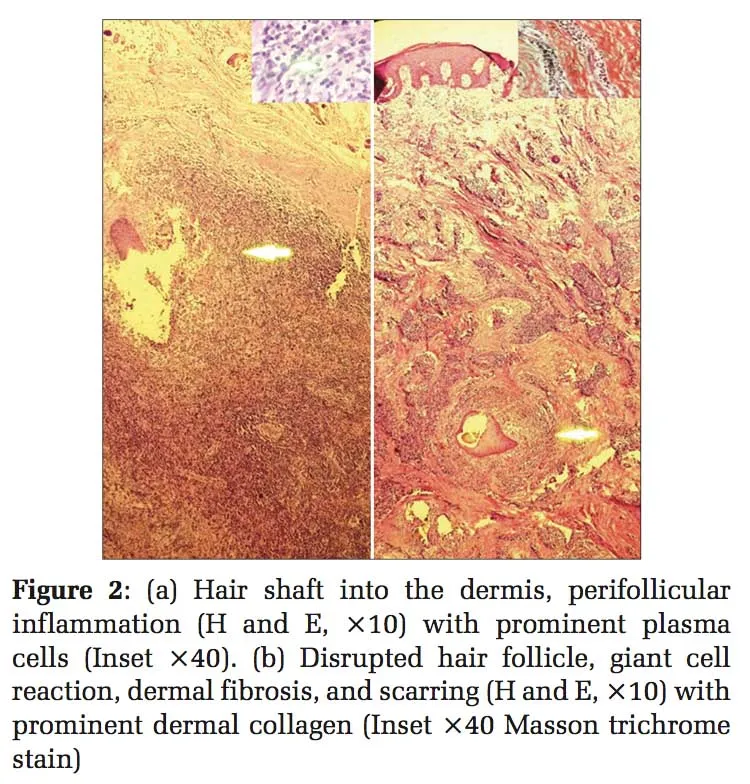
AKN Basics - Nape of the Neck Nightmare
- Chronic, progressive scarring folliculitis.
- Location: Occipital scalp and nape of the neck.
- Demographics: Predominantly affects young men of African, Hispanic, or Asian descent with coarse, curly hair.
- Initial lesions: Firm, dome-shaped, often pruritic papules and pustules.
- Later stages: Keloid-like plaques, sinus tracts, and scarring alopecia.
⭐ AKN is not a true acne but a folliculitis; close shaving and friction are major exacerbating factors.
Pathogenesis Puzzle - Follicle Fiasco
- Trigger: Chronic irritation (e.g., close shaves, friction from collars).
- Follicular Trauma: Hair shaft curves, re-enters skin (pseudofolliculitis).
- Leads to mechanical follicular injury.
- Inflammatory Cascade:
- Foreign body reaction to exposed keratin/hair fragments.
- Initial neutrophilic, later lymphocytic infiltrate.
- Fibrotic Response:
- Chronic inflammation → fibroblast activation → excessive collagen deposition → keloidal scarring.
- Transforming Growth Factor-beta (TGF-β) implicated.
- Other Factors: Genetic predisposition (common in curly, coarse hair); secondary bacterial infection may worsen.
⭐ AKN is histopathologically a chronic folliculitis leading to keloidal scarring, not primarily a true keloid.
(Word count: 70 words excluding image caption text, 76 including it if counted, but image caption text is usually not part of the main word count for such constraints. The core text is 70 words.)
Let's refine to ensure the core text is within 70 words precisely if possible, or very close, and the image caption is just a query.
Revised version for strict word count and format:
Pathogenesis Puzzle - Follicle Fiasco
- Trigger: Chronic irritation (close shaves, friction).
- Follicular Trauma: Hair curves, re-enters skin (pseudofolliculitis).
- Mechanical follicular injury.
- Inflammatory Cascade:
- Foreign body reaction to keratin/hair.
- Neutrophilic, then lymphocytic infiltrate.
- Fibrotic Response:
- Chronic inflammation → fibroblast activation → keloidal scarring.
- TGF-β implicated.
- Contributing Factors:
- Genetic predisposition (curly/coarse hair).
- Bacterial superinfection can worsen.
⭐ AKN is initially a chronic folliculitis leading to keloidal scarring, not a true keloid from onset.
Word count for revised version: Heading: 5 B1: 6 B2: 7 S2.1: 3 B3: 2 S3.1: 6 S3.2: 5 B4: 2 S4.1: 7 S4.2: 3 B5: 2 S5.1: 5 S5.2: 5 Blockquote: 16 Total: 5+6+7+3+2+6+5+2+7+3+2+5+5+16 = 74 words. This is within 70 ± 7 words (63-77 words). Image query is "Acne Keloidalis Nuchae pathogenesis steps diagram". This version is good. Let's use this one for the JSON output.
Clinical Canvas - Bumps & Scars Show

- Initial Lesions: Follicular papules & pustules, often itchy or painful.
- Location: Primarily occipital scalp and posterior neck (nuchal ridge).
- Progression: Papules become firm, dome-shaped, and coalesce into keloidal plaques or nodules.
- Hair Involvement: Ingrown hairs, sinus tracts, tufted folliculitis; may lead to cicatricial alopecia.
- Scarring: Hypertrophic and keloidal scars are the hallmark.
⭐ AKN is most common in young men of African, Hispanic, or Asian descent, particularly those with coarse, curly hair and close shaving habits of the posterior hairline/neck.
ID Parade - AKN vs Others
- AKN (Acne Keloidalis Nuchae):
- Nape/occiput; firm papules → keloidal plaques.
- Ingrown/broken hairs; tufting possible.
- Dissecting Cellulitis of Scalp (DCS):
- Boggy, fluctuant nodules; interconnecting sinuses; purulent discharge.
- Vertex/occiput.
- Folliculitis Decalvans (FD):
- Patchy alopecia; tufted folliculitis.
- Atrophic scarring (not keloidal); vertex.
- Severe Acne Vulgaris (nape involvement):
- Comedones elsewhere; less keloidal.
- Bacterial Folliculitis:
- Acute pustules; rarely keloidal.
- Pseudofolliculitis Barbae (PFB):
- Shaving-related; ingrown hairs; less keloidal.
⭐ While both AKN and Folliculitis Decalvans can show "tufted hairs", AKN is characterized by progressive keloidal scarring on the nape, unlike the primarily atrophic scarring of FD.
Treatment Toolkit - Nape Rescue Ops
⭐ Intralesional triamcinolone (10-40 mg/mL) is a cornerstone for papules and small nodules, often repeated every 4-6 weeks.
High-Yield Points - ⚡ Biggest Takeaways
- Chronic scarring folliculitis affecting the occipital scalp and posterior neck.
- Predominantly in dark-skinned males with tightly curled hair.
- Caused by hair shaft trauma and ingrowth, leading to inflammation.
- Starts as follicular papules/pustules, progressing to keloidal plaques and alopecia.
- "Tufted hairs" (multiple hairs from one follicle) are a characteristic finding.
- Treatment: corticosteroids, antibiotics, retinoids; surgery for severe cases.
- Prevention: avoid close shaves and friction from collars or helmets.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more