Glucose Transporters: Overview & Families - Sweet Gates
- Membrane proteins vital for transporting glucose across cell membranes.
- Essential as polar glucose cannot readily cross the hydrophobic lipid bilayer.
- Two primary families:
- GLUT (GLUcose Transporter) family: Facilitated diffusion (passive transport).
- SGLT (Sodium-GLucose Transporter) family: Secondary active transport (co-transports glucose with $Na^+$).
- Key players in maintaining systemic glucose homeostasis.
⭐ Glucose, being a polar molecule, cannot diffuse freely across the lipid bilayer and requires specific carrier proteins.
GLUT Family (Facilitated Diffusion) - The Facilitators
GLUT transporters (SLC2A gene family) mediate facilitated glucose diffusion. These integral membrane proteins exhibit tissue-specific expression and varying kinetic properties ($K_m$ values), crucial for glucose homeostasis.
| Transporter | Gene | Key Locations | Approx. $K_m$ & Affinity | Specific Functions/Notes | Clinical/Mnemonic (📌) |
|---|---|---|---|---|---|
| GLUT1 | SLC2A1 | RBCs, brain, placenta | Low ($K_m \approx \textbf{1-2 mM}$), high affinity | Basal glucose uptake; Blood-Brain Barrier (BBB). | 📌 "One for all" (basal). De Vivo disease. |
| GLUT2 | SLC2A2 | Liver, Pancreas ($\beta$-cells), kidney, gut (basolateral) | High ($K_m \approx \textbf{15-20 mM}$), low affinity | Glucose sensor (pancreas); high-capacity, bidirectional (liver). | 📌 "Two-way street". Fanconi-Bickel syndrome. |
| GLUT3 | SLC2A3 | Neurons, placenta | Very Low ($K_m < \textbf{1 mM}$), very high affinity | Main neuronal glucose uptake. | 📌 "Three for brain's glee". |
| GLUT4 | SLC2A4 | Skeletal muscle, adipose tissue, heart | Moderate ($K_m \approx \textbf{5 mM}$), medium affinity | Insulin-regulated glucose uptake. | 📌 "Four for more" (insulin). Type 2 DM. |
| GLUT5 | SLC2A5 | Small intestine (apical), testes, kidney | Fructose specific ($K_m \approx \textbf{6 mM}$ for fructose) | Primarily fructose transporter. | 📌 "Five for Fructose". Fructose malabsorption. |
| GLUT7 | SLC2A7 | Endoplasmic Reticulum (liver, gluconeogenic tissues) | Low $K_m$ | Glucose export from ER (gluconeogenesis/glycogenolysis). | Key in hepatic glucose production. |
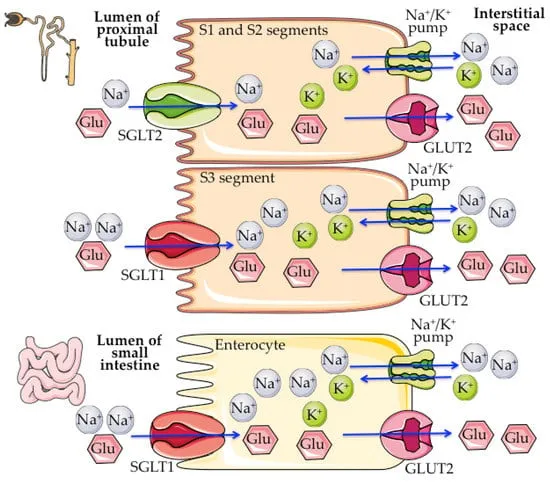
SGLT Family (Secondary Active Transport) - The Co-Riders
- Mechanism: $Na^+$-glucose cotransport (symport). Energy from electrochemical $Na^+$ gradient (via $Na^+$/$K^+$-ATPase).
| Feature | SGLT1 | SGLT2 |
|---|---|---|
| Gene (SLC5A) | SLC5A1 | SLC5A2 |
| Location | Intestine (absorption), Kidney (PCT S3) | Kidney (PCT S1/S2) |
| Stoichiometry | 2 $Na^+$ : 1 Glucose | 1 $Na^+$ : 1 Glucose |
| Affinity/Capacity | ↑ Affinity, ↓ Capacity | ↓ Affinity, ↑ Capacity (bulk reabsorption) |
| Key Role | Glucose-galactose absorption; Final renal glucose capture | Reabsorbs ~90% filtered renal glucose |
| Clinical Note | Mutations: Glucose-galactose malabsorption | Target for SGLT2 inhibitors (e.g., -gliflozins) |
⭐ SGLT2 inhibitors (e.g., canagliflozin, dapagliflozin, empagliflozin) are antidiabetic drugs promoting urinary glucose excretion by blocking glucose reabsorption in proximal renal tubules.
Clinical Significance & Regulation - Sweet Malfunctions & Masters
- Regulation
- Insulin: ↑ GLUT4 translocation (muscle, adipose), ↑ glucose uptake.
- Genetic Disorders
- GLUT1 Deficiency (De Vivo): Low CSF glucose, seizures, dev. delay. Ketogenic diet.
⭐ GLUT1 Deficiency Syndrome typically presents with infantile seizures, developmental delay, microcephaly, and is managed with a ketogenic diet to provide an alternative fuel source for the brain.
- Fanconi-Bickel (GLUT2): Impaired glucose/galactose use; hepatorenal glycogen, rickets, FTT.
- Glucose-Galactose Malabsorption (SGLT1): Neonatal osmotic diarrhea (glucose/galactose). Fructose diet.
- 📌 SGLT1: Salty Gut Loses Two (Glucose, Galactose).
- GLUT1 Deficiency (De Vivo): Low CSF glucose, seizures, dev. delay. Ketogenic diet.
- Pharmacology
- SGLT2 inhibitors (-gliflozins): Block renal glucose reabsorption (PCT); for T2DM, HF.
- Targeting GLUTs (e.g., GLUT1): Potential in cancer therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- GLUT1: Key for RBCs & brain; basal glucose uptake; insulin-independent.
- GLUT2: Liver, pancreatic β-cells; high Km (low affinity), high capacity; glucose sensor.
- GLUT3: Neurons, placenta; low Km (high affinity); ensures brain's glucose supply.
- GLUT4: Skeletal muscle, adipose tissue; insulin-dependent; translocates to membrane with insulin.
- GLUT5: Small intestine (jejunum); primarily a fructose transporter.
- SGLT1: Small intestine, kidney; Na+-glucose cotransporter (active); absorbs glucose & galactose.
- SGLT2: Kidney (PCT); Na+-glucose cotransporter; reabsorbs glucose; target for gliflozin drugs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more