Ca2+ Roles & Levels - Calcium Command Center
- Key Roles:
- Second messenger (signal transduction)
- Muscle contraction, neurotransmitter release
- Enzyme cofactor (e.g., calmodulin)
- Blood coagulation
- Bone & teeth mineralization
- Concentration Gradients:
- Cytosolic: ~100 nM ($10^{-7}M$)
- Extracellular: ~1-2 mM ($10^{-3}M$)
- ER/SR lumen: ~0.1-1 mM
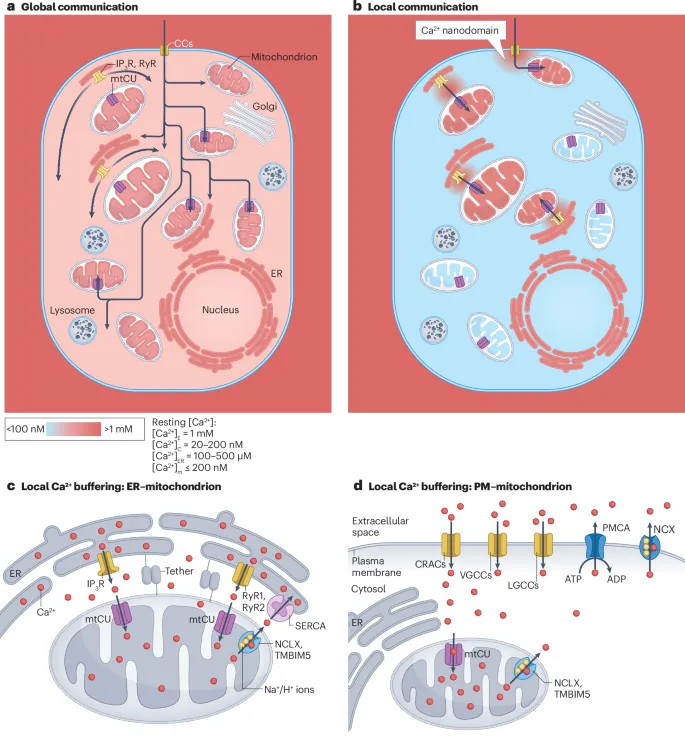
⭐ The steep electrochemical gradient for calcium ions across the plasma membrane is crucial for its role as a rapid signaling ion.
Ca2+ Transport Systems - Calcium Highway Patrol
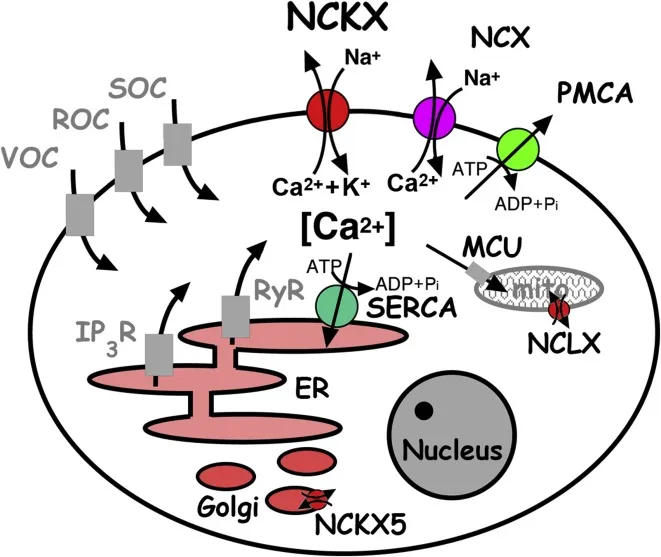
- Overview: Cells maintain low cytosolic $Ca^{2+}$ (
100 nM) vs. high extracellular $Ca^{2+}$ (1-2 mM) via diverse transporters. Gradient crucial for signaling.
| Feature | $Ca^{2+}$ Channels | $Ca^{2+}$ Pumps (ATPases) | $Ca^{2+}$ Exchangers |
|---|---|---|---|
| Mechanism | Facilitated diffusion | Active transport | Secondary active transport |
| Energy | Uses gradient; no direct ATP | ATP hydrolysis (PMCA, SERCA) | Uses another ion's gradient ($Na^{+}$) |
| Direction | Influx (down gradient) | Efflux/into organelles (up gradient) | Primarily efflux (NCX, NCKX) |
| Examples | VOCs, ROCs, SOCs | PMCA, SERCA | NCX ($Na^{+}/Ca^{2+}$), NCKX ($Na^{+}/K^{+}/Ca^{2+}$) |
- Regulation: Kinases, phosphatases, $Ca^{2+}$ itself (e.g., calmodulin).
- 📌 Mnemonic (SERCA): SERiously CAlms CAlcium (in SR/ER).
Ca2+ ATPases: SERCA/PMCA - Calcium's Power Pumps
Ca2+ ATPases are P-type pumps essential for maintaining low cytosolic Ca2+ concentrations. They function via a catalytic cycle involving phosphorylation and conformational changes (E1-E2 states): $E1 + Ca^{2+}{cyt} + ATP \rightleftharpoons E1 \cdot Ca^{2+} \cdot ATP \rightarrow E1 \sim P \cdot Ca^{2+} \rightarrow E2 \sim P \cdot Ca^{2+} \rightarrow E2 \sim P + Ca^{2+}{lum/ext} + ADP \rightarrow E2 + P_i \rightarrow E1$
Two primary types:
- 📌 SERCA: Sarcoplasmic/Endoplasmic Reticulum Ca2+-ATPase
- 📌 PMCA: Plasma Membrane Ca2+-ATPase
Comparison of SERCA and PMCA:
| Feature | SERCA (Sarco/Endoplasmic Reticulum Ca2+-ATPase) | PMCA (Plasma Membrane Ca2+-ATPase) |
|---|---|---|
| Isoforms | SERCA1, SERCA2 (2a, 2b), SERCA3 | PMCA1, PMCA2, PMCA3, PMCA4 |
| Location | SR/ER membrane | Plasma membrane |
| Stoichiometry | 2 Ca2+ / 1 ATP | 1 Ca2+ / 1 ATP |
| Specific Regulators | Phospholamban (PLN), Sarcolipin (SLN) | Calmodulin, Acidic phospholipids, Protein Kinases (PKA, PKC) |
| Affinity for Ca2+ | High (nM range, ~0.1-0.5 µM) | Lower (µM range, ~10 µM), ↑ with Calmodulin to ~0.5 µM |
Post-Albers Cycle for Ca2+-ATPase:
Clinical: Ca2+ Pumps - Calcium Chaos Clinic
- SERCA Pump Dysfunction:
- Darier's Disease: ATP2A2 (SERCA2) mutation; skin lesions.
- Brody Disease: ATP2A1 (SERCA1) mutation; muscle cramps, impaired relaxation.
- Heart Failure: ↓SERCA2 activity impairs cardiac relaxation.
- PMCA Pump Dysfunction:
- Hypertension: Altered PMCA function implicated.
- Rare mutations: Can cause ataxia, hearing loss.
- Pharmacological Note:
-
⭐ Thapsigargin: Specific SERCA inhibitor; research tool for Ca2+ signaling.
-
High‑Yield Points - ⚡ Biggest Takeaways
- Calcium ATPases (SERCA & PMCA) are P-type ATPases that maintain low cytosolic Ca²⁺.
- SERCA pumps Ca²⁺ into the sarcoplasmic/endoplasmic reticulum (SR/ER).
- PMCA expels Ca²⁺ from the cell via the plasma membrane.
- Both use ATP hydrolysis to transport Ca²⁺ against its electrochemical gradient.
- Calmodulin stimulates PMCA activity.
- Phospholamban (in cardiac muscle) inhibits SERCA; its phosphorylation relieves this inhibition.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

