Climate Change Science Basics - Earth's Warm Hug
- Greenhouse Effect: Natural process warming Earth's surface. Atmosphere traps solar energy.
- Sunlight (shortwave radiation) reaches Earth.
- Earth absorbs and re-radiates heat (longwave infrared radiation).
- Greenhouse Gases (GHGs): Absorb and re-emit this infrared radiation, trapping heat.
- Key GHGs: Carbon Dioxide ($CO_2$), Methane ($CH_4$), Nitrous Oxide ($N_2O$), Water Vapour ($H_2O$).
- 📌 Mnemonic: "Can Monkeys Nibble Watermelons?" ($CO_2$, $CH_4$, $N_2O$, $H_2O$)
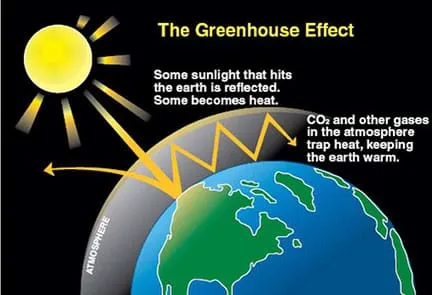
⭐ $CO_2$ is the primary anthropogenic GHG, contributing most to current warming. Its atmospheric lifetime is centuries.
Climate Change Science Basics - The Heat Trappers
- Greenhouse gases (GHGs) trap atmospheric heat, warming Earth (Greenhouse Effect).
- Enhanced effect from ↑ human activities (e.g., burning fossil fuels) causes global warming.
- Key GHGs and their characteristics:
| Greenhouse Gas | Formula | Major Sources | GWP (100-yr) | Approx. Atmospheric Lifetime |
|---|---|---|---|---|
| Carbon Dioxide | $CO_2$ | Fossil fuels, deforestation, cement | 1 | Variable, long (50-200+ yrs) |
| Methane | $CH_4$ | Agriculture (livestock, rice), waste, fossil fuels | 25-28 | ~12 years |
| Nitrous Oxide | $N_2O$ | Agriculture (fertilizers), fossil fuels, biomass burning | 265-298 | ~114 years |
| Fluorinated Gases | e.g., HFCs, $SF_6$ | Industrial processes, refrigerants | Thousands | Variable (yrs to millennia) |
Climate Change Science Basics - Planet's Vital Signs
- Global Temperature Rise:
- Atmosphere & oceans warming significantly.
- Global average temperature ↑ by ~1.1-1.2°C above pre-industrial levels (1850-1900).
- Due to ↑ anthropogenic greenhouse gases (GHGs).
- Sea Level Rise:
- Global average sea level ↑ by ~20 cm (0.2m) since 1900.
- Causes: Thermal expansion of water, melting glaciers & ice sheets.
- Ocean Acidification:
- Oceans absorb ~25-30% of anthropogenic $CO_2$ emissions.
- Leads to ↓ pH (increased acidity), harming marine ecosystems.
- Extreme Weather Events:
- ↑ Frequency & intensity of heatwaves, droughts, heavy rainfall, and tropical cyclones.
- Melting Ice & Snow (Cryosphere Changes):
- Widespread glacier retreat, shrinking ice sheets (Greenland, Antarctica), ↓ Arctic sea ice extent.
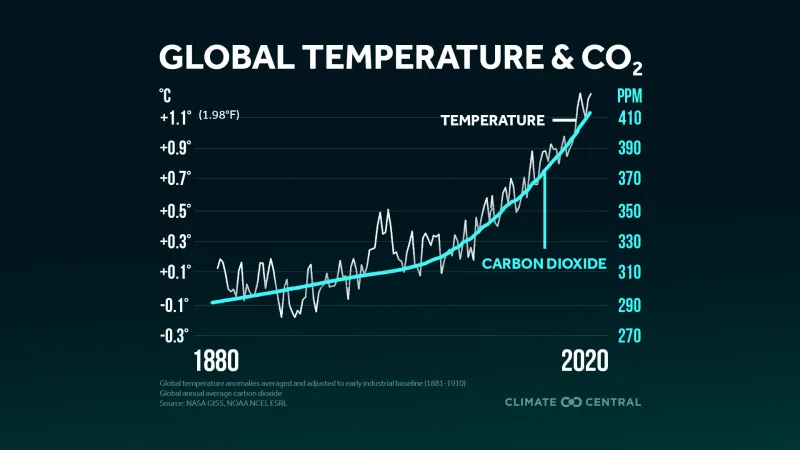
⭐ Atmospheric $CO_2$ levels now exceed 410 ppm, the highest in at least 800,000 years an crucial indicator of climate change.
Climate Change Science Basics - Who's Pushing Buttons?
- Primary Drivers of Climate Change:
- Anthropogenic (Human-Caused): The dominant influence.
- Fossil Fuel Combustion: Releases Greenhouse Gases (GHGs): $CO_2$, $CH_4$, $N_2O$.
- Deforestation & Land Use Change: Reduces $CO_2$ sinks.
- Industrial Processes: GHG & aerosol emissions.
- Agriculture: Livestock ($CH_4$), rice ($CH_4$), fertilizers ($N_2O$).
- Natural Factors: Minor role in current warming.
- Solar Activity Variations.
- Volcanic Eruptions: Aerosols cause short-term cooling.
- Earth's Orbital Cycles (Milankovitch): Long-term climate influence.
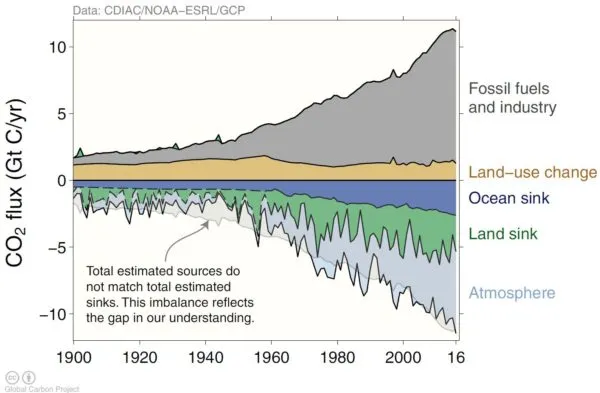
- Anthropogenic (Human-Caused): The dominant influence.
⭐ IPCC: Unequivocal that human influence has warmed atmosphere, ocean, land.
- Greenhouse gases (GHGs) like CO2, CH4, N2O trap heat, causing global warming.
- Global Warming Potential (GWP) measures a GHG's heat-trapping ability relative to CO2.
- The IPCC is the primary international body for climate change assessment.
- The Paris Agreement aims to limit warming well below 2°C, pursuing efforts for 1.5°C.
- Key anthropogenic sources: fossil fuel burning, deforestation, and agriculture.
- Major consequences include ↑ sea levels, extreme weather events, and vector-borne disease spread.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

