Purine Degradation - Uric Acid Unravelled
- Purines (AMP, GMP) ultimately degrade to Uric Acid.
- Key Intermediates: Inosine, Guanosine, Hypoxanthine, Xanthine.
- Xanthine Oxidase (XO): Key enzyme. Catalyzes two steps:
- Hypoxanthine $\rightarrow$ Xanthine
- Xanthine $\rightarrow$ Uric Acid. Produces $H_2O_2$.
- Clinical Correlation: Gout (Hyperuricemia).
- $\uparrow$ Uric acid levels $\rightarrow$ monosodium urate crystal deposition in joints & tissues.
- Significant Enzyme Deficiencies:
- ADA (Adenosine Deaminase) Deficiency: Accumulation of adenosine & deoxyadenosine $\rightarrow$ lymphotoxicity (especially T & B cells) $\rightarrow$ Severe Combined Immunodeficiency (SCID). 📌 ADA causes SCID.
- PNP (Purine Nucleoside Phosphorylase) Deficiency: Affects T-cells primarily $\rightarrow$ recurrent infections, neurological issues.
⭐ Allopurinol, a suicide inhibitor, and Febuxostat, a non-purine inhibitor, target Xanthine Oxidase in gout treatment.

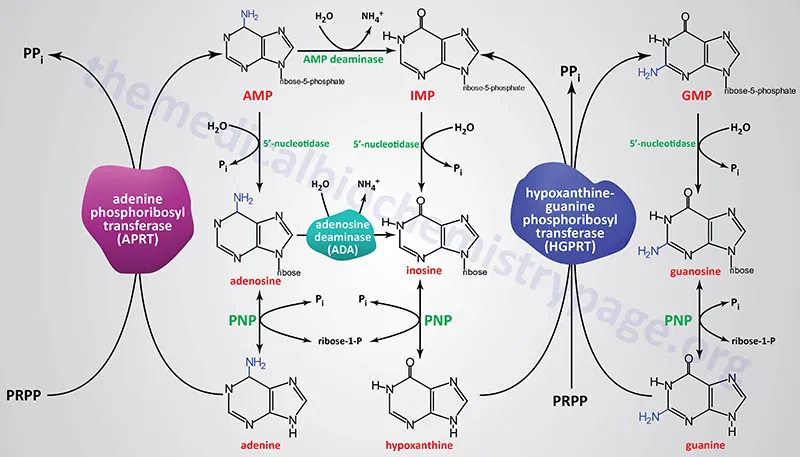
Purine Salvage - Rescue & Recycle
- Reclaims purine bases (adenine, guanine, hypoxanthine) from degradation, using PRPP.
- Conserves energy vs. de novo synthesis. Vital for tissues with low de novo capacity (e.g., brain).
- Key Enzymes & Reactions:
- APRT (Adenine Phosphoribosyltransferase):
- Adenine + PRPP $\rightarrow$ AMP + PPi
- Deficiency: APRT nephropathy (2,8-dihydroxyadenine stones).
- HGPRT (Hypoxanthine-Guanine Phosphoribosyltransferase):
- Hypoxanthine + PRPP $\rightarrow$ IMP + PPi
- Guanine + PRPP $\rightarrow$ GMP + PPi
- Partial deficiency: Kelley-Seegmiller syndrome (gout, urolithiasis).
- APRT (Adenine Phosphoribosyltransferase):

⭐ Lesch-Nyhan syndrome (HGPRT deficiency) presents with hyperuricemia, gout, self-mutilation, and neurological dysfunction (📌 Mnemonic: HGPRT - Hyperuricemia, Gout, Pissed off [aggression, self-mutilation], Retardation, dysTonia).
Pyrimidine Metabolism - Breakdown & Buildup
- Breakdown (Catabolism):
- C, U, T → β-Alanine, β-Aminoisobutyrate, $NH_3$, $CO_2$ (water-soluble).
- Key enzyme: Dihydropyrimidine dehydrogenase (DPD). DPD def.: ↑5-FU toxicity.
- Buildup (De Novo Synthesis):
- Precursors: Glutamine, $CO_2$, Aspartate.
- Key: Carbamoyl Phosphate Synthetase II (CPS II) (cytosolic, rate-limiting).
- Orotic acid → UMP (UMP Synthase).
- Orotic Aciduria: UMP Synthase defect; megaloblastic anemia, orotic aciduria. Rx: Uridine.
- Salvage: Minor pathway.
⭐ Pyrimidine breakdown yields highly water-soluble products (β-alanine, β-aminoisobutyrate, NH3, CO2), unlike purine catabolism, thus no gout-like syndromes.
Clinical Hotspots - Pathway Pathologies
- Gout:
- Hyperuricemia (↑purine breakdown / ↓excretion). Allopurinol inhibits xanthine oxidase.
- Acute inflammatory arthritis (urate crystals), tophi.
- Triggers: alcohol, red meat, fructose.
- Lesch-Nyhan Syndrome:
- X-linked HGPRT deficiency (purine salvage defect).
- Hyperuricemia, gout, self-mutilation, choreoathetosis, intellectual disability.
- 📌 Hyperuricemia, Gout, Pissed off (aggression/self-mutilation), Retardation (intellectual disability), DysTonia.
- Adenosine Deaminase (ADA) Deficiency:
⭐ Adenosine Deaminase (ADA) deficiency causes Severe Combined Immunodeficiency (SCID) due to accumulation of dATP, which is toxic to T and B lymphocytes by inhibiting ribonucleotide reductase.
- Purine Nucleoside Phosphorylase (PNP) Deficiency:
- Autosomal recessive; causes severe T-cell immunodeficiency. Recurrent infections.
High‑Yield Points - ⚡ Biggest Takeaways
- Purine degradation culminates in uric acid; its overproduction or underexcretion causes gout.
- Adenosine Deaminase (ADA) deficiency is a key cause of Severe Combined Immunodeficiency (SCID).
- Lesch-Nyhan syndrome, due to HGPRT deficiency, features hyperuricemia and self-mutilation.
- Pyrimidine degradation yields water-soluble products like β-alanine and β-aminoisobutyrate.
- Salvage pathways are crucial for recycling purine bases, conserving metabolic energy.
- Allopurinol inhibits xanthine oxidase, treating gout by ↓ uric acid production.
- Ribonucleotide reductase is vital for converting ribonucleotides to deoxyribonucleotides for DNA synthesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

