CEA Basics - What's the Deal?
- What: Compares costs (money) vs. health outcomes (natural units: LYG, cases averted) of interventions.
- Goal: Best value - max health per cost, or target health at min cost.
- Outcomes: Natural units (LYG, lives saved), not money.
- Core Metric: Incremental Cost-Effectiveness Ratio (ICER).
- $ICER = \frac{\Delta C}{\Delta E}$
- Key Distinctions:
- vs. CMA: Outcomes differ (CMA: equal).
- vs. CBA: Health units, not money (CBA: money).
- CUA: Subtype using QALYs/DALYs.
⭐ CEA focuses on allocative efficiency: choosing interventions that maximize health outcomes from a limited budget.
CEA Metrics - Number Crunching
- Costs in CEA:
- Direct Costs: Medical (drugs, consultations, fees), Non-medical (patient travel, special food).
- Indirect Costs: Productivity losses (absenteeism from work, premature mortality).
- Intangible Costs: Pain, suffering, anxiety (difficult to value monetarily).
- Outcome Measures:
- QALY (Quality-Adjusted Life Year): $1 \text{ QALY} = 1 \text{ year of life in perfect health}$. Measures health gain.
- DALY (Disability-Adjusted Life Year): $DALY = YLL + YLD$. Measures overall disease burden.
- YLL: Years of Life Lost (due to premature mortality).
- YLD: Years Lived with Disability (adjusted for severity & duration).
- ICER (Incremental Cost-Effectiveness Ratio):
- Formula: $ICER = \frac{(\text{Cost}\text{new} - \text{Cost}\text{std})}{(\text{Effect}\text{new} - \text{Effect}\text{std})}$ (or $\frac{\Delta C}{\Delta E}$)
- Compares extra cost for extra health gain of a new intervention vs. standard/comparator.
- Units: e.g., Cost per QALY gained, Cost per DALY averted.
⭐ ICER helps determine if an intervention's additional cost is justified by its additional health benefit, guiding resource allocation decisions.
CEA Steps - The How-To Guide
- 1. Define Problem & Perspective: State health question, population, viewpoint (e.g., societal, payer).
- 2. Identify Alternatives: List interventions/programs for comparison (e.g., new vs. standard).
- 3. Identify & Measure Costs: Quantify resources: direct medical/non-medical, indirect costs (e.g., productivity).
- 4. Identify & Measure Outcomes: Assess effects: natural units (e.g., LYG, cases averted) or QALYs.
- 5. Calculate ICER: $ICER = \frac{\Delta \text{Cost}}{\Delta \text{Effect}}$.
- 6. Conduct Sensitivity Analysis: Evaluate impact of uncertainty in estimates on ICER.
- 7. Interpret & Recommend: Compare ICER to cost-effectiveness threshold for decisions.
⭐ The perspective of a CEA (e.g., patient, provider, societal) significantly influences which costs and benefits are included, thereby affecting the results.
Interpreting & Applying CEA - Decision Time!
- Incremental Cost-Effectiveness Ratio (ICER): $ICER = \frac{\Delta C}{\Delta E} = \frac{C_1 - C_0}{E_1 - E_0}$. Compare to WTP.
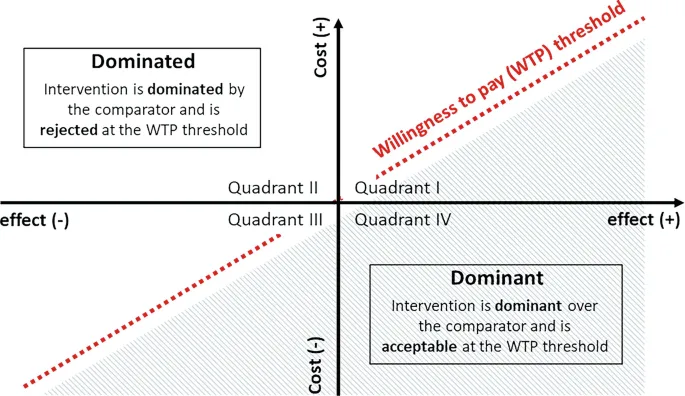
- Cost-Effectiveness (CE) Plane: Visualizes interventions:
- NE Quadrant (More effect, Less cost): Dominant → Accept.
- SW Quadrant (Less effect, More cost): Dominated → Reject.
- SE/NW Quadrants: Trade-offs, decision via ICER vs. WTP.
- Willingness-to-Pay (WTP) Threshold: Max society pays for health gain (e.g., per QALY/DALY averted).
- ICER < WTP: Cost-effective.
- ICER > WTP: Not cost-effective.
⭐ WHO: 1x GDP per capita = very cost-effective; 1-3x GDP per capita = cost-effective.
- Decision Rule: Prioritize interventions where ICER < WTP. Consider equity & budget impact.
- Sensitivity Analysis: Tests robustness of ICER to uncertainties.
High‑Yield Points - ⚡ Biggest Takeaways
- CEA compares interventions by costs (monetary) and health outcomes (natural units like LYG, QALYs).
- Key metric: ICER (Incremental Cost-Effectiveness Ratio) = ΔCost / ΔEffect.
- Dominant strategy: Cheaper and more effective; always preferred.
- Dominated strategy: More expensive and less effective; always rejected.
- Cost-Effectiveness Plane visually plots interventions against a comparator.
- Willingness-to-Pay (WTP) threshold helps decide if an ICER is acceptable.
- CEA aids in efficient resource allocation and health policy decisions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

