Eicosanoid Basics - Tiny Lipid Titans
- Potent, short-lived local hormones (autacoids) from $C_{20}$ PUFAs.
- Main precursor: Arachidonic Acid (AA), an $\omega-6$ fatty acid.
- Classes: Prostaglandins (PGs), Thromboxanes (TXs) via cyclooxygenase (COX).
- Leukotrienes (LTs), Lipoxins (LXs) via lipoxygenase (LOX).
- Synthesized "on demand"; not stored.
- Mediate inflammation, pain, fever, platelet aggregation, smooth muscle.
⭐ Phospholipase A2 (PLA2) is the key enzyme releasing arachidonic acid from membrane phospholipids.
AA Metabolism - The Eicosanoid Factory
- Substrate: Arachidonic Acid (AA), a $C_{20:4}(\omega-6)$ PUFA.
- Released from membrane phospholipids by Phospholipase A₂ (PLA₂).
- PLA₂ inhibited by corticosteroids (via lipocortin).
- Pathways & Products:
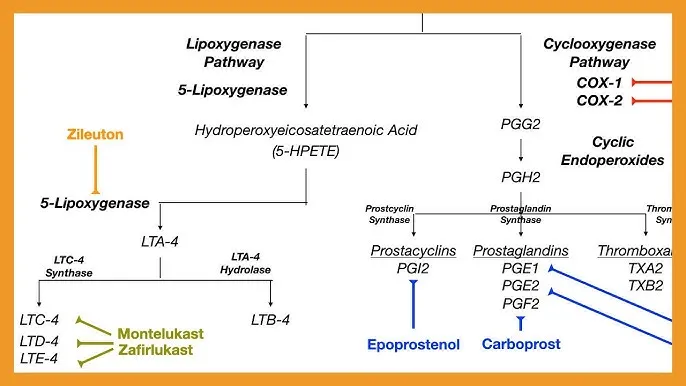
- Cyclooxygenase (COX) → PGH₂ (unstable intermediate) → Prostaglandins (PGs - inflammation, pain), Prostacyclin (PGI₂ - vasodilation, anti-platelet), Thromboxane A₂ (TXA₂ - vasoconstriction, pro-platelet).
- COX-1 (constitutive), COX-2 (inducible).
- Inhibited by NSAIDs.
- Lipoxygenase (LOX) → Leukotrienes (LTs e.g., LTB₄ - chemotaxis; LTC₄, LTD₄, LTE₄ - bronchoconstriction, SRS-A), Lipoxins (anti-inflammatory).
- 5-LOX inhibitors (Zileuton), LT receptor antagonists (Montelukast).
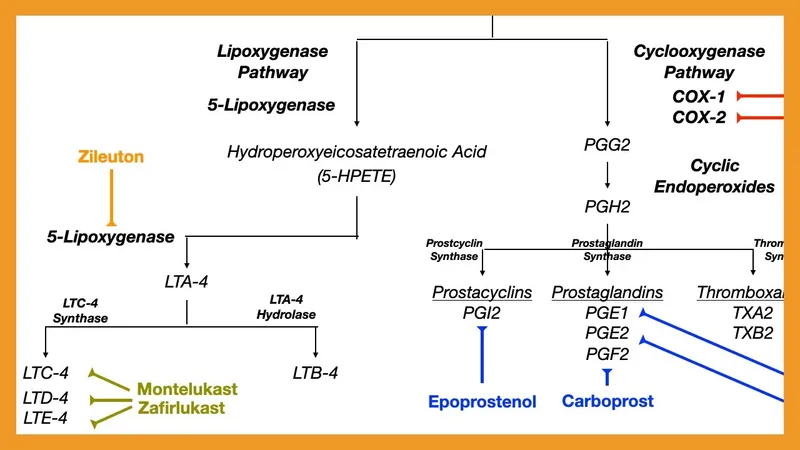
- 5-LOX inhibitors (Zileuton), LT receptor antagonists (Montelukast).
- Cyclooxygenase (COX) → PGH₂ (unstable intermediate) → Prostaglandins (PGs - inflammation, pain), Prostacyclin (PGI₂ - vasodilation, anti-platelet), Thromboxane A₂ (TXA₂ - vasoconstriction, pro-platelet).
⭐ Aspirin irreversibly acetylates COX-1 & COX-2; its anti-platelet effect lasts for the platelet's lifespan (8-10 days) due to TXA₂ inhibition.
Prostaglandins/Thromboxanes - Inflammation & Clot Crew
- From arachidonic acid via COX pathway (COX-1/COX-2).
- Prostaglandins (PGs):
- PGI₂ (Prostacyclin): Vasodilation, ↓platelet aggregation. Endothelial.
- PGE₁: Maintains PDA (Alprostadil).
- PGE₂: Uterine contraction, pain, fever (Dinoprostone).
- PGF₂α: Uterine contraction, bronchoconstriction (Latanoprost).
- Thromboxanes (TXs):
- TXA₂: Vasoconstriction, ↑platelet aggregation. Platelet origin.
- 📌 PGI₂: Platelet Inhibitor; TXA₂: Thrombus Activator.
- NSAIDs inhibit COX, ↓PG & TX.
⭐ Aspirin irreversibly inhibits platelet COX-1, ↓TXA₂ for platelet lifespan (7-10 days), key antiplatelet action.
Leukotrienes/Lipoxins - Allergy & Resolution Squad
- Leukotrienes (LTs): Pro-inflammatory; from Arachidonic Acid via 5-Lipoxygenase (5-LOX) & FLAP.
- LTB4: Neutrophil chemoattractant, ↑adhesion.
- Cysteinyl LTs (LTC4, LTD4, LTE4): Bronchoconstriction, ↑vascular permeability, mucus. (📌 "C" for Constriction). Formerly SRS-A.
- Drugs: Zileuton (5-LOX inh.); Montelukast (CysLT1 antag.).
- Lipoxins (LXs): Anti-inflammatory "stop signals"; promote resolution.
- LXA4, LXB4.
- Synthesized by sequential LOX actions (e.g., 15-LOX then 5-LOX).
- Inhibit neutrophil recruitment, stimulate monocyte clearance.
⭐ Aspirin acetylates COX-2, shifting it to produce Aspirin-Triggered Lipoxins (e.g., 15-epi-LXA4), enhancing resolution.
Eicosanoid Drugs - Drug Targets Galore
- COX Inhibitors (NSAIDs): Block cyclooxygenase → ↓Prostaglandins, Thromboxanes.
- Non-selective: Aspirin (irreversible), Ibuprofen, Diclofenac. Uses: inflammation, pain, fever. Aspirin: antiplatelet.
- COX-2 selective: Celecoxib, Etoricoxib. Less GI toxicity, ↑CV risk.
- Leukotriene Modifiers:
- 5-LOX Inhibitor: Zileuton (asthma).
- LT Receptor Antagonists (📌 LTRA): MonteLUKAST, ZafirLUKAST (asthma, allergic rhinitis).
- Prostaglandin Analogs:
- PGE1: Misoprostol (ulcer prevention), Alprostadil (PDA, ED).
- PGF2α: Latanoprost (glaucoma), Carboprost (PPH).
- Corticosteroids: Inhibit Phospholipase A2 → ↓Arachidonic Acid → ↓all eicosanoids. Broad anti-inflammatory.
⭐ Aspirin irreversibly acetylates COX, inhibiting platelet aggregation for their lifespan (8-10 days).
High‑Yield Points - ⚡ Biggest Takeaways
- Eicosanoids (PGs, TXs, LTs) derive from arachidonic acid via COX or lipoxygenase pathways.
- COX-1 (constitutive) & COX-2 (inducible) are key for PG/TX synthesis; inhibited by NSAIDs.
- Aspirin irreversibly inhibits COX; corticosteroids block phospholipase A₂, preventing AA release.
- Leukotrienes (via lipoxygenase) mediate allergic reactions and inflammation (e.g., asthma).
- PGI₂ (prostacyclin) causes vasodilation & ↓platelet aggregation; TXA₂ causes vasoconstriction & ↑platelet aggregation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more