Heme Structure & Synthesis Intro - Blood's Red Heart
- Heme: A heterocyclic porphyrin ring (Protoporphyrin IX) complexed with a ferrous iron ($Fe^{2+}$) atom.
- Essential for:
- Oxygen transport (hemoglobin, myoglobin).
- Electron transport (cytochromes).
- Enzyme activity (catalase, peroxidase).
- Synthesis primarily in bone marrow (for Hb) & liver (for cytochromes); occurs in mitochondria & cytosol.
- Initial step: $Glycine + Succinyl CoA \rightarrow \delta-Aminolevulinic Acid (ALA)$.
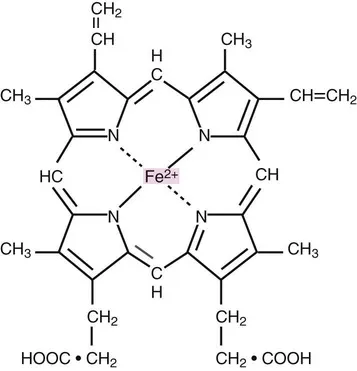
⭐ Heme contains ferrous ($Fe^{2+}$) iron. Oxidation to ferric ($Fe^{3+}$) state forms methemoglobin, which cannot bind oxygen effectively.
Heme Synthesis Pathway - The Heme Assembly Line
- Pathway Sites: Mitochondria (start/end) & Cytosol (intermediate steps).
- Key Cofactors: Pyridoxal Phosphate (PLP/Vit B6) for ALAS; Fe²⁺ for Ferrochelatase.
- Lead Inhibition: Affects ALA Dehydratase (ALAD) and Ferrochelatase.
- 📌 Enzyme Order: Alcoholics Anonymous Participants Usually Understand Complicated Problems Fast (ALAS, ALAD, PBGD, UROS, UROD, CPOX, PPOX, Ferrochelatase).
⭐ Rate-limiting enzyme: ALA Synthase (ALAS).
- Location: Mitochondria.
- Regulation: ↓ by Heme (feedback inhibition); ↑ by drugs inducing CYP450 (e.g., barbiturates, anti-epileptics) which deplete heme. Requires PLP (Vit B6).
Porphyrias Overview - Heme's Dark Side
- Genetic disorders of heme synthesis; enzyme deficiencies lead to accumulation of specific porphyrin precursors.
- Clinical features vary: neurovisceral, cutaneous photosensitivity, or both.
- Classified as erythropoietic or hepatic based on primary organ of enzyme defect.
⭐ Drugs precipitating acute porphyria attacks (e.g., Acute Intermittent Porphyria - AIP): Barbiturates, Sulphonamides, Anticonvulsants (Phenytoin, Carbamazepine), Griseofulvin, Alcohol. 📌 Mnemonic: Bad Sun Affects Great Porphyrics (Barbiturates, Sulphonamides, Anticonvulsants, Griseofulvin, Progestogens/Painkillers/Alcohol).
Major Porphyrias - The Symptom Syndromes
- Acute Intermittent Porphyria (AIP): Autosomal Dominant (AD). Neurovisceral symptoms (abdominal pain, neuropathy, psychiatric). No photosensitivity.
- Enzyme defect: Porphobilinogen (PBG) Deaminase.
- Urine: ↑ Aminolevulinic Acid (ALA), ↑ PBG (darkens on standing, port-wine color).
⭐ AIP: 5 P's - Painful abdomen, Polyneuropathy, Psychological disturbances, Precipitated by drugs (e.g., barbiturates, sulfa), Purple pee.
- Porphyria Cutanea Tarda (PCT): Most common porphyria. AD or acquired. Photosensitivity (vesicles, bullae, skin fragility on sun-exposed areas).
- Enzyme defect: Uroporphyrinogen Decarboxylase.
- Urine: ↑ Uroporphyrin (tea-colored or pink fluorescence under Wood's lamp).
- Triggers: Hepatitis C, HIV, alcohol, estrogens, iron overload.
- Erythropoietic Protoporphyria (EPP): AD. Early onset photosensitivity (non-blistering; burning, itching, pain, swelling within minutes of sun exposure).
- Enzyme defect: Ferrochelatase.
- Blood/Stool: ↑ Protoporphyrin.
- Congenital Erythropoietic Porphyria (CEP) (Gunther Disease): Autosomal Recessive (AR). Severe photosensitivity from infancy, mutilation, hemolytic anemia, erythrodontia (red-brown teeth).
- Enzyme defect: Uroporphyrinogen III Synthase.
- Urine: ↑ Uroporphyrin I, Coproporphyrin I (red-pink).

Lead Poisoning & Heme - The Toxic Intruder
- Lead (Pb) toxicity, an acquired porphyrinopathy, disrupts heme synthesis.
- Key enzymes inhibited: ALA Dehydratase (ALAD) & Ferrochelatase.
- Accumulation: ↑ δ-Aminolevulinic acid (ALA), ↑ Protoporphyrin IX.
- Clinical features: Microcytic anemia (basophilic stippling), abdominal colic, peripheral neuropathy, "lead lines" on gums (Burton's lines).
- Diagnosis: ↑ Blood lead levels, ↑ urinary ALA, ↑ Free Erythrocyte Protoporphyrin (FEP) or Zinc Protoporphyrin (ZPP).

⭐ Enzymes inhibited by lead: ALA Dehydratase & Ferrochelatase.
High‑Yield Points - ⚡ Biggest Takeaways
- ALA synthase is the rate-limiting enzyme in heme synthesis, requiring PLP (Vitamin B6).
- Lead poisoning inhibits ALA dehydratase and ferrochelatase, causing microcytic anemia and ↑ protoporphyrin.
- Acute Intermittent Porphyria (AIP): Autosomal dominant; PBG deaminase (HMB synthase) deficiency. Presents with 5 Ps: Painful abdomen, Port-wine urine, Polyneuropathy, Psychological disturbances, Precipitated by drugs (e.g., barbiturates, P450 inducers). No photosensitivity.
- Porphyria Cutanea Tarda (PCT): Uroporphyrinogen decarboxylase deficiency. Photosensitivity, blisters on sun-exposed areas. Most common porphyria.
- Sideroblastic anemia: Defective heme synthesis (e.g., ALA synthase deficiency or lead poisoning) leading to iron accumulation in mitochondria; ring sideroblasts in bone marrow.
- Heme synthesis begins with Glycine + Succinyl CoA in the mitochondria to form δ-ALA.
- Treatment for acute porphyria attacks includes glucose and hemin, which inhibit ALA synthase activity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

