Definitions & Objectives - Epidemic Essentials
- Epidemic: Disease occurrence clearly exceeding normal expectancy.
- Outbreak: Localized epidemic (e.g., village, institution).
- Endemic: Constant presence of disease in a specific area/population.
- Pandemic: Epidemic over a wide geographical area, often global.
- Sporadic: Irregular, haphazard, infrequent cases.
- Objectives of Investigation:
- Define problem magnitude (cases, deaths).
- Identify agent, source, mode of transmission.
- Implement control measures.
- Prevent future occurrences.
⭐ An epidemic is not defined by a fixed number of cases, but by exceeding the expected level.
Investigation Steps - Detective's Toolkit
A systematic, multi-step approach to identify an epidemic's origin, transmission mode, and implement effective control.
Key Investigative Steps:
- Verification:
- Confirm diagnosis (clinical/lab).
- Establish epidemic existence (cases > expected frequency).
- Case Definition & Finding:
- Develop precise case criteria (suspected, probable, confirmed).
- Conduct active case search.
- Descriptive Epidemiology: Characterize by:
- Time: Epidemic curve (pattern: common source, propagated, mixed).
- Place: Spot map for geographic spread; calculate place-specific attack rates.
- Person: Calculate person-specific attack rates (age, sex, occupation, exposure history).
- Hypothesis Formulation:
- Propose likely agent, source, transmission mode, and risk factors.
- Hypothesis Testing:
- Use analytical studies (case-control, cohort).
- Calculate Odds Ratio (OR) / Relative Risk (RR).
- Control & Prevention:
- Implement measures targeting source, interrupting transmission, protecting susceptibles.
- Communication:
- Disseminate findings and recommendations to authorities, health professionals, and public.
⭐ Attack Rate (AR): vital in outbreaks (e.g., foodborne). Proportion of exposed who get ill.
Attack Rate (AR) = $\frac{\text{Number of new cases among exposed}}{\text{Total number exposed}} \times 100$
Measures & Curves - Tracking Patterns
- Attack Rate (AR): $AR = \frac{\text{No. of new cases in specified period}}{\text{Total population at risk during same period}} \times 100$. Measures risk in exposed population.
- Secondary Attack Rate (SAR): $SAR = \frac{\text{New cases among contacts of primary cases (within 1 incubation period)}}{\text{Total susceptible contacts}} \times 100$. Measures person-to-person spread.
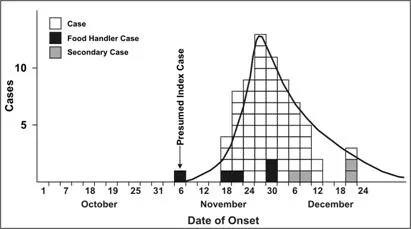
- Epidemic Curve: Plot of cases by time of onset. Shows outbreak's pattern, magnitude, duration, outliers, and likely incubation period.
- Common Source Outbreaks: Exposure to a common noxious influence.
- Point Source: Rapid rise, sharp peak, rapid fall. Cases within 1 incubation period. (e.g., food poisoning)
- Continuous Source: Prolonged exposure. Gradual rise, plateau, then fall. (e.g., contaminated well)
- Intermittent Source: Irregular peaks reflecting periodic exposure. (e.g., leaky sewer)
- Propagated (Progressive) Outbreaks: Person-to-person spread.
- Series of progressively taller peaks, each ~1 incubation period apart. (e.g., measles)
- Mixed Outbreaks: Features of both common source and propagated.
- Common Source Outbreaks: Exposure to a common noxious influence.
⭐ The shape of an epidemic curve helps identify the probable source of infection and mode of transmission.
Control & Reporting - Ending the Outbreak
- Control Measures: Aimed at source/reservoir, routes of transmission, and susceptible hosts.
- Source: Isolation, treatment, quarantine (📌 QRT: Quarantine - Restriction of healthy contacts for specific Time).
- Transmission: Environmental disinfection, vector control, food/water safety.
- Host: Immunization, chemoprophylaxis, PPE, health education.
- Monitoring & Surveillance:
- Track new cases, assess control measure effectiveness.
⭐ An outbreak is typically declared over when 2 maximum incubation periods have passed since the onset of the last identified case.
- Reporting:
- Preliminary and comprehensive final reports.
- Final report: Background, methods, findings, control measures, recommendations.
- Disseminate to authorities (e.g., IDSP), stakeholders; consider publication.
High‑Yield Points - ⚡ Biggest Takeaways
- Verify diagnosis is the critical first step in any outbreak investigation.
- Confirm epidemic existence by comparing current incidence with expected baseline levels.
- A precise case definition ensures consistent case identification.
- Analyze time, place, and person data to describe the epidemic.
- Calculate attack rates to measure risk among exposed populations.
- The epidemic curve visualizes onset patterns, indicating common-source or propagated spread.
- Implement control measures immediately, often before identifying the exact pathogen.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

