Bilirubin Metabolism - Heme's Transformation Tale
Error generating content for this concept group: Failed to process successful response
Jaundice Classification - When Yellow Flags Fly
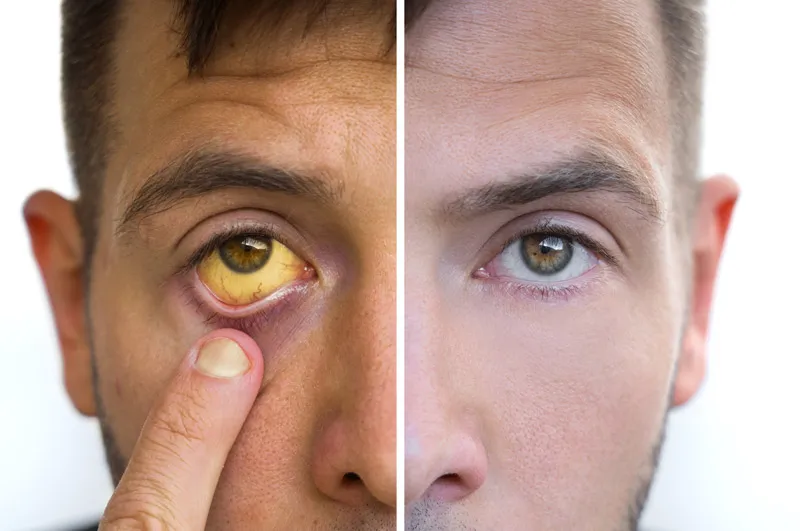
Jaundice (icterus): Clinically evident yellowish pigmentation of skin, sclera, and mucous membranes due to hyperbilirubinemia (serum bilirubin typically > 2-3 mg/dL). It's a key sign of liver or hematological disorders, classified by dysfunction site:
| Feature | Pre-hepatic (Hemolytic) | Hepatic (Hepatocellular/Intrahepatic) | Post-hepatic (Obstructive/Cholestatic) |
|---|---|---|---|
| Primary Defect | ↑ Bilirubin production (hemolysis) | ↓ Hepatic processing (hepatitis, cirrhosis) | ↓ Bile drainage (gallstones, tumor) |
| Serum Bilirubin | Unconjugated ↑ (>80%) | Mixed or specific type (Gilbert's, DJS) | Conjugated ↑ (>50%) |
| Urine Bilirubin | Absent | Present (if conj. ↑) | Present (dark urine) |
| Urine Urobilinogen | ↑ | Normal / ↓ / ↑ (variable) | ↓ or Absent |
| Stool Color | Normal / Dark | Normal / Pale | Pale (acholic) |
| Key LFTs | LDH ↑ | AST/ALT ↑↑ | ALP/GGT ↑↑ |
Specific Jaundice Conditions - Syndromes & Small Fry
- Unconjugated Hyperbilirubinemia (Inherited):
- Gilbert's Syndrome: Mild ↓ UGT1A1 activity. Intermittent jaundice (stress, fasting). Benign.
⭐ Gilbert's syndrome is typically a benign condition characterized by mild, fluctuating unconjugated hyperbilirubinemia, often exacerbated by stress or fasting.
- Crigler-Najjar Syndrome:
- Type I: Absent UGT1A1. Severe. Kernicterus.
- Type II (Arias): Markedly ↓ UGT1A1. Responds to phenobarbital. Less severe.
- Gilbert's Syndrome: Mild ↓ UGT1A1 activity. Intermittent jaundice (stress, fasting). Benign.
- Conjugated Hyperbilirubinemia (Inherited):
- Dubin-Johnson Syndrome: Defective MRP2 (cMOAT). Black liver. Urine: Coproporphyrin I >80%.
- Rotor Syndrome: Defective OATP1B1/B3. No black liver. Impaired storage. Urine: ↑ Copro I & III (Copro I <80%).
- 📌 Syndrome Keys: Gilbert (↓UGT), Crigler-Najjar (No/↓UGT), Dubin-Johnson (MRP2, Dark liver, ↑Copro I), Rotor (OATP, No dark liver, ↑Copro I&III).
- Neonatal Jaundice:
- Physiological: Appears after 24 hrs, peaks 3-5 days. Immature UGT.
- Pathological: Within 24 hrs; Bilirubin ↑ >5 mg/dL/day; Total >15 mg/dL (term).
- Kernicterus: Neurologic damage if unconjugated bili >20-25 mg/dL.
- Breast milk jaundice: Day 4-7 onset, prolonged. β-glucuronidase.
- Breastfeeding failure jaundice: Early, dehydration, ↓ intake.
High‑Yield Points - ⚡ Biggest Takeaways
- Bilirubin is derived from heme breakdown.
- Unconjugated bilirubin (UCB) is lipid-soluble, neurotoxic, and albumin-bound.
- Hepatic UDP-glucuronosyltransferase (UGT) conjugates UCB to water-soluble conjugated bilirubin (CB).
- Gilbert's syndrome: Mild ↑ UCB due to ↓ UGT activity; often benign.
- Crigler-Najjar syndrome: Severe ↑ UCB from UGT absence (Type I) or deficiency (Type II).
- Dubin-Johnson syndrome: ↑ CB, black liver (MRP2 defect).
- Physiological jaundice of newborn: Common, transient ↑ UCB from immature UGT.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

