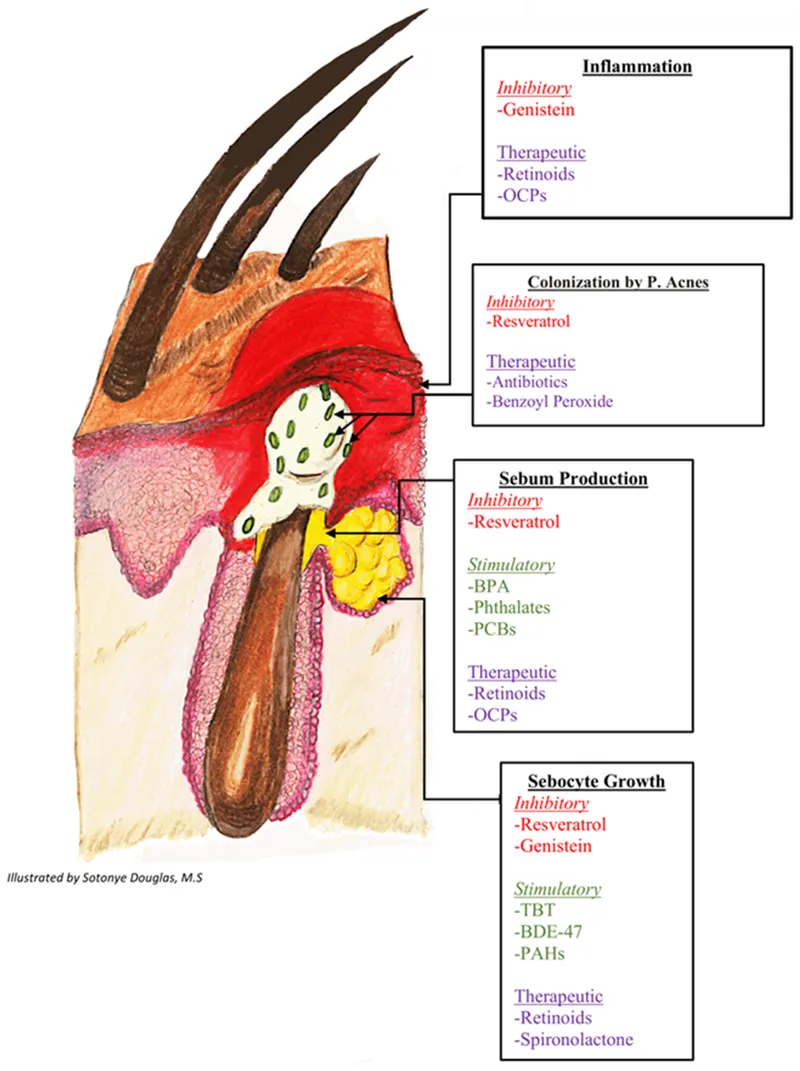
⭐ Androgens, particularly dihydrotestosterone (DHT), are the primary stimulants of sebum production. They bind to receptors in sebocytes, increasing gland size and sebum output.
Follicular Hyperkeratinization - Pore Plug Panic
- Core Problem: Dysregulation of keratinocyte proliferation and differentiation in the follicular infundibulum. This leads to an overproduction and inadequate shedding of keratinocytes.
- Mechanism of Obstruction:
- Keratinocytes become more cohesive (sticky).
- Shed corneocytes accumulate instead of being expelled.
- This forms a dense plug, obstructing the pilosebaceous duct.
- Result: The Microcomedone
- This initial plug is the microcomedone.
⭐ The microcomedone is the primary, non-inflammatory, and clinically invisible precursor to all acne lesions.
- Contributing Factors:
- Androgenic stimulation.
- Local cytokines (e.g., IL-1α).
Cutibacterium acnes - Bug's Life, Acne Style
- Gram-positive, anaerobic/microaerophilic rod; normal skin commensal.
- Colonizes pilosebaceous follicles; proliferates in lipid-rich sebum.
- Key pathogenic roles:
- Hydrolyzes sebum triglycerides via lipases → pro-inflammatory free fatty acids (FFAs) & comedogenic byproducts.
- Releases chemotactic factors & enzymes, attracting neutrophils & promoting follicular rupture.
- Forms biofilms, potentially increasing persistence & treatment resistance.
⭐ Cutibacterium acnes (formerly Propionibacterium acnes) stimulates inflammation by activating Toll-like receptor 2 (TLR-2) on immune cells and keratinocytes.
Inflammation & Immune Response - Red Alert Rampage
- C. acnes surface proteins & metabolic byproducts (e.g., porphyrins, lipases) act as potent chemoattractants and antigens.
- Activation of innate immunity: Toll-like receptors (TLR-2 on keratinocytes, macrophages) recognize C. acnes.
- Release of pro-inflammatory cytokines (IL-1α, IL-8, TNF-α, IL-12) & chemokines, attracting neutrophils.
- Neutrophils phagocytose C. acnes, releasing lysosomal enzymes & ROS, causing follicular wall rupture and dermal inflammation.
- Adaptive immune response: T-cells (Th1, Th17) and B-cells contribute to chronic inflammation and lesion persistence.
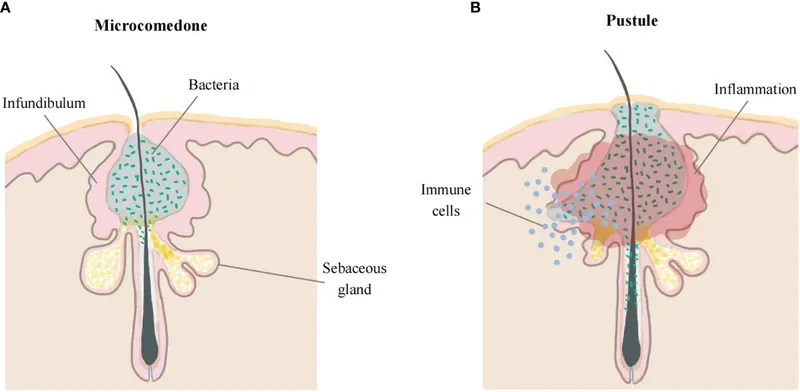
⭐ C. acnes activates the NLRP3 inflammasome, boosting IL-1β production and inflammation significantly.
High-Yield Points - ⚡ Biggest Takeaways
- Follicular hyperkeratinization (abnormal desquamation) forms microcomedones, the precursor lesion.
- Increased sebum production, stimulated by androgens, creates a lipid-rich follicular milieu.
- Cutibacterium acnes (P. acnes), an anaerobe, proliferates within these blocked follicles.
- C. acnes metabolizes sebum, releasing pro-inflammatory mediators and chemotactic factors.
- Host immune response (innate & adaptive) causes inflammation (papules, pustules, nodules).
- Genetic predisposition strongly influences acne susceptibility and severity.
- High glycemic load diets may exacerbate acne in some individuals.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

