Health Economics

On this page
💰 The Economic Engine: Healthcare's Financial Architecture
Healthcare consumes trillions globally, yet most clinicians never learn how these resources flow, who decides their allocation, or how to measure true value beyond price tags. You'll master the economic frameworks that shape every clinical decision-from insurance mechanics and financing models to cost-benefit analysis and burden quantification-transforming you into a physician who understands not just what care to deliver, but how systems determine which patients receive it and why. This knowledge turns you from a passive participant into an architect of sustainable, equitable healthcare delivery.
📌 Remember: HEAL - Health needs are unlimited, Economic resources are scarce, Allocation requires choices, Lives depend on efficiency
Healthcare economics operates on three fundamental pillars that distinguish it from traditional market economics:
-
Scarcity Management
- Global health spending: $8.3 trillion annually (10.9% of global GDP)
- India's health expenditure: ₹6.15 lakh crores (3.6% of GDP in 2021-22)
- Per capita health spending: ₹4,381 (significantly below WHO recommendation of $86)
- Public spending: ₹1,753 per capita (40% of total)
- Private spending: ₹2,628 per capita (60% of total)
-
Market Peculiarities
- Information asymmetry: Patients lack 85% of medical knowledge physicians possess
- Demand uncertainty: 70% of healthcare needs are unpredictable
- Supply constraints: 1:1,456 doctor-patient ratio (WHO standard: 1:1,000)
-
Outcome Optimization
- Quality-Adjusted Life Years (QALYs): Standard metric for health outcomes
- Cost-effectiveness threshold: ₹1-3 lakhs per QALY in Indian context
- Disability-Adjusted Life Years (DALYs): 40.5 million lost annually in India
| Economic Principle | Traditional Markets | Healthcare Markets | Impact Factor | Indian Context |
|---|---|---|---|---|
| Price Elasticity | High (-1.2 to -2.0) | Low (-0.2 to -0.6) | Demand insensitive | 78% pay out-of-pocket |
| Information | Symmetric | Asymmetric (85% gap) | Trust-dependent | 12% health literacy |
| Entry Barriers | Moderate | Extreme (8-12 years) | Supply constrained | 1:1,456 ratio |
| Externalities | Limited | Extensive (herd immunity) | Social benefits | ₹2.1 lakh crores indirect costs |
| Uncertainty | Predictable | Unpredictable (70%) | Insurance essential | 38% coverage |
💡 Master This: Market failure in healthcare occurs when free markets cannot efficiently allocate resources - requiring government intervention through regulation, subsidies, and public provision to ensure equitable access and optimal outcomes
Understanding healthcare's economic foundation connects directly to resource allocation principles, where these market peculiarities create unique challenges in distributing finite medical resources across infinite population needs.
💰 The Economic Engine: Healthcare's Financial Architecture
⚖️ Resource Allocation Mastery: The Distribution Dilemma
📌 Remember: PRIME - Priority setting requires criteria, Resources are always limited, Impact measurement guides decisions, Maximize population benefit, Equity ensures fairness
Healthcare resource allocation operates through four fundamental approaches that determine how societies distribute medical care:
-
Allocation Principles
- Utilitarian approach: Greatest good for greatest number (maximize QALYs)
- Egalitarian approach: Equal access regardless of ability to pay
- Libertarian approach: Market-based distribution (ability to pay)
- Rawlsian approach: Priority to worst-off populations (social justice)
- India follows mixed approach: 62% private + 38% public provision
- Constitutional mandate: Right to health under Article 21
-
Priority Setting Criteria
- Disease burden: 40.5 million DALYs lost annually in India
- Cost-effectiveness: Interventions below ₹1-3 lakhs per QALY
- Budget impact: Total financial implications for health system
- Equity considerations: Geographic and socioeconomic disparities
- Rural-urban gap: 1:3 specialist availability ratio
- Interstate variation: 2.5x difference in health outcomes
-
Resource Categories
- Human resources: 1.34 million doctors, 2.96 million nurses
- Infrastructure: 1.85 lakh health facilities (70% public)
- Technology: ₹45,000 crores medical device market
- Pharmaceuticals: ₹1.72 lakh crores domestic market
| Allocation Method | Efficiency Focus | Equity Focus | Implementation Complexity | Indian Application |
|---|---|---|---|---|
| Market-based | High (90%+) | Low (30%) | Simple | Private sector (62%) |
| Need-based | Moderate (60%) | High (85%) | Complex | NRHM rural focus |
| Merit-based | High (80%) | Moderate (50%) | Moderate | AIIMS selection |
| Rights-based | Low (40%) | Very High (95%) | Very Complex | RSBY/AB-PMJAY |
| Mixed approach | Moderate (65%) | Moderate (65%) | High | Current Indian system |
💡 Master This: Effective resource allocation requires explicit priority-setting frameworks that balance clinical effectiveness, cost-efficiency, and social equity - transparent criteria prevent arbitrary decisions and ensure optimal population health outcomes
Resource allocation principles directly inform cost-benefit analysis methodologies, where systematic evaluation frameworks determine which healthcare interventions provide maximum value for invested resources.
⚖️ Resource Allocation Mastery: The Distribution Dilemma
🔍 Cost-Benefit Analysis Architecture: The Value Calculation Engine
📌 Remember: BENEFIT - Benefits must be monetized, Externalities included, Net present value calculated, Equity weights applied, Future costs discounted, Intangible benefits valued, Time horizon specified
Cost-benefit analysis operates through six systematic components that transform complex health outcomes into comparable monetary units:
-
Cost Identification and Measurement
- Direct medical costs: Hospital care (₹1.8 lakh crores), pharmaceuticals (₹1.72 lakh crores)
- Direct non-medical costs: Transportation (₹15,000 crores), accommodation
- Indirect costs: Productivity losses (₹2.1 lakh crores annually)
- Intangible costs: Pain, suffering, quality of life impacts
- Time horizon: Typically 10-30 years for chronic disease interventions
- Discount rate: 3-5% annually for future costs and benefits
-
Benefit Quantification Methods
- Human capital approach: Productivity gains from prevented mortality/morbidity
- Willingness-to-pay: Survey-based valuation of health improvements
- Quality-Adjusted Life Years: ₹1-3 lakhs per QALY in Indian context
- Value of Statistical Life: ₹15-45 lakhs (varies by methodology)
- Revealed preference: Market behavior analysis
- Stated preference: Contingent valuation surveys
-
Analytical Framework Components
- Incremental analysis: Compare intervention vs. status quo
- Sensitivity analysis: Test assumption variations (±20% parameter changes)
- Uncertainty analysis: Monte Carlo simulations with 10,000+ iterations
- Equity weighting: Adjust for distributional impacts across populations
| CBA Component | Measurement Method | Typical Range (₹) | Data Sources | Reliability Level |
|---|---|---|---|---|
| Direct Medical | Accounting records | ₹5,000-5 lakhs | Hospital bills, insurance | High (95%) |
| Productivity Loss | Human capital | ₹50,000-8 lakhs | Wage surveys, employment | Moderate (70%) |
| Quality of Life | QALY monetization | ₹1-3 lakhs/QALY | Utility studies | Moderate (65%) |
| Mortality Prevention | VSL approach | ₹15-45 lakhs/life | Economic studies | Low (50%) |
| Caregiver Burden | Opportunity cost | ₹25,000-2 lakhs | Time-use surveys | Low (45%) |
💡 Master This: CBA enables comparison of diverse healthcare interventions on a common monetary scale - converting health outcomes to rupee values allows direct comparison between cancer screening programs and road safety initiatives for optimal resource allocation
Cost-benefit analysis frameworks directly support health insurance system design, where actuarial calculations determine premium structures and coverage decisions based on expected costs and benefits across covered populations.
🔍 Cost-Benefit Analysis Architecture: The Value Calculation Engine
🛡️ Health Insurance Mechanics: The Risk Distribution Network
📌 Remember: INSURE - Insurance pools risks, Need drives utilization, Solidarity spreads costs, Underwriting assesses risk, Reserves ensure solvency, Equity improves access
Health insurance operates through five fundamental mechanisms that transform individual health risks into manageable collective financial instruments:
-
Risk Pooling Principles
- Law of large numbers: Risk predictability increases with pool size
- Cross-subsidization: Healthy subsidize sick, young subsidize old
- Temporal smoothing: Current premiums cover future uncertain costs
- Geographic pooling: Urban-rural risk distribution
- Optimal pool size: 100,000+ lives for stable risk prediction
- Risk variation: 10:1 ratio between high and low-risk individuals
-
Premium Calculation Components
- Expected claims: ₹8,500 average per member per year
- Administrative costs: 8-15% of premium (₹680-1,275 per member)
- Profit margin: 3-8% for private insurers
- Reserves: 15-25% of annual premiums for claim fluctuations
- Medical inflation: 12-15% annually in India
- Utilization growth: 8-12% annual increase
-
Coverage Design Elements
- Benefit package: Services covered under insurance scheme
- Cost-sharing: Deductibles (₹5,000-25,000), copayments (10-20%)
- Provider networks: Empaneled hospitals and clinics
- Utilization management: Prior authorization, case management
| Insurance Model | Risk Pool Size | Premium Structure | Coverage Scope | Indian Examples |
|---|---|---|---|---|
| Social Insurance | 500M+ lives | Income-based (2-6%) | Comprehensive | ESIC (3.25% wage) |
| Private Voluntary | 50K-2M lives | Risk-based (₹5K-50K) | Variable packages | Star Health, HDFC |
| Government Sponsored | 100M+ lives | Tax-funded | Targeted services | AB-PMJAY (₹5 lakh cover) |
| Community-based | 1K-50K lives | Flat contribution | Basic services | SEWA cooperatives |
| Employer-based | 10K-500K lives | Employer-funded | Employee benefits | Corporate group policies |
💡 Master This: Effective health insurance requires balanced risk pools with adequate healthy members to subsidize sick members - successful schemes maintain 80:20 healthy-to-sick ratios through mandatory enrollment or risk adjustment mechanisms
Health insurance mechanisms directly enable diverse financing strategies, where multiple funding sources and payment methods create comprehensive healthcare financing systems that support universal health coverage goals.
🛡️ Health Insurance Mechanics: The Risk Distribution Network
💳 Healthcare Financing Blueprints: The Revenue Architecture
📌 Remember: FINANCE - Funding sources diversified, Intermediate pooling mechanisms, Needs-based allocation, Accountability ensures efficiency, Network provider payments, Cost containment strategies, Equitable access maintained
Healthcare financing operates through six integrated components that transform diverse revenue sources into coordinated healthcare delivery systems:
-
Revenue Generation Mechanisms
- Tax-based financing: ₹2.73 lakh crores (44% of total health spending)
- Social insurance contributions: ₹45,000 crores (7% of total)
- Private insurance premiums: ₹75,000 crores (12% of total)
- Out-of-pocket payments: ₹2.28 lakh crores (37% of total)
- Tax revenue sources: Income tax (35%), GST (28%), corporate tax (22%)
- Contribution rates: ESIC (3.25% of wages), state schemes (1-2%)
-
Pooling Arrangements
- National pooling: Single risk pool for entire population
- Regional pooling: State-level or district-level risk sharing
- Occupational pooling: Employment-based insurance schemes
- Voluntary pooling: Community-based health insurance
- Pool fragmentation: India has 100+ separate health financing pools
- Cross-subsidization: Limited due to fragmented pooling arrangements
-
Provider Payment Systems
- Fee-for-service: ₹1.8 lakh crores (70% of private sector payments)
- Capitation: ₹15,000 per family per year under PMJAY
- Diagnosis-related groups: ₹5,000-8 lakhs per case package rates
- Global budgets: Annual allocation to public hospitals
- Payment delays: Average 90-120 days for government schemes
- Administrative costs: 8-15% of total scheme expenditure
| Financing Model | Revenue Stability | Equity Impact | Efficiency Incentives | Administrative Cost | Indian Context |
|---|---|---|---|---|---|
| Tax-based | High (95%) | High (85%) | Moderate (60%) | Low (3-5%) | Central/State budgets |
| Social Insurance | High (90%) | High (80%) | Moderate (65%) | Moderate (8-12%) | ESIC system |
| Private Insurance | Moderate (70%) | Low (30%) | High (80%) | High (15-20%) | Commercial market |
| Out-of-pocket | Low (40%) | Very Low (15%) | High (85%) | Very Low (1%) | Dominant in India |
| Mixed System | Moderate (75%) | Moderate (55%) | Moderate (65%) | Moderate (10%) | Current Indian model |
💡 Master This: Effective healthcare financing balances revenue adequacy, risk protection, and efficiency incentives - optimal systems combine progressive revenue generation with strategic purchasing to maximize population health outcomes per rupee invested
Healthcare financing mechanisms directly determine the economic burden of disease patterns, where different funding arrangements create varying financial impacts on individuals, families, and society when illness occurs.
💳 Healthcare Financing Blueprints: The Revenue Architecture
📊 Economic Burden Quantification: The True Cost Calculator
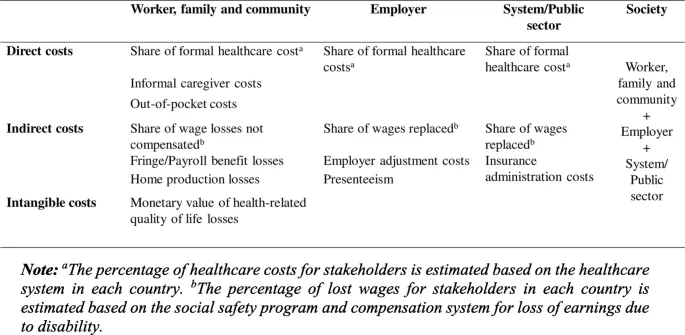

📌 Remember: BURDEN - Both direct and indirect costs, Utility losses quantified, Resource consumption measured, Disability impacts valued, Economic productivity effects, National accounting integration
Economic burden analysis operates through four comprehensive cost categories that capture the full societal impact of disease and illness:
-
Direct Medical Costs
- Hospital inpatient care: ₹1.8 lakh crores (29% of total health spending)
- Outpatient services: ₹1.2 lakh crores (19% of total spending)
- Pharmaceuticals: ₹1.72 lakh crores (28% of total spending)
- Diagnostic services: ₹45,000 crores (7% of total spending)
- Catastrophic expenditure: 18% of households spend >10% income on health
- Impoverishment: 7% of households pushed below poverty line annually
-
Direct Non-Medical Costs
- Transportation: ₹15,000 crores annually for healthcare access
- Accommodation: ₹8,000 crores for patient/family lodging
- Caregiver expenses: ₹12,000 crores for informal care support
- Equipment/modifications: ₹5,000 crores for disability aids
- Rural transportation: Average ₹2,500 per episode for specialist care
- Urban parking/transport: ₹500-1,500 per hospital visit
-
Indirect Costs (Productivity Losses)
- Premature mortality: ₹1.2 lakh crores in lost lifetime earnings
- Morbidity-related absence: ₹85,000 crores in lost workdays
- Reduced productivity: ₹45,000 crores from presenteeism
- Caregiver time: ₹35,000 crores in opportunity costs
- Average workdays lost: 12 days per illness episode
- Caregiver burden: 2.5 family members affected per patient
-
Intangible Costs
- Pain and suffering: Measured through Quality-Adjusted Life Years
- Reduced quality of life: ₹1-3 lakhs per QALY lost
- Psychological distress: Depression in 35% of chronic disease patients
- Social isolation: Reduced social participation and relationships
| Disease Category | Direct Medical (₹ Crores) | Indirect Costs (₹ Crores) | Total Burden (₹ Crores) | % of GDP | DALYs Lost (Millions) |
|---|---|---|---|---|---|
| Cardiovascular | 85,000 | 1,25,000 | 2,10,000 | 0.9% | 8.5 |
| Cancer | 65,000 | 95,000 | 1,60,000 | 0.7% | 6.2 |
| Diabetes | 45,000 | 75,000 | 1,20,000 | 0.5% | 4.8 |
| Respiratory | 35,000 | 55,000 | 90,000 | 0.4% | 5.1 |
| Mental Health | 25,000 | 85,000 | 1,10,000 | 0.5% | 7.3 |
| Infectious Disease | 55,000 | 45,000 | 1,00,000 | 0.4% | 8.6 |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | |||||
| flowchart TD |
INC["📉 Disease Incidence
• New case frequency• Population impact"]
DMC["🏥 Direct Medical
• Hospital service• Pharma treatment"]
DNC["🚗 Direct Non-Med
• Travel expenses• Home care costs"]
IDC["💼 Indirect Costs
• Work absences• Reduced output"]
ITC["👤 Intangible Costs
• Pain and suffering• Family distress"]
UTI["🩺 Utilization
• Resource usage• Clinic visits"]
EXP["💸 Family Expense
• Household impact• Out of pocket"]
LOS["📉 Productivity
• Labor loss• Income reduction"]
QOL["🧬 QoL Impact
• Wellness level• Health status"]
TOT["💰 Total Burden
• Economic sum• Societal cost"]
POL{"📋 Policy Implication
• Strategic planning• Resource choice"}
PRI["⚠️ Priority Stat
• Urgent action• High investment"]
TAR["🎯 Targeted Prog
• Specific focus• Shared funding"]
MON["👁️ Monitoring
• Routine watch• Annual review"]
INC --> DMC INC --> DNC INC --> IDC INC --> ITC
DMC --> UTI DNC --> EXP IDC --> LOS ITC --> QOL
UTI --> TOT EXP --> TOT LOS --> TOT QOL --> TOT
TOT --> POL
POL -->|High| PRI POL -->|Moderate| TAR POL -->|Low| MON
style INC fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style DMC fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style DNC fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style IDC fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style ITC fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style UTI fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style EXP fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style LOS fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style QOL fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style TOT fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style POL fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style PRI fill:#FDF4F3, stroke:#FCE6E4, stroke-width:1.5px, rx:12, ry:12, color:#B91C1C style TAR fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style MON fill:#EEFAFF, stroke:#DAF3FF, stroke-width:1.5px, rx:12, ry:12, color:#0369A1
> ⭐ **Clinical Pearl**: **Indirect costs often exceed direct medical costs for chronic diseases** - cardiovascular disease generates **₹1.25 lakh crores** in productivity losses compared to **₹85,000 crores** in direct medical expenses, highlighting prevention's economic value
> 💡 **Master This**: **Economic burden analysis reveals the true societal cost of disease beyond healthcare spending** - comprehensive measurement including productivity losses and quality-of-life impacts guides evidence-based priority setting and resource allocation decisions
Economic burden quantification directly informs cost-effectiveness analysis frameworks, where comprehensive cost data enables systematic comparison of intervention alternatives to identify optimal strategies for reducing disease burden and maximizing health system efficiency.
📊 Economic Burden Quantification: The True Cost Calculator
🎯 Clinical Mastery Arsenal: Economic Decision-Making Tools
📌 Remember: MASTER - Measure all costs comprehensively, Assess outcomes systematically, Synthesis through economic evaluation, Target efficient interventions, Equity considerations integrated, Resource optimization achieved
Essential economic evaluation toolkit for healthcare decision-making:
-
Cost-Effectiveness Thresholds
- Highly cost-effective: <₹50,000 per QALY gained
- Cost-effective: ₹50,000-1.5 lakhs per QALY
- Moderately cost-effective: ₹1.5-3 lakhs per QALY
- Not cost-effective: >₹3 lakhs per QALY
- WHO threshold: 1-3x GDP per capita (₹1.4-4.2 lakhs)
- Indian context: ₹1-3 lakhs most appropriate range
-
Budget Impact Analysis Framework
- 5-year financial projections for new interventions
- Population coverage estimates and uptake rates
- Displacement effects on existing services
- Infrastructure requirements and capacity constraints
-
Equity Integration Methods
- Distributional cost-effectiveness analysis across income quintiles
- Geographic equity assessment (rural-urban disparities)
- Social value weighting for disadvantaged populations
- Financial risk protection impact measurement
| Economic Tool | Application | Time Horizon | Data Requirements | Decision Threshold | Indian Examples |
|---|---|---|---|---|---|
| Cost-Effectiveness | Intervention comparison | 10-30 years | Costs, QALYs | <₹3 lakhs/QALY | HPV vaccination |
| Budget Impact | Affordability assessment | 3-5 years | Costs, uptake rates | <5% budget | PMJAY expansion |
| Cost-Benefit | Social value assessment | 20-50 years | Monetized benefits | BCR >1.0 | Immunization programs |
| Cost-Utility | Quality of life focus | Lifetime | Utilities, costs | <₹2 lakhs/QALY | Dialysis vs transplant |
| Multi-criteria | Complex decisions | Variable | Multiple outcomes | Weighted scores | Essential medicine selection |
💡 Master This: Successful healthcare economic evaluation requires integration of efficiency, equity, and feasibility considerations - optimal decisions balance cost-effectiveness evidence with budget constraints, implementation capacity, and social value judgments to maximize population health outcomes
Understanding healthcare economics transforms clinical practice by revealing the resource implications of medical decisions, enabling healthcare professionals to optimize both individual patient outcomes and population health through evidence-based resource allocation and systematic economic evaluation frameworks.
🎯 Clinical Mastery Arsenal: Economic Decision-Making Tools
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























