Sub-Centers - Tiny Titans of Health
- Peripheral-most, first contact point between primary healthcare system & community.
- Types:
- Type A: For normal areas, delivery services not provided.
- Type B: For difficult/tribal areas, equipped for deliveries.
- Population Norms:
- Plain areas: 1 per 5000 population.
- Hilly/Tribal/Difficult areas: 1 per 3000 population.
⭐ Sub-Centers are pivotal for MCH services, ICDS coordination, and disease surveillance at the grassroots level. They are managed by at least one ANM/Female Health Worker and one Male Health Worker (MPW-M).
The A-Team & Their Abode
- Staffing (IPHS 2022 Norms):
- Health Worker (F) / ANM: 1 (Type A); 2 (Type B: delivery load >20/month or difficult/tribal area).
- Health Worker (M): 1.
- Part-time Sweeper: 1.
- Supervision (1 per 6 SCs): Health Assistant (F)/LHV & Health Assistant (M).
- Abode (Infrastructure & Supplies):
- Building: IPHS standard; ANM residential accommodation.
- Essential Drugs: Kits A & B (ORS, IFA, basic antibiotics, vaccines).
- Equipment: BP apparatus, stethoscope, weighing scales (adult & infant), thermometer, delivery kit, hub cutter.
- Vaccine carriers: 2 per ANM.
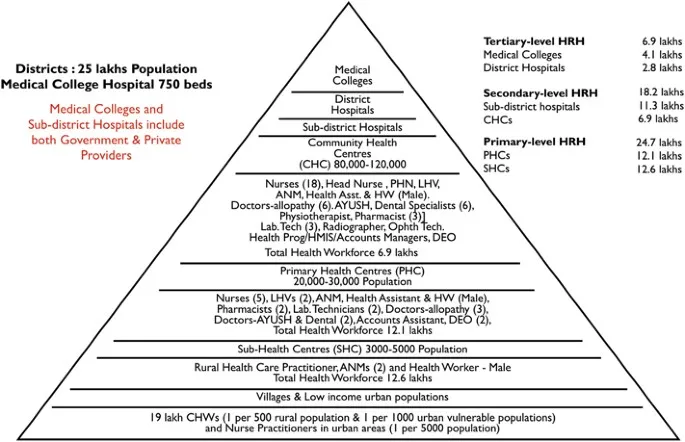
⭐ Sub-Centres are the first contact point between the primary healthcare system and the community.
Health Hub - Services Galore
- Maternal & Child Health (MCH):
- Antenatal Care (ANC): Early reg., min. 4 check-ups, IFA, TT.
- Postnatal Care (PNC): Mother & newborn care.
- Newborn Care: Essential care, basic resuscitation.
- Child Health: Immunization (NIS), growth monitoring, IMNCI (diarrhea, ARI).
- Family Planning & Contraception:
- Counseling, education.
- Provision: Condoms, OCPs, ECPs.
- IUD insertion (trained ANM/SN).
- Disease Surveillance & Control:
- Malaria: Smear collection, RDTs, treatment.
- TB: Sputum collection, DOTS referral.
- Communicable disease outbreak reporting.
- NCD screening (BP, Diabetes) & referral.
- Other Essential Services:
- Minor ailment treatment.
- Health education & counseling.
- Vital statistics (birth/death reg.).
- Referral to PHC/CHC.
- Water quality testing (FTKs).
⭐ Sub-centres provide a defined "Assured Services" package under the National Health Mission (NHM).
Wellness Warriors - Upgraded & Accountable
- Sub-Centres (SCs): Initial community contact for primary healthcare.
- Upgraded to Health & Wellness Centres (HWCs) under Ayushman Bharat (AB-HWC) from 2018.
- Goal: Deliver Comprehensive Primary Health Care (CPHC) near homes.
- Expanded Services (CPHC):
- Original SC services + 12 additional packages.
- Includes: NCD screening (hypertension, diabetes, oral/breast/cervical cancers), elderly care, palliative care, basic mental health, oral/eye/ENT care.
- Key Team:
- ANM (MPW-F), MPW-M.
- Community Health Officer (CHO): MLHP (BSc Nursing/BAMS + CCH), leads HWC-SC.
- Monitoring & Accountability:
- Performance-Linked Incentives (PLI).
- Digital platforms: NCD app, RCH portal, Nikshay.
- Supportive supervision; Jan Arogya Samitis (JAS) for community engagement.

⭐ Population Norms for Sub-Centres: 1 SC per 5000 population (plain areas), 1 SC per 3000 population (hilly/tribal/difficult areas).
High‑Yield Points - ⚡ Biggest Takeaways
- Most peripheral and first contact point for primary healthcare.
- Population norm: 5000 (plains), 3000 (hilly/tribal/difficult areas).
- Key staff: Auxiliary Nurse Midwife (ANM) / Female Health Worker, Male Health Worker.
- Focus on MCH services, immunization, family planning, and disease surveillance.
- Acts as a reporting unit for vital events.
- Upgraded to Health and Wellness Centers (HWCs) under Ayushman Bharat.
- Supervised by the Medical Officer of the respective Primary Health Centre (PHC).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

