FA Activation & Transport - The Entry Ticket
- Activation (Cytosol):
- Primes FAs for degradation.
- Enzyme: Acyl-CoA Synthetase (Thiokinase) (OMM).
- Reaction: $FA + ATP + CoASH \rightarrow Acyl-CoA + AMP + PPi$.
- Energy cost: 2 ATP equivalents (ATP $\rightarrow$ AMP).
- Transport into Mitochondria (Carnitine Shuttle):
- For Long-Chain Fatty Acids (LCFA, >12C); shorter chains diffuse.
- Rate-limiting for LCFA oxidation.
- 📌 Mnemonic: "CARnitine = CAR for Acyl-CoA into mitochondria."
- Key steps:
- CPT I (OMM): $Acyl-CoA + Carnitine \rightarrow Acylcarnitine$. Inhibited by Malonyl-CoA.
- Translocase (IMM): Acylcarnitine (in) / Carnitine (out).
- CPT II (IMM): $Acylcarnitine \rightarrow Acyl-CoA (matrix) + Carnitine$.
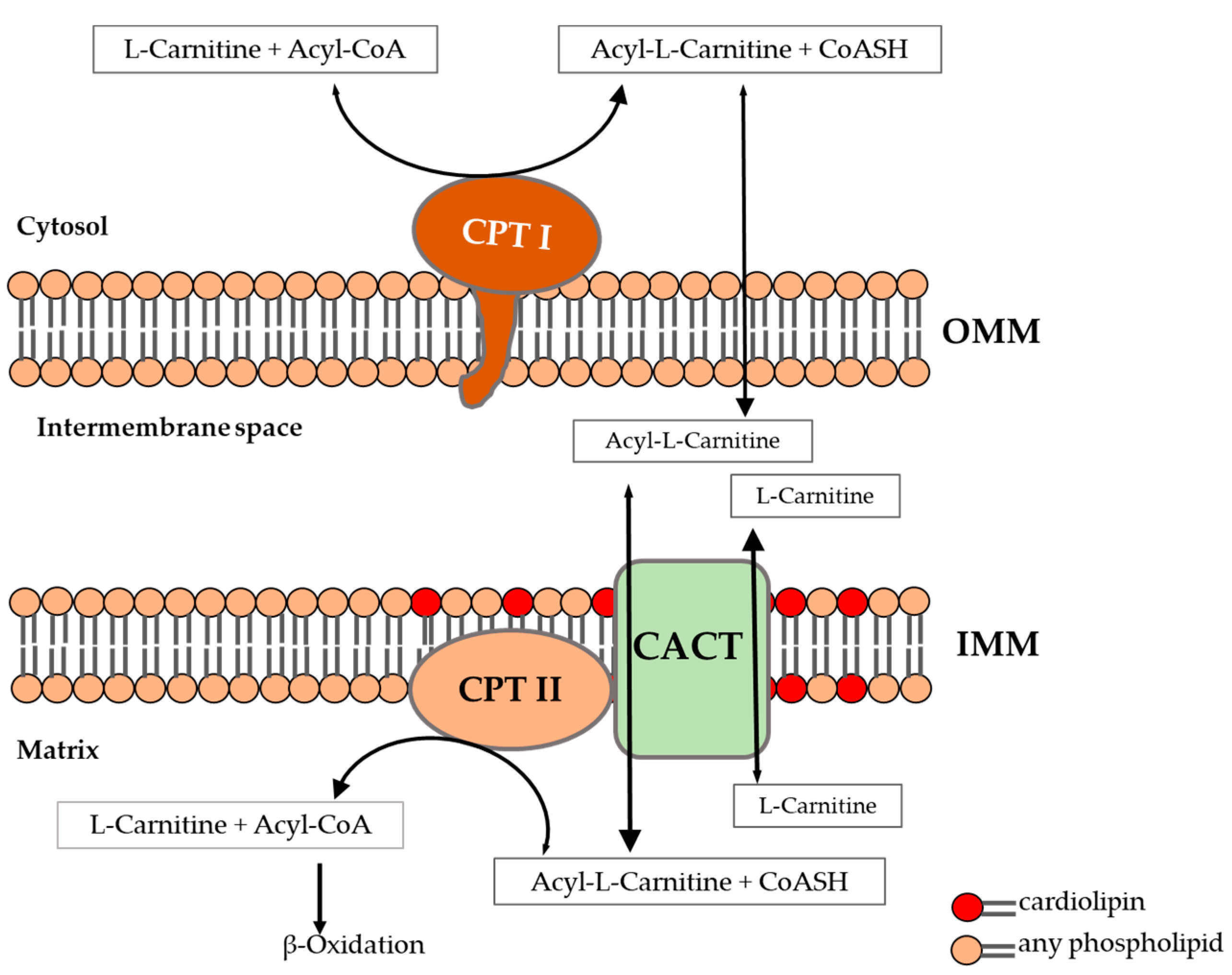
> ⭐ Carnitine shuttle defects (CPT I/II deficiency) cause hypoketotic hypoglycemia & muscle weakness, especially during fasting.
β-Oxidation Spiral - Chopping Champs
- Core Process: Iterative four-step cycle in mitochondrial matrix, cleaving 2-C units (Acetyl-CoA) from fatty acyl-CoA.
- The Four Recurring Enzymatic Steps: 📌 Mnemonic for reaction types: "Old Hippies Often Trip" (Oxidation, Hydration, Oxidation, Thiolysis)
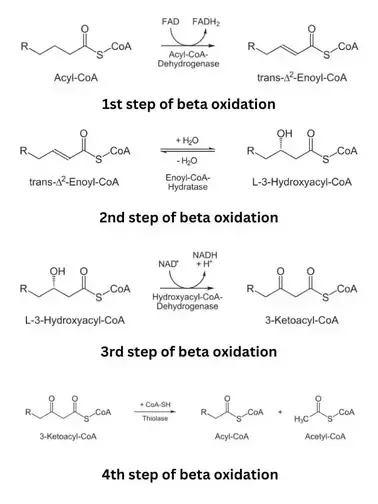
- 1. Oxidation: Acyl-CoA Dehydrogenase converts fatty acyl-CoA to Trans-Δ²-Enoyl-CoA.
- Coenzyme: $FAD \rightarrow FADH_2$.
- 2. Hydration: Enoyl-CoA Hydratase adds $H_2O$ across double bond, forming L-β-Hydroxyacyl-CoA.
- 3. Oxidation: β-Hydroxyacyl-CoA Dehydrogenase oxidizes hydroxyl to keto group, forming β-Ketoacyl-CoA.
- Coenzyme: $NAD^+ \rightarrow NADH + H^+$.
- 4. Thiolysis: Thiolase (β-Ketothiolase) cleaves β-Ketoacyl-CoA with CoA-SH.
- Products: Acetyl-CoA & fatty acyl-CoA (shortened by 2C, i.e., $C_{n-2}$ from $C_n$).
- 1. Oxidation: Acyl-CoA Dehydrogenase converts fatty acyl-CoA to Trans-Δ²-Enoyl-CoA.
⭐ Each round of β-oxidation yields 1 FADH₂, 1 NADH, & 1 Acetyl-CoA. These fuel ATP synthesis via oxidative phosphorylation.
Energetics & Regulation - Fuel & Control
Energetics (Palmitate C16):
- Activation: $-2$ ATP.
- 7 β-oxidation cycles yield:
- $7 \text{ FADH}_2 \rightarrow 10.5 \text{ ATP}$ ($7 \times 1.5$)
- $7 \text{ NADH} \rightarrow 17.5 \text{ ATP}$ ($7 \times 2.5$)
- 8 Acetyl-CoA (via TCA cycle) $\rightarrow 80 \text{ ATP}$ ($8 \times 10$).
- Net ATP yield: $\textbf{106 ATP}$ for Palmitate.
- Overall: $PalmitoylCoA + 7FAD + 7NAD⁺ + 7CoA + 7H_2O \rightarrow 8 AcetylCoA + 7FADH_2 + 7NADH + 7H⁺$
Regulation:
- CPT I (Rate-limiting step): Located on outer mitochondrial membrane.
⭐ Malonyl-CoA (from FA synthesis) allosterically inhibits CPT I, preventing futile cycling.
- Hormonal Control:
- Glucagon/Epinephrine: ↑ Lipolysis (HSL), ↑ FFAs $\rightarrow$ ↑ β-oxidation.
- Insulin: ↓ Lipolysis, ↑ Malonyl-CoA (via ACC activation) $\rightarrow$ ↓ β-oxidation.
- Energy Status (Feedback Inhibition):
- High ATP/ADP ratio & High NADH/NAD⁺ ratio $\rightarrow$ ↓ β-oxidation (inhibits dehydrogenases).
Special FA Oxidation & Disorders - Oddballs & Ouchies
- Odd-chain FA (e.g., C17):
- Propionyl-CoA → Succinyl-CoA (TCA).
- Enzymes: Propionyl-CoA Carboxylase (Biotin), Methylmalonyl-CoA Mutase (Vit B12). 📌 Biotin & B12 help odd FAs enter TCA.
- Defect: Methylmalonic acidemia.
- Unsaturated FA:
- Need Isomerase, Reductase.
- Peroxisomal β-Oxidation (VLCFA > C22):
- Acyl-CoA Oxidase ($FADH_2 \rightarrow H_2O_2$); Catalase.
- Zellweger Syndrome: Peroxisome biogenesis defect.
- X-ALD: ABCD1 (VLCFA transporter) defect.
- α-Oxidation (Phytanic Acid):
- Peroxisomal.
- Refsum Disease: Phytanoyl-CoA hydroxylase def.
- ω-Oxidation (ER):
- Minor; forms dicarboxylic acids. ↑ in β-oxidation defects.
⭐ MCAD (Medium-chain acyl-CoA dehydrogenase) deficiency is the most common inherited defect of FA oxidation, presenting with hypoketotic hypoglycemia and dicarboxylic aciduria.
High‑Yield Points - ⚡ Biggest Takeaways
- Primary site: Mitochondrial matrix; Peroxisomes for Very Long Chain Fatty Acids (VLCFAs).
- Rate-limiting enzyme: Carnitine Palmitoyltransferase I (CPT-I), inhibited by Malonyl-CoA.
- Carnitine shuttle: Essential for LCFA transport into mitochondria.
- β-oxidation products (per cycle): 1 Acetyl-CoA, 1 NADH, 1 FADH₂.
- Odd-chain FAs: Yield Propionyl-CoA, converted to Succinyl-CoA (TCA intermediate).
- MCAD deficiency: Most common defect; presents with hypoketotic hypoglycemia, dicarboxylic aciduria.
- Zellweger syndrome: Impaired peroxisomal oxidation of VLCFAs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

