IEM Overview & Screening - Tiny Troubles
- Definition: Inherited single-gene defects; enzyme/transporter dysfunction disrupts metabolic pathways.
- Classification (Broad):
- Small molecule (aminoacidopathies, organic acidemias, UCDs, FAODs).
- Large molecule (LSDs, mitochondrial disorders).
- Clinical Clues (Red Flags):
- Neonatal: Poor feeding, vomiting, lethargy, seizures.
- Biochemical: Hypoglycemia, metabolic acidosis (↑AG), hyperammonemia.
- Organ: Hepatosplenomegaly, cardiomyopathy.
- Sensory: Cataracts, corneal clouding.
- Unusual odors (e.g., mousy - PKU).
- Newborn Screening (NBS):
- Critical for early diagnosis & intervention.
- Method: Tandem Mass Spectrometry (MS/MS) on dried blood spots.
⭐ Most Inborn Errors of Metabolism (IEMs) are autosomal recessive, though notable exceptions like Ornithine Transcarbamylase (OTC) deficiency (X-linked) and Fabry disease (X-linked) exist.

Carbohydrate Metabolism Disorders - Sugar Storms
- Glycogen Storage Diseases (GSDs):
- Von Gierke (Type I): Glucose-6-phosphatase def. Severe fasting hypoglycemia, hepatomegaly, lactic acidosis, ↑uric acid.
- Pompe (Type II): Lysosomal $\alpha$-1,4-glucosidase def. Cardiomegaly, muscle weakness. 📌 Pompe affects Pump (heart).
- Cori (Type III): Debranching enzyme def. Milder Type I features, muscle involvement.
- McArdle (Type V): Muscle glycogen phosphorylase def. Exercise intolerance, cramps, myoglobinuria.
- Galactosemia:
- Classic (GALT def.): Galactose-1-phosphate uridyltransferase def. Jaundice, hepatomegaly, cataracts, E. coli sepsis. Avoid galactose/lactose.
- GALK def.: Galactokinase def. Cataracts only.
- Hereditary Fructose Intolerance (HFI): Aldolase B def. Hypoglycemia, vomiting, jaundice on fructose/sucrose intake.
⭐ Von Gierke's Disease (GSD Type Ia), a defect in glucose-6-phosphatase, presents with severe fasting hypoglycemia, hepatomegaly, lactic acidosis, and hyperuricemia.
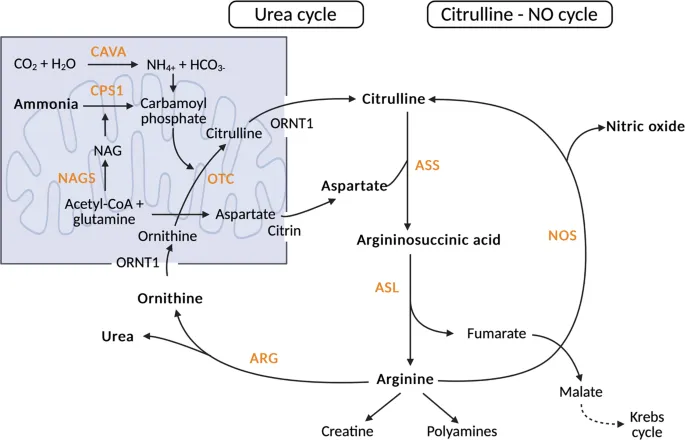
Amino Acid, Organic Acid & Urea Cycle Defects - Protein & Ammonia Perils
- AA Defects:
- PKU: ↓PAH, ↑Phe. Mousy odor.
- MSUD: ↓BCKDH, ↑BCAAs. Maple syrup urine.
- Alkaptonuria: ↓HGD, ↑HGA. Dark urine, ochronosis.
- Homocystinuria: ↓CBS. ↑HCY. Lens subluxation, thrombosis.
- Tyrosinemia I: ↓FAH. Cabbage odor. Liver/kidney failure.
- OA Defects: Acidosis, hyperammonemia.
- Methylmalonic Acidemia (MMA): ↓Methylmalonyl-CoA mutase.
- Propionic Acidemia (PA): ↓Propionyl-CoA carboxylase.
- UCDs: Hyperammonemia, ↓BUN.
- OTC Deficiency: X-linked. ↑Orotic acid.
⭐ Phenylketonuria (PKU) is caused by phenylalanine hydroxylase deficiency, leading to accumulation of phenylalanine; a mousy or musty odor of urine/sweat is characteristic if untreated.
Lysosomal & Peroxisomal Storage - Cellular Clutter
- Lysosomal Storage Disorders (LSDs): Defective lysosomal enzymes → substrate accumulation.
- Tay-Sachs: Hexosaminidase A deficiency → GM2 ganglioside accumulation; cherry-red spot, neurodegeneration. 📌 Tay-SaX lacks heXosaminidase.
- Niemann-Pick: Sphingomyelinase deficiency → sphingomyelin accumulation; hepatosplenomegaly, cherry-red spot (Type A).
- Gaucher: Glucocerebrosidase deficiency → glucocerebroside; hepatosplenomegaly, pancytopenia, bone crises. "Crumpled tissue paper" macrophages.
- Fabry: α-galactosidase A deficiency → globotriaosylceramide (Gb3); X-linked; angiokeratomas, renal failure, neuropathy.
- Mucopolysaccharidoses (MPS): Defective degradation of glycosaminoglycans (GAGs).
- Hurler (MPS I): α-L-iduronidase deficiency; coarse facies, corneal clouding.
- Hunter (MPS II): Iduronate-2-sulfatase deficiency; X-linked; NO corneal clouding. 📌 Hunters see clearly (no corneal clouding) and aim for the X.

- Peroxisomal Disorders: Defective peroxisome biogenesis or enzyme function.
- Zellweger Syndrome: PEX gene mutations → empty peroxisomes; craniofacial dysmorphism, hypotonia, seizures.
- X-linked Adrenoleukodystrophy (X-ALD): ABCD1 gene defect → VLCFA accumulation; adrenal insufficiency, neurological decline.
⭐ Gaucher disease, the most common lysosomal storage disorder, is due to glucocerebrosidase deficiency, leading to accumulation of glucocerebroside in macrophages (Gaucher cells).
High‑Yield Points - ⚡ Biggest Takeaways
- Most IEMs are autosomal recessive; notable exceptions: Hunter's (XLR), OTC deficiency (XLR).
- PKU: Phenylalanine hydroxylase deficiency; mousy odor, CNS effects; dietary restriction is key.
- Alkaptonuria: Homogentisate oxidase deficiency; dark urine on standing, ochronosis (dark cartilage).
- MSUD: Branched-chain ketoacid dehydrogenase deficiency; sweet/burnt sugar urine odor, neurotoxicity.
- Galactosemia (Classic): GALT deficiency; neonatal jaundice, cataracts, risk of E. coli sepsis.
- Von Gierke's (GSD I): Glucose-6-phosphatase deficiency; severe fasting hypoglycemia, hepatomegaly, lactic acidosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more