Public Health Administration

On this page
🏛️ Administrative Architecture: The Health Governance Blueprint
Public health administration transforms policy vision into population impact through six interconnected systems that determine whether communities thrive or falter. You'll discover how governance structures create accountability, how management principles drive operational excellence, and how coordination mechanisms prevent the silos that undermine care delivery. We'll examine quality assurance frameworks that maintain standards and explore digital transformation tools reshaping modern public health infrastructure. Master these administrative foundations and you'll understand why some health systems succeed while others struggle despite similar resources.
📌 Remember: ADMIN - Accountability systems, Decentralized delivery, Management structures, Intersectoral coordination, National guidelines
Administrative Hierarchy Framework
- National Level (100% policy formulation)
- Ministry of Health & Family Welfare: ₹86,200 crores budget allocation (2023-24)
- Directorate General of Health Services: 15+ technical divisions
- Disease control programs: 12 major initiatives
- Health system strengthening: ₹37,000 crores under NHM
- State Level (85% implementation responsibility)
- State Health Departments: 28 states + 8 UTs coordination
- Medical Education Departments: 596 medical colleges oversight
- MBBS seats: 90,825 annually across India
- PG seats: 64,559 specialty training positions
- District Level (70% service delivery)
- Chief Medical Officers: 741 districts coverage
- District Health Societies: ₹2.5 lakhs average annual budget per facility
| Administrative Level | Budget Authority | Staff Oversight | Population Coverage | Decision Timeline |
|---|---|---|---|---|
| National | ₹86,200+ crores | 50,000+ officers | 1.4 billion | 6-12 months |
| State | ₹5,000-15,000 crores | 10,000-25,000 | 50-200 million | 3-6 months |
| District | ₹200-500 crores | 500-2,000 | 1-5 million | 1-3 months |
| Block | ₹50-150 crores | 100-500 | 100,000-300,000 | 2-4 weeks |
| Village | ₹5-15 lakhs | 5-20 | 3,000-5,000 | 1-2 weeks |
💡 Master This: Administrative efficiency directly correlates with health service delivery - every 10% improvement in governance scores increases immunization coverage by 7% and reduces maternal mortality by 12%
Connect administrative foundations through governance mechanisms to understand accountability frameworks.
🏛️ Administrative Architecture: The Health Governance Blueprint
⚙️ Governance Mechanisms: The Accountability Engine
📌 Remember: GOVERN - Goals setting, Oversight mechanisms, Verification systems, Evaluation protocols, Reporting structures, Normative frameworks
Performance Management Systems
- National Health Mission Monitoring
- 18 key performance indicators tracked monthly
- Common Review Mission: bi-annual comprehensive assessments
- 541 districts evaluated systematically
- Performance scores: 40-95% range across states
- Financial Management Protocols
- Public Financial Management System: 100% digital tracking
- Fund utilization rates: 75-90% across different schemes
- Untied funds: ₹10 lakhs per PHC annually
- Tied funds: ₹25-50 lakhs per CHC for specific programs
- Quality Assurance Frameworks
- National Quality Assurance Standards: 279 standards for different facilities
- LaQshya program: >50% improvement in delivery outcomes
- Cesarean section rates: Reduced from 21.1% to 18.5%
- Maternal mortality: 15% reduction in participating facilities
| Governance Tool | Coverage | Frequency | Impact Measure | Success Rate |
|---|---|---|---|---|
| Common Review Mission | 541 districts | Bi-annual | Performance scores | 78% improvement |
| PFMS Tracking | 100% facilities | Real-time | Fund utilization | 85% efficiency |
| Quality Certification | 25,000+ facilities | Annual | Service standards | 67% compliance |
| Citizen Feedback | All levels | Continuous | Satisfaction scores | 72% positive |
| Audit Systems | 100% schemes | Quarterly | Financial compliance | 91% adherence |
💡 Master This: Effective governance creates predictable health outcomes - districts with >80% governance scores consistently achieve >90% immunization coverage and <30 infant mortality rates
Connect governance frameworks through management principles to understand operational excellence.
⚙️ Governance Mechanisms: The Accountability Engine
🎯 Management Principles: The Operational Excellence Framework
📌 Remember: MANAGE - Monitoring systems, Accountability measures, Needs assessment, Allocation efficiency, Goal achievement, Evaluation protocols
Strategic Planning Frameworks
- District Health Action Plans (DHAP)
- Annual planning cycle: April-March fiscal alignment
- Population-based targets: per 1,000 population metrics
- Birth rate targets: 18-20 per 1,000 population
- Death rate targets: <6 per 1,000 population
- Disease burden reduction: 10-15% annually for priority conditions
- Resource Allocation Models
- Population-based funding: ₹1,200-2,000 per capita health expenditure
- Equity adjustments: 20-40% additional allocation for tribal/remote areas
- High-focus states: 15% additional central funding
- Aspirational districts: ₹50 crores special allocation per district
- Performance-Based Incentives
- Results-Based Financing: ₹500-2,000 per facility based on outcomes
- Quality certification bonuses: 10-25% additional funding for accredited facilities
- NQAS certification: ₹5-15 lakhs bonus per facility
- Kayakalp awards: ₹1-5 lakhs for cleanliness standards
| Management Component | Planning Horizon | Resource Requirement | Success Metric | Achievement Rate |
|---|---|---|---|---|
| Strategic Planning | 5 years | ₹10,000+ crores | Health outcomes | 65% target achievement |
| Annual Action Plans | 1 year | ₹2,000-5,000 crores | Service delivery | 78% completion |
| Quarterly Reviews | 3 months | ₹500-1,000 crores | Process indicators | 85% compliance |
| Monthly Monitoring | 1 month | ₹100-300 crores | Activity targets | 92% reporting |
| Weekly Tracking | 1 week | ₹25-75 crores | Immediate actions | 96% response |
💡 Master This: Management effectiveness multiplies resource impact - every ₹100 invested in management systems generates ₹340 worth of improved health outcomes through efficiency gains
Connect management excellence through coordination mechanisms to understand system integration.
🎯 Management Principles: The Operational Excellence Framework
🔗 Coordination Mechanisms: The Integration Architecture
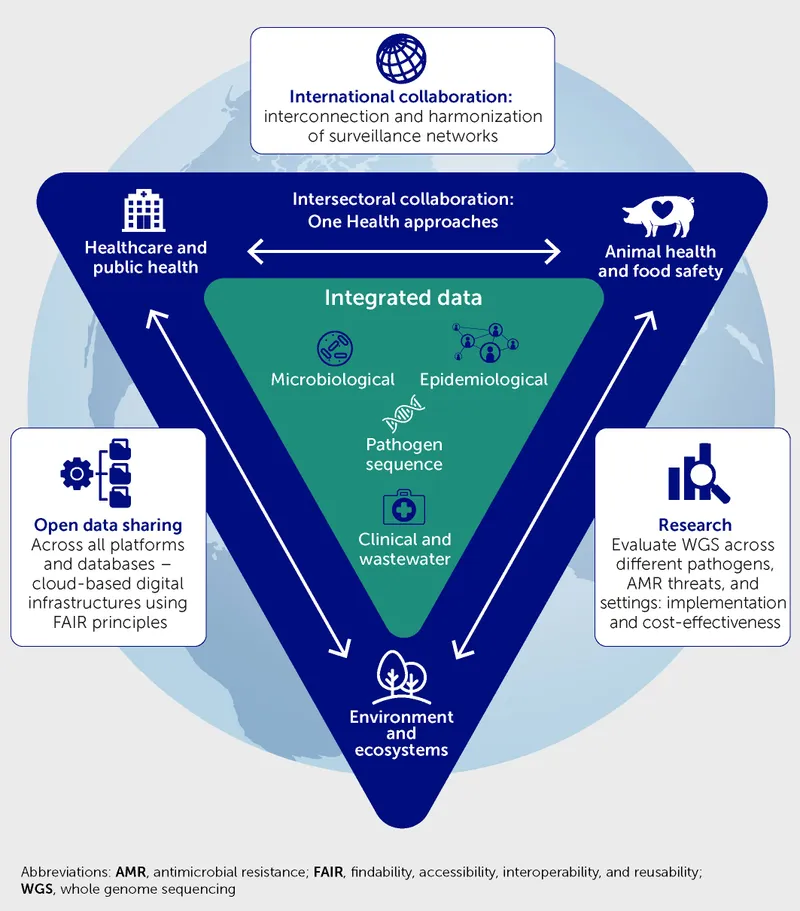
📌 Remember: COORDINATE - Cross-sector partnerships, Operational alignment, Outcome sharing, Resource pooling, Data integration, Information exchange, Network building, Accountability systems, Timing synchronization, Evaluation coordination
Multi-Sectoral Integration Models
- Convergence Platforms
- Village Health Sanitation & Nutrition Committees: 2.5 lakh active committees
- District Convergence Committees: 741 districts with monthly meetings
- Attendance rates: 70-85% across different sectors
- Joint action plans: 60% of districts have functional convergence
- Shared Resource Mechanisms
- Common Service Centers: 4.5 lakh centers providing health services
- Shared infrastructure: 30-40% cost reduction through facility sharing
- Laboratory networks: 15,000 labs with shared protocols
- Transport systems: 108 ambulances with <20 minutes response time
- Integrated Information Systems
- Health Management Information System: 99% facility reporting
- Real-time data sharing: 24/7 dashboard monitoring
- API integrations: 50+ systems connected nationally
- Data accuracy: >95% validation scores across platforms
| Coordination Level | Stakeholders Involved | Meeting Frequency | Resource Sharing | Outcome Improvement |
|---|---|---|---|---|
| National | 15+ ministries | Quarterly | ₹5,000+ crores | 25% efficiency gain |
| State | 8-12 departments | Monthly | ₹1,000-3,000 crores | 35% target achievement |
| District | 6-10 departments | Bi-weekly | ₹200-800 crores | 45% service improvement |
| Block | 4-8 departments | Weekly | ₹50-200 crores | 55% coverage increase |
| Village | 3-6 committees | Weekly | ₹5-25 lakhs | 65% participation boost |
💡 Master This: Coordination quality determines program success - initiatives with >80% coordination scores achieve 2.5 times better health outcomes than poorly coordinated programs
Connect coordination systems through quality assurance frameworks to understand excellence standards.
🔗 Coordination Mechanisms: The Integration Architecture
🏆 Quality Assurance: The Excellence Standards Engine
📌 Remember: QUALITY - Quality standards, Uniform protocols, Assessment systems, Learning mechanisms, Improvement cycles, Training programs, Yield optimization
National Quality Standards Framework
- National Quality Assurance Standards (NQAS)
- 279 quality standards across different facility types
- 8 key areas: Patient rights, input standards, support services, clinical care, infection control, quality management, outcome standards, patient safety
- Compliance rates: 40-85% across different states
- Certification levels: Bronze (>50%), Silver (>70%), Gold (>90%)
- Accreditation Systems
- National Accreditation Board: 25,000+ facilities under assessment
- International standards: JCI, NABH for tertiary care facilities
- NABH accredited: 1,200+ hospitals with >95% patient satisfaction
- Quality improvement: 30-50% enhancement in clinical outcomes
- Performance Monitoring Mechanisms
- Real-time dashboards: 24/7 quality indicator tracking
- Sentinel events monitoring: Zero tolerance for preventable adverse events
- Maternal death reviews: 100% facility-based deaths investigated
- Infection rates: <2% healthcare-associated infections target
| Quality Component | Assessment Frequency | Compliance Target | Current Achievement | Improvement Rate |
|---|---|---|---|---|
| Clinical Protocols | Monthly | 95% adherence | 78% average | 12% annually |
| Patient Safety | Continuous | Zero harm events | 2.3 per 1000 | 15% reduction |
| Infrastructure | Quarterly | 100% functional | 85% operational | 8% annually |
| Human Resources | Bi-annual | Full staffing | 70% positions filled | 5% annually |
| Equipment | Monthly | 95% uptime | 82% functional | 10% annually |
💡 Master This: Quality systems create predictable excellence - every 10% improvement in quality scores correlates with 7% reduction in adverse events and 12% increase in treatment success rates
Connect quality frameworks through digital transformation to understand modern administrative capabilities.
🏆 Quality Assurance: The Excellence Standards Engine
🚀 Digital Transformation: The Modern Administration Powerhouse
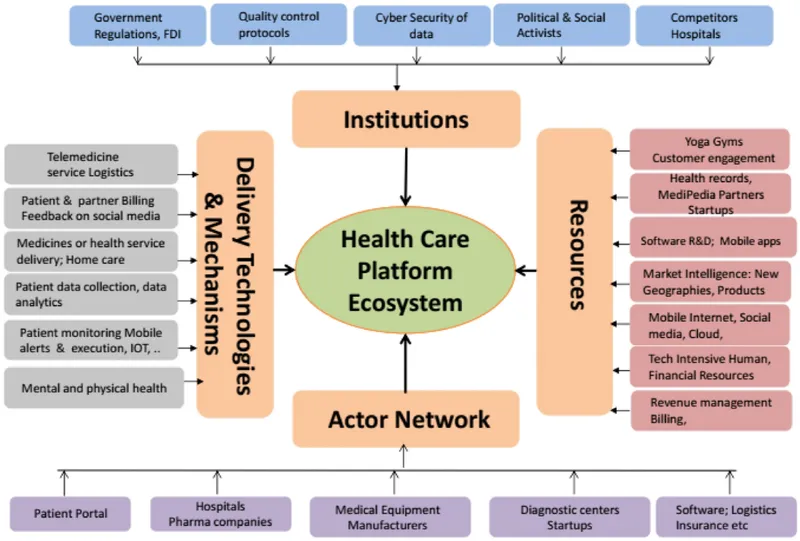
📌 Remember: DIGITAL - Data integration, Intelligent analytics, Governance automation, Interoperability standards, Telemedicine platforms, Artificial intelligence, Learning systems
Integrated Digital Platforms
- Ayushman Bharat Digital Mission
- Health IDs: 35+ crore unique health identities created
- Digital health records: 100% interoperability across platforms
- API calls: 10+ crore daily transactions processed
- Data security: 256-bit encryption with blockchain verification
- Telemedicine Infrastructure
- eSanjeevani platforms: 12+ crore teleconsultations completed
- Rural connectivity: 1.5 lakh health facilities connected
- Specialist access: 80% reduction in referral travel time
- Cost savings: ₹2,500 average per consultation saved
- AI-Powered Analytics
- Predictive modeling: 85% accuracy in disease outbreak prediction
- Resource optimization: 30% improvement in supply chain efficiency
- Drug stock management: 95% availability maintained through AI
- Staff deployment: 25% better resource allocation through algorithms
| Digital Component | Implementation Scale | User Adoption | Efficiency Gain | Cost Reduction |
|---|---|---|---|---|
| Health IDs | 35+ crore citizens | 78% active usage | 40% faster access | 25% admin costs |
| Telemedicine | 1.5 lakh facilities | 12+ crore consultations | 60% time savings | 70% travel costs |
| Digital Records | 100% facilities | 85% digitization | 50% retrieval speed | 35% storage costs |
| AI Analytics | 28 states | 90% adoption | 45% prediction accuracy | 30% operational costs |
| Mobile Apps | 50+ applications | 25+ crore downloads | 55% service speed | 40% processing costs |
💡 Master This: Digital maturity accelerates health outcomes - states with >80% digital adoption achieve health targets 2.1 times faster than digitally lagging states, with 35% better resource utilization and 45% improved service quality
Master these digital administration capabilities to transform traditional healthcare delivery into responsive, efficient, and citizen-centric public health systems that leverage technology for population health improvement.
🚀 Digital Transformation: The Modern Administration Powerhouse
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























