Rural Health

On this page
🏥 Rural Health Infrastructure: The Bedrock of Village Wellness
Rural health infrastructure determines whether millions receive timely care or face preventable suffering, yet India's villages confront persistent gaps in facilities, standards, and service delivery. You'll explore how the three-tier system functions, master IPHS benchmarks that define quality, and examine why monitoring and innovation matter when distance and resources create unique obstacles. This lesson equips you to understand both the structural realities and transformational possibilities that shape healthcare access for over 65% of India's population.
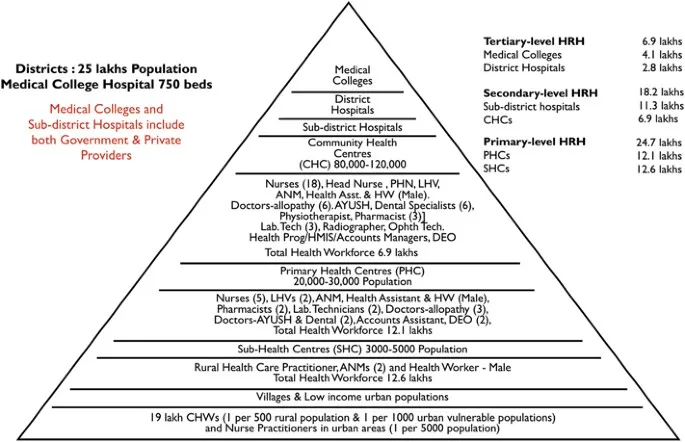
India's rural health infrastructure operates as a meticulously engineered three-tier system, designed to deliver comprehensive healthcare from village doorsteps to district hospitals. This architectural marvel serves 833 million rural Indians through 1.58 lakh Sub Health Centers, 25,650 Primary Health Centers, and 5,624 Community Health Centers, creating the world's largest rural healthcare network.
📌 Remember: SPC - Sub-centers serve 3,000-5,000 population, PHCs cover 20,000-30,000 people, CHCs manage 80,000-1.2 lakh population with 30-bed capacity and 4 specialists
The foundation tier consists of Sub Health Centers (SHCs), positioned as the first contact point between rural communities and formal healthcare. Each SHC covers 3,000-5,000 population in plains and 3,000 in hilly/tribal areas, staffed by 1 ANM and 1 Male Health Worker. These centers provide immunization, antenatal care, treatment of minor ailments, and health education to 80% of India's rural population.
- Sub Health Centers Architecture
- Coverage: 3,000-5,000 population (plains), 3,000 (hilly/tribal)
- Staffing: 1 ANM + 1 Male Health Worker
- Services: Immunization (85% coverage), ANC (76% registration)
- Minor ailment treatment: 60-70% of rural health needs
- Health education: 100% villages covered
- Drug distribution: Essential Drug List of 34 medicines
Primary Health Centers form the operational backbone, providing curative, preventive, and promotive healthcare services. Each PHC serves 20,000-30,000 population with 6-bed indoor facility, 1 Medical Officer, 14 paramedical staff, and 24x7 delivery services. PHCs achieve institutional delivery rates of 88.6% and conduct 2.5 lakh deliveries annually across the network.
⭐ Clinical Pearl: PHCs handle 70% of rural healthcare needs, with Medical Officers managing 50-60 OPD cases daily and conducting 8-10 deliveries monthly per center
Community Health Centers represent the apex of rural healthcare, providing specialist care and emergency services. Each CHC covers 80,000-1.2 lakh population with 30-bed capacity, 4 specialists (Medicine, Surgery, Obstetrics, Pediatrics), operation theater, X-ray, and laboratory facilities. CHCs perform 60% of rural surgeries and handle emergency referrals for 15% of rural patients.
| Infrastructure Tier | Population Coverage | Bed Capacity | Specialist Staff | Key Services | Achievement Rate |
|---|---|---|---|---|---|
| Sub Health Center | 3,000-5,000 | 0 | ANM + MHW | Immunization, ANC | 85% coverage |
| Primary Health Center | 20,000-30,000 | 6 beds | 1 Medical Officer | Delivery, OPD | 88.6% institutional delivery |
| Community Health Center | 80,000-1.2 lakh | 30 beds | 4 Specialists | Surgery, Emergency | 60% rural surgeries |
| District Hospital | 10-20 lakh | 100-300 beds | All Specialists | Tertiary care | 95% referral acceptance |
| Medical College | State level | 500+ beds | Super specialists | Teaching + Tertiary | 100% critical care |
Connect this foundational infrastructure through Indian Public Health Standards (IPHS) to understand quality benchmarks that transform basic facilities into centers of clinical excellence.
🏥 Rural Health Infrastructure: The Bedrock of Village Wellness
🎯 IPHS Standards: The Quality Command Center
IPHS represents India's comprehensive quality framework, launched in 2012 and revised in 2022, establishing minimum standards for infrastructure, manpower, equipment, and services across all rural health facilities. These standards ensure uniform quality across 1.9 lakh rural health facilities, creating measurable benchmarks for clinical care, patient safety, and service delivery.
📌 Remember: IPHS-MESS - Infrastructure, Personnel, Healthcare, Services standards with Minimum Essential Service Standards ensuring 24x7 emergency care, skilled birth attendance, and drug availability >80%
Infrastructure Standards define precise specifications for building design, space allocation, and utility requirements. SHCs require minimum 3 rooms with 150 sq ft consultation area, PHCs need 8 rooms with 1,200 sq ft total area, and CHCs mandate 20 rooms with 4,000 sq ft space including operation theater and laboratory facilities.
- IPHS Infrastructure Specifications
- SHC: 3 rooms, 150 sq ft consultation, 24-hour electricity backup
- PHC: 8 rooms, 1,200 sq ft, labor room, minor OT, pharmacy
- Water supply: 24x7 availability with storage capacity
- Waste management: Color-coded segregation, biomedical waste disposal
- Accessibility: Ramp access, disabled-friendly facilities
- CHC: 20 rooms, 4,000 sq ft, major OT, X-ray room, blood storage
Equipment Standards ensure diagnostic capability and treatment readiness across all facility levels. PHCs require 56 essential equipment items including ECG machine, autoclave, delivery kit, and emergency drugs. CHCs mandate 120+ equipment items including X-ray machine, operation table, anesthesia machine, and blood bank refrigerator.
⭐ Clinical Pearl: IPHS equipment compliance reaches 78% at PHC level and 65% at CHC level, with diagnostic equipment availability directly correlating to 30% reduction in referral rates and 25% improvement in patient satisfaction scores
Manpower Standards specify exact staffing patterns with qualification requirements and service responsibilities. PHCs require 1 Medical Officer (MBBS), 1 Staff Nurse (GNM), 1 ANM, 1 Pharmacist, and 11 support staff. CHCs mandate 4 specialists, 6 staff nurses, 2 ANMs, 1 radiographer, and 15 support staff for 24x7 operations.
| Facility Type | Medical Staff | Nursing Staff | Support Staff | Specialist Requirements | Service Hours |
|---|---|---|---|---|---|
| SHC | 1 ANM, 1 MHW | 1 ANM | 1 Attendant | None | 6 hours/day |
| PHC | 1 Medical Officer | 1 Staff Nurse, 1 ANM | 11 Support staff | MBBS mandatory | 24x7 emergency |
| CHC | 4 Specialists | 6 Staff Nurses, 2 ANMs | 15 Support staff | Medicine, Surgery, OBG, Pediatrics | 24x7 full services |
| District Hospital | 15+ Specialists | 50+ Nurses | 100+ Support | All major specialties | 24x7 tertiary care |
| Medical College | 100+ Faculty | 200+ Nurses | 300+ Support | Super specialists | Teaching + Clinical |
Connect these quality standards through service delivery protocols to understand how standardized care transforms rural health outcomes.
🎯 IPHS Standards: The Quality Command Center
🚀 Service Delivery Excellence: The Rural Care Engine
Comprehensive Service Delivery encompasses preventive, curative, and promotive healthcare through standardized protocols and evidence-based interventions. Rural facilities provide 12 essential service packages including maternal health, child health, immunization, family planning, communicable disease control, and emergency care with quality indicators and performance targets.
📌 Remember: PRIME-CD - Preventive, Reproductive, Immunization, Maternal, Emergency services plus Communicable Disease control form the 6 core service pillars with >90% coverage targets and 24x7 emergency availability
Maternal Health Services achieve institutional delivery rates of 88.6% through skilled birth attendance, emergency obstetric care, and comprehensive ANC. PHCs conduct 4+ ANC visits for 76% of pregnant women, provide iron-folic acid supplementation to 85%, and ensure 48-hour postpartum stay for 92% of deliveries with maternal mortality reduction of 60% since 2000.
- Maternal Health Service Metrics
- ANC Registration: 76% in first trimester, 4+ visits completion
- Institutional Delivery: 88.6% overall, 95% in aspirational districts
- Emergency Obstetric Care: 24x7 availability at CHC level
- Skilled Birth Attendance: 89% deliveries by trained personnel
- Postpartum Care: 48-hour stay, 6-week follow-up
- High-Risk Pregnancy: 15% identification, specialized care referral
Child Health Services deliver Universal Immunization Program achieving 85% full immunization coverage, Integrated Management of Neonatal and Childhood Illness (IMNCI) protocols, and nutritional rehabilitation. Rural facilities provide growth monitoring for 78% children, vitamin A supplementation for 89%, and treatment of severe acute malnutrition with >85% cure rates.
⭐ Clinical Pearl: IMNCI protocols reduce under-5 mortality by 40% through systematic assessment of danger signs, classification of illness severity, and appropriate treatment or referral decisions with <2 minutes assessment time per child
Emergency Care Services provide 24x7 availability at PHC and CHC levels with first aid, stabilization, and referral protocols. Rural facilities handle trauma care, obstetric emergencies, cardiac events, and poisoning cases with golden hour compliance of 78% and referral completion rates of 92% for critical patients.
| Service Category | Coverage Target | Achievement Rate | Quality Indicators | Performance Metrics |
|---|---|---|---|---|
| Maternal Health | 90% institutional delivery | 88.6% achieved | MMR <70/lakh | 60% reduction since 2000 |
| Child Health | 85% full immunization | 85% achieved | IMR <30/1000 | 67% reduction since 2000 |
| Family Planning | 70% contraceptive prevalence | 67.8% achieved | Unmet need <10% | 12.9% current unmet need |
| Emergency Care | 100% 24x7 availability | 78% compliance | <30 min response | 92% referral completion |
| Communicable Disease | 90% case detection | 82% achieved | <5% treatment default | 85% cure rates |
Connect these service protocols through performance monitoring systems to understand how data-driven management optimizes rural healthcare delivery.
🚀 Service Delivery Excellence: The Rural Care Engine
📊 Performance Monitoring: The Analytics Powerhouse
Health Management Information System (HMIS) serves as the central nervous system for rural health monitoring, collecting monthly data from all health facilities on service delivery, resource utilization, and health outcomes. The system processes 2.5 crore data entries monthly, generating automated reports for facility, block, district, and state levels with real-time performance tracking.
📌 Remember: HMIS-RAPID - Health Management Information System tracks Resources, Activities, Performance, Indicators, Delivery outcomes with monthly reporting, quarterly reviews, and annual assessments ensuring data-driven healthcare management
Key Performance Indicators (KPIs) measure service quality, access, and outcomes across 8 thematic areas. Maternal health indicators include ANC registration rates, institutional delivery percentages, and maternal mortality ratios. Child health metrics track immunization coverage, growth monitoring, and infant mortality rates with district-wise comparisons and trend analysis.
- Critical Performance Metrics Framework
- Access Indicators: Facility availability within 5 km, specialist availability >80%
- Quality Indicators: IPHS compliance >75%, patient satisfaction >85%
- Outcome Indicators: MMR <70/lakh, IMR <30/1000, TFR <2.1
- Process Indicators: ANC 4+ visits, institutional delivery, full immunization
- Input Indicators: Manpower availability, drug stock, equipment functionality
- Impact Indicators: Life expectancy, healthy life years, disease burden reduction
Digital Monitoring Platforms integrate HMIS, Mother and Child Tracking System (MCTS), Reproductive and Child Health (RCH) portal, and Ayushman Bharat Health Account (ABHA) creating unified dashboards. These platforms enable real-time tracking of individual beneficiaries, facility performance, and program outcomes with predictive analytics and early warning systems.
⭐ Clinical Pearl: Real-time monitoring reduces maternal deaths by 25% through high-risk pregnancy tracking, due date alerts, and emergency response coordination with SMS-based follow-up achieving 78% compliance rates
Performance-Based Financing links fund allocation to achievement of targets, incentivizing quality improvement and outcome optimization. Results-Based Financing (RBF) provides additional funding for facilities achieving >90% targets in maternal health, child health, and service quality indicators, resulting in 30% improvement in performance metrics.
| Monitoring System | Data Collection | Reporting Frequency | Key Metrics | Performance Impact |
|---|---|---|---|---|
| HMIS | Monthly facility reports | Monthly/Quarterly | 200+ indicators | 25% improvement in data quality |
| MCTS/RCH | Individual tracking | Real-time updates | Maternal/child outcomes | 30% reduction in dropouts |
| ABHA | Digital health records | Continuous | Service utilization | 40% better care coordination |
| Financial Monitoring | Expenditure tracking | Monthly | Budget utilization | 95% fund utilization |
| Quality Assurance | Facility assessments | Quarterly | IPHS compliance | 35% improvement in standards |
Connect this monitoring framework through infrastructure challenges and solutions to understand how systematic problem-solving strengthens rural healthcare delivery.
📊 Performance Monitoring: The Analytics Powerhouse
⚡ Infrastructure Challenges: The Reality Check Engine
Human Resource Shortages represent the most critical challenge, with rural areas experiencing 70% shortage of doctors and 50% shortage of specialists. CHCs operate with only 65% of required specialists, PHCs function with 83% of medical officers, and ANM positions show 15% vacancy rates. Rural postings face high attrition with 40% of doctors seeking urban transfers within 2 years.
📌 Remember: GAPS-HR - Geographic isolation, Amenity lack, Professional isolation, Salary disparities create Human Resource challenges with 70% doctor shortage, 65% specialist availability, and 40% attrition in rural postings requiring retention strategies
Infrastructure Deficits affect basic facility operations with 35% of SHCs lacking electricity, 28% without water supply, and 45% missing all-weather road connectivity. Equipment functionality remains suboptimal with 40% of diagnostic equipment non-functional, 25% of vehicles out of service, and 30% of facilities lacking internet connectivity for telemedicine and data reporting.
- Critical Infrastructure Gaps
- Power Supply: 35% SHCs without reliable electricity, backup power in <50% facilities
- Water and Sanitation: 28% facilities lack 24x7 water, 40% need sanitation upgrades
- Connectivity: 45% lack all-weather roads, 30% without internet access
- Equipment Status: 40% diagnostic equipment non-functional, maintenance gaps
- Transportation: 25% ambulances out of service, referral delays
- Communication: Limited mobile coverage in 20% areas, emergency coordination challenges
Financial Constraints limit infrastructure development and service expansion with per capita health spending of ₹1,657 compared to global average of ₹74,000. State budget allocations for health remain <6% of total expenditure, while infrastructure maintenance receives <15% of health budgets, creating sustainability challenges.
⭐ Clinical Pearl: Public-Private Partnerships (PPP) in rural infrastructure development achieve 35% cost reduction and 50% faster implementation compared to traditional government procurement, with successful models in Rajasthan, Gujarat, and Karnataka demonstrating scalable solutions
Innovative Solutions address infrastructure challenges through technology integration, alternative service delivery, and community participation. Mobile Health Units extend services to remote areas, telemedicine connects specialists to rural patients, and solar power systems ensure reliable electricity for critical equipment operation.
| Challenge Category | Severity Level | Current Status | Solution Approach | Expected Impact |
|---|---|---|---|---|
| Human Resources | Critical | 70% doctor shortage | MBBS rural quota, incentives | 50% improvement by 2025 |
| Infrastructure | High | 35% power deficit | Solar systems, PPP models | 80% coverage by 2024 |
| Equipment | Moderate | 40% non-functional | AMC contracts, local technicians | 90% functionality target |
| Connectivity | High | 30% no internet | Fiber optic expansion | 95% connectivity by 2025 |
| Financing | Critical | <6% budget allocation | Increased allocation, efficiency | 8% target by 2025 |
Connect these challenge-solution frameworks through future development strategies to understand how strategic planning transforms rural healthcare infrastructure.
⚡ Infrastructure Challenges: The Reality Check Engine
🌟 Future Infrastructure Vision: The Transformation Blueprint
Digital Health Infrastructure forms the backbone of transformation with comprehensive connectivity, electronic health records, and AI-powered decision support systems. National Digital Health Mission (NDHM) creates unified health IDs for all rural beneficiaries, interoperable systems across facility levels, and real-time data analytics enabling predictive healthcare and personalized treatment protocols.
📌 Remember: SMART-RH - Sustainable, Mobile-enabled, AI-powered, Resilient, Technology-integrated Rural Health infrastructure with 100% digital connectivity, paperless operations, and outcome-based service delivery achieving universal health coverage
Hub-and-Spoke Model optimizes resource utilization through strategic facility positioning and service integration. Health and Wellness Centers (HWCs) serve as community hubs providing comprehensive primary care, while specialized services concentrate at CHC clusters serving multiple PHC areas through telemedicine, mobile units, and referral networks.
- Integrated Service Delivery Architecture
- Health and Wellness Centers: 1.5 lakh facilities providing 12 service packages
- Telemedicine Networks: 100% connectivity enabling specialist consultations
- Mobile Health Units: Fleet expansion to 10,000 units covering remote areas
- Emergency Response: 108 ambulance integration with GPS tracking
- Supply Chain: Drone delivery for medicines and vaccines to inaccessible areas
- Quality Assurance: Real-time monitoring through IoT sensors and automated reporting
Sustainable Infrastructure Development incorporates green technologies, renewable energy, and climate-resilient design principles. Solar power systems provide reliable electricity to 100% rural facilities, rainwater harvesting ensures water security, and waste management systems maintain environmental standards while reducing operational costs by 30%.
⭐ Clinical Pearl: Modular Infrastructure Design enables rapid scaling and cost optimization with standardized facility modules reducing construction time by 50% and costs by 35% while ensuring uniform quality and IPHS compliance across all rural health facilities
Community-Centered Care Models strengthen local ownership and sustainability through Village Health Sanitation and Nutrition Committees (VHSNCs), community health volunteers, and social accountability mechanisms. Participatory planning involves communities in facility design, service prioritization, and performance monitoring achieving 85% community satisfaction and improved health outcomes.
| Transformation Component | Implementation Timeline | Investment Required | Expected Outcomes | Sustainability Measures |
|---|---|---|---|---|
| Digital Infrastructure | 2024-2027 | ₹50,000 crore | 100% connectivity | Revenue generation through services |
| Hub-Spoke Model | 2023-2026 | ₹75,000 crore | 40% efficiency gain | Optimized resource utilization |
| Sustainable Systems | 2024-2030 | ₹30,000 crore | 30% cost reduction | Green technology adoption |
| Community Integration | 2023-2025 | ₹15,000 crore | 85% satisfaction | Local ownership models |
| Quality Enhancement | 2024-2028 | ₹40,000 crore | 95% IPHS compliance | Performance-based financing |
🌟 Future Infrastructure Vision: The Transformation Blueprint
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















