Rural Infra Overview - Bedrock of Wellbeing
- Essential for delivering primary healthcare to rural populations, ensuring equity and accessibility. Forms the backbone of public health services.
- Key Components (IPHS Norms):
- Sub-Centre (SC): Most peripheral; health education, MCH, immunisation.
- Primary Health Centre (PHC): First doctor contact; basic curative & preventive care.
- Community Health Centre (CHC): First referral unit (FRU); specialist services, inpatient care.
- Core Challenges: Inadequate human resources, poor connectivity & infrastructure, irregular supplies, maintenance issues, weak referral linkages.
⭐ A Community Health Centre (CHC) is designed to cover a population of 1,20,000 in plain areas and 80,000 in hilly/tribal/difficult areas, serving as a First Referral Unit (FRU).
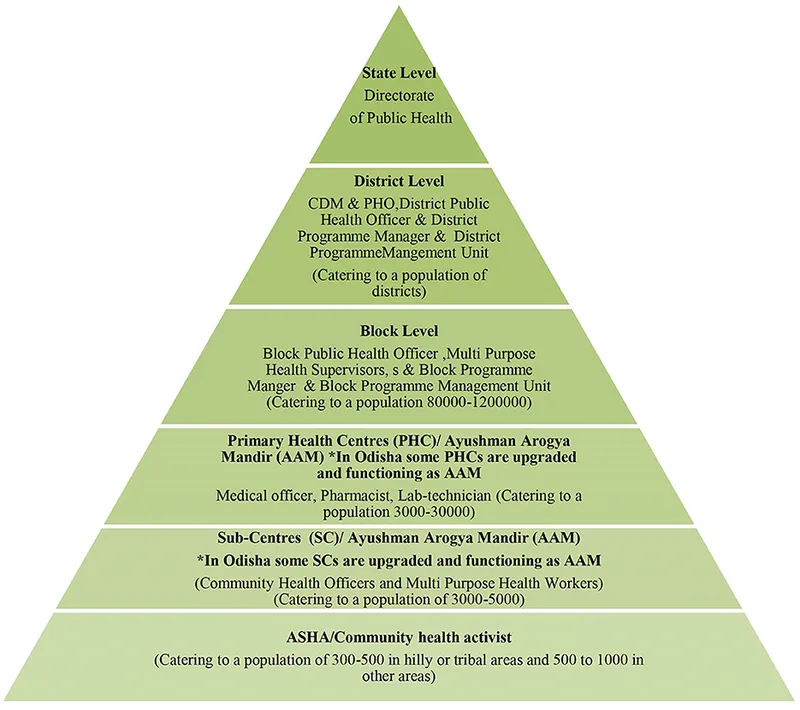
3-Tier System - The Rural Care Ladder
| Feature | Sub-Centre (SC) | Primary Health Centre (PHC) | Community Health Centre (CHC) |
|---|---|---|---|
| Population Norms | Plain: 5000 Hilly/Tribal: 3000 | Plain: 30000 Hilly/Tribal: 20000 | Plain: 120000 Hilly/Tribal: 80000 |
| Staff (Key) | ANM (1), MPW(M) (1) | MO (1), Pharmacist, Nurse, Lab Tech. (Total ~15) | Specialists (4: Surg, Phys, Gyn, Paed), MOs (Total ~25-55) |
| Beds | 2 (Type A for delivery) / 0 (Type B) | 4-6 | 30 |
| Key Services | MCH, FP, Immunization, Basic curative, Referral. | OPD, 24x7 Emergency & Delivery, MTP, National Health Prog., Lab. | Specialist care, Surgery (incl. C-section), Blood storage, X-ray, Lab. |
| Referral Unit For | - | 4-6 Sub-Centres | 4 PHCs |
IPHS & Referrals - Quality & Flow
- IPHS (Indian Public Health Standards): Define quality benchmarks for public health facilities (SC, PHC, CHC) to ensure standardized care.
- Specify essential norms for: Services, Manpower (e.g., 1 MO at PHC 24x7), Equipment, Drugs, Infrastructure.
- Goal: Ensure acceptable quality of care, patient rights & accountability.
- Referral System: Structured, functional pathway for seamless patient transfer between levels.
- Ensures continuum of care & timely access; two-way (upward for complexity, downward for follow-up).
- ASHA: Key community link; facilitates referrals, accompanies patients, promotes health service utilization.
- Referral Flow:
⭐ A CHC designated as an FRU must provide 24x7 services for emergency obstetric and newborn care, including surgical interventions like C-sections.
Rural Schemes & Challenges - Boosting & Bottlenecks
- Boosting Initiatives:
- National Health Mission (NHM): Umbrella program.
- NRHM (2005): Strengthens rural systems; ASHA, JSY, JSSK.
- Ayushman Bharat (2018):
- Health & Wellness Centres (HWCs): Comprehensive primary care.
- PM-JAY: Insurance for hospitalization.
- National Health Mission (NHM): Umbrella program.
- Persistent Bottlenecks:
- Manpower: Shortage, maldistribution.
- Infrastructure: Poor infra, equipment, supply.
- Accessibility: Geographic, social, financial barriers.
- Quality of Care: Variable standards.
⭐ Janani Shishu Suraksha Karyakram (JSSK) ensures free delivery (incl. C-section) in public facilities for pregnant women.
High‑Yield Points - ⚡ Biggest Takeaways
- Sub-Centre (SC): First contact point; 1 per 5000 (plains) / 3000 (hilly/tribal).
- Primary Health Centre (PHC): Referral unit for 6 SCs; 1 per 30,000 (plains) / 20,000 (hilly/tribal).
- Community Health Centre (CHC): Referral unit for 4 PHCs; 1 per 1,20,000 (plains) / 80,000 (hilly/tribal); 4 specialists, 30 beds.
- ASHA (Accredited Social Health Activist): Community health volunteer; 1 per 1000 population.
- NRHM (2005), now under NHM, aimed to strengthen rural health infrastructure.
- The three-tier system (SC, PHC, CHC) is fundamental to rural healthcare delivery in India.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

