Liver Overview - Metabolic Maestro
- Body's primary metabolic clearinghouse; pivotal for homeostasis.
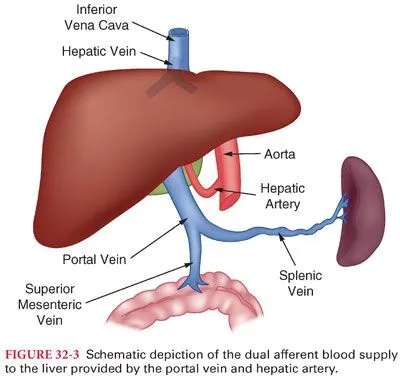
- Unique dual blood supply:
- Portal vein (~75%): nutrient-rich blood from intestines, pancreas, spleen.
- Hepatic artery (~25%): supplies oxygenated blood.
- Strategically located to process absorbed nutrients first.
- Major functions:
- Intermediary metabolism of carbohydrates, fats, proteins.
- Detoxification (e.g., ammonia to urea via urea cycle).
- Synthesis (e.g., albumin, bile, clotting factors).
⭐ Liver is the primary site for ketogenesis during prolonged fasting or low carbohydrate diets, producing ketone bodies (acetoacetate, β-hydroxybutyrate) from acetyl-CoA derived from fatty acid oxidation for use by extrahepatic tissues like brain and muscle as fuel when glucose is scarce. This process spares glucose and protein breakdown. The liver itself cannot utilize ketone bodies as it lacks the enzyme succinyl-CoA:3-ketoacid CoA transferase (thiophorase).
Carbohydrate Metabolism - Sugar Switchboard
- Glucose Buffer: Liver maintains blood glucose ($70-110$ mg/dL) via GLUT2 (insulin-independent transporter).
- Fed State (↑Insulin, ↓Glucagon):
- Glycogenesis: Glucose → Glycogen for storage. Key enzyme: Glycogen synthase.
- Glycolysis/TCA Cycle: Glucose → ATP. Excess Acetyl-CoA → Lipogenesis (fatty acid synthesis).
- HMP Shunt (Pentose Phosphate Pathway): Produces NADPH (for reductive biosynthesis) & Ribose-5-P (for nucleotide synthesis).
- Fasting State (↓Insulin, ↑Glucagon):
- Glycogenolysis: Glycogen → Glucose. Liver glycogen can supply glucose for ~12-18 hours. Key enzyme: Glycogen phosphorylase.
- Gluconeogenesis: Synthesis of glucose from non-carbohydrate precursors (lactate, alanine, glycerol). Key liver-specific enzyme: Glucose-6-phosphatase.
- Fed State (↑Insulin, ↓Glucagon):
- Fructose & Galactose Metabolism: Primarily occurs in the liver; these sugars are converted to glycolytic or gluconeogenic intermediates.
- Key Hepatic Enzymes: Glucokinase (high $K_m$, phosphorylates glucose when abundant), Glucose-6-phosphatase (G6Pase, allows free glucose release into blood).
⭐ The liver's Glucose-6-phosphatase (G6Pase) is crucial for releasing free glucose into the bloodstream to maintain blood glucose levels; muscle lacks G6Pase, so muscle glycogen cannot directly contribute to blood glucose.
Lipid Metabolism - Lipid Logistics
- Liver: Central processing unit for lipids; manages synthesis, storage, distribution.
- Sources of Hepatic Lipids:
- Chylomicron remnants (CR): Dietary TGs; LRP1/LDLR uptake.
- Free Fatty Acids (FFA): From adipose, albumin-bound.
- De novo synthesis: From excess carbohydrates/amino acids.
- Hepatic Lipid Fates & Transport:
- VLDL (ApoB-100): Exports endogenous TGs & cholesterol to periphery.
- HDL (ApoA-I): Synthesized de novo; reverse cholesterol transport.
- β-oxidation: For ATP.
- Ketogenesis: During fasting (e.g., acetoacetate).
- Cholesterol: To bile acids/salts or VLDL.
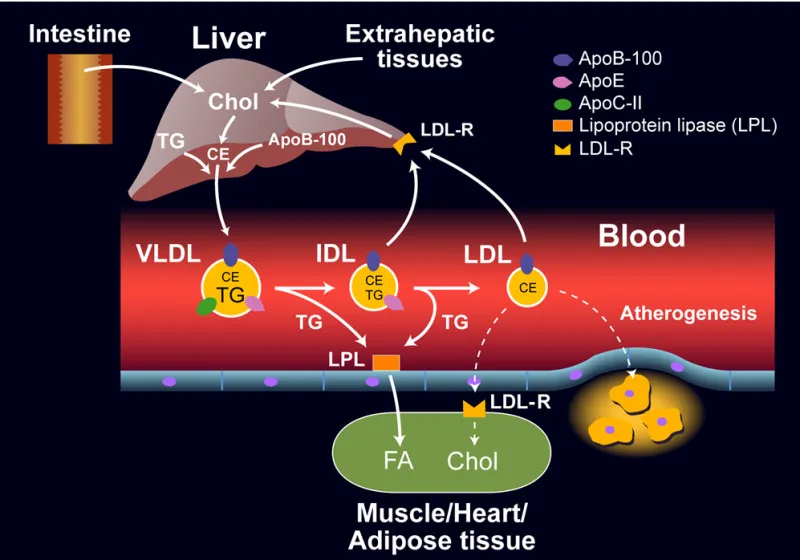
⭐ ApoC-II (on chylomicrons & VLDL) activates lipoprotein lipase (LPL) for TG hydrolysis in peripheral tissues.
Protein & Nitrogen Metabolism - Amino Acid Arena
-
Liver: Central for amino acid (AA) pool management & nitrogen (N) disposal.
- AA Fates: Protein synthesis (e.g., albumin, clotting factors), N-compounds, energy (gluconeogenesis/ketogenesis).
-
Key Reactions:
- Transamination (PLP-Vit B6 dependent, e.g., ALT, AST): Interconverts AAs.
- Deamination (e.g., Glutamate Dehydrogenase - GDH): Releases $NH_3$ from AAs.
-
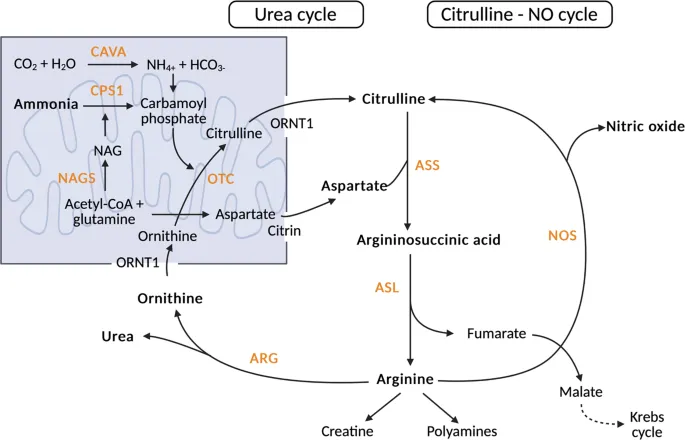
Urea Cycle: Detoxifies $NH_3 \rightarrow$ Urea (less toxic, excreted).
- Location: Mitochondria & Cytosol.
- Rate-limiting enzyme: Carbamoyl Phosphate Synthetase I (CPS-I).
- Allosteric activator: N-Acetylglutamate (NAG) for CPS-I.
⭐ Hyperammonemia (↑$NH_3$) is neurotoxic; features: tremor, slurring, vomiting, cerebral edema. Common in liver failure & Urea Cycle Disorders (UCDs). Ornithine Transcarbamylase (OTC) deficiency is the most common UCD (X-linked recessive).
High‑Yield Points - ⚡ Biggest Takeaways
- Liver is paramount for glucose homeostasis: balancing glycogenesis, glycogenolysis, gluconeogenesis.
- Manages lipid metabolism: including fatty acid synthesis, β-oxidation, ketogenesis, cholesterol, and VLDL synthesis.
- Central to amino acid metabolism: transamination, deamination, urea cycle for nitrogen excretion.
- Key detoxification organ: metabolizes drugs and toxins via Phase I & II reactions.
- Synthesizes essential plasma proteins like albumin, acute phase proteins, and clotting factors.
- Major storage site for glycogen, vitamin A, vitamin B12, and iron.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

