Point-of-Care Testing - Speedy Spot Checks
- Definition: Medical testing performed near the patient, outside a central laboratory. Enables rapid results for timely clinical decisions.
- AKA: Near-patient testing, bedside testing, ancillary testing.
- Scope:
- Blood glucose (glucometers)
- Urine dipsticks (protein, glucose, ketones, pH, bilirubin, blood)
- Pregnancy tests (hCG)
- Hemoglobin (HbA1c, anemia screening)
- Electrolytes (Na+, K+, Cl-, Ca2+)
- Blood gases (pH, pCO2, pO2)
- Coagulation (PT/INR)
- Cardiac markers (Troponin I/T)
- Infectious diseases (HIV, malaria, influenza, COVID-19 antigen)
- Advantages:
- Rapid turnaround time (TAT)
- Reduced sample transport issues
- Smaller sample volumes
- Improved patient convenience & management
- Disadvantages:
- Higher cost per test
- Quality control challenges (operator variability)
- Limited test menu compared to central lab
- Potential for misinterpretation without lab expertise

⭐ Exam Favourite: Glucometers are the most common POCT devices, crucial for diabetes management and monitoring glycemic control. They typically use electrochemical biosensor technology based on glucose oxidase or glucose dehydrogenase enzymes for glucose measurement in whole blood (capillary or venous).
Point-of-Care Testing - Bedside Test Toolkit
- Definition: Rapid testing near patient, outside central lab. Goal: ↓ Turnaround Time (TAT), faster clinical decisions.
- Common POCT Analytes & Devices:
- Glucose: Glucometers (electrochemical). Diabetes mgmt. Target: Fasting 70-100 mg/dL, Post-prandial <140 mg/dL.
- ABG & Electrolytes: Portable analyzers (Ion-Selective Electrodes - ISE). Measures: pH, $pCO_2$, $pO_2$, $HCO_3^-$, $Na^+$, $K^+$, $Cl^-$, $Ca^{2+}$, lactate. Crucial in ICU/ER.
- Cardiac Markers: Immunoassays. Troponin I/T (Acute Coronary Syndrome - ACS, Myocardial Infarction - MI rule-out <1 hr), BNP/NT-proBNP (heart failure).
- Coagulation: Prothrombin Time/International Normalized Ratio (PT/INR) (warfarin), Activated Clotting Time (ACT) (heparin).
- Urinalysis: Dipsticks (pH, protein, glucose, ketones, bilirubin, blood, nitrites, leukocytes).
- Infectious Diseases: Rapid antigen tests (e.g., Strep A, Influenza, Malaria, Dengue, HIV).
- Hemoglobin (Hb): Portable photometers. Anemia screening.
- HbA1c: Diabetes monitoring (some POCT available).
- Ketones: Blood/urine (Diabetic Ketoacidosis - DKA). β-hydroxybutyrate preferred.
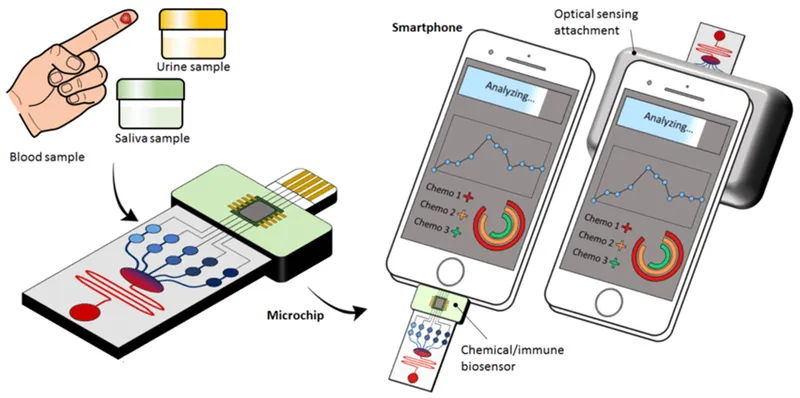
- Key Technologies:
- Electrochemical: Amperometry, potentiometry (e.g., biosensors for glucose, ISEs for electrolytes).
- Optical: Reflectance photometry (e.g., urine dipsticks), immunochromatography (lateral flow assays).
- Advantages:
- ↓ TAT (results in minutes).
- Small sample volume.
- Portability.
- Improved patient triage & management.
- Disadvantages:
- Higher cost per test vs central lab.
- Stringent Quality Control (QC) & operator training vital.
- Interferences (e.g., hematocrit, drugs, bilirubin with glucometers).
- ⚠️ Potential for pre-analytical & analytical errors if protocols not followed.
⭐ Most POCT glucose meters utilize glucose oxidase or glucose dehydrogenase enzyme-based electrochemical biosensors for glucose detection an important fact for NEET PG exam preparation focusing on clinical biochemistry applications of enzymes and biosensors technology in diagnostics
Point-of-Care Testing - Ensuring Accuracy Anywhere
- Quality Assurance (QA):
- Internal QC (IQC): Daily/batch checks; controls. Validates precision.
- External Quality Assessment (EQA): Blind samples; inter-lab comparison. Assesses accuracy.
- Calibration: Regular verification. Ensures accuracy.
- Operator Competency: Training & ongoing assessment.
- Error Hotspots & Prevention (📌 Pre > Ana > Post):
- Pre-analytical: ID, sample quality (hemolysis, clots), interferences.
- Prevention: Strict SOPs, training.
- Analytical: Instrument/reagent faults, calibration errors.
- Prevention: IQC, EQA, maintenance.
- Post-analytical: Transcription errors, critical value delays.
- Prevention: LIS, clear protocols.
- Pre-analytical: ID, sample quality (hemolysis, clots), interferences.
- Regulatory (India):
- NABL: ISO 15189, 22870 (POCT). Ensures quality.
- Documentation: SOPs, QC logs, maintenance, training (mandatory).
⭐ Glucose meters (POCT) must meet ISO 15197:2013 accuracy: 95% of results within ±15 mg/dL (for glucose <100 mg/dL) or ±15% (for glucose ≥100 mg/dL) compared to reference lab method.
High‑Yield Points - ⚡ Biggest Takeaways
- POCT delivers rapid, near-patient results, enabling swift clinical decisions.
- Key examples: Glucometers, ABG analyzers, urine dipsticks, cardiac troponin, PT/INR monitors.
- Major benefits: Drastically reduced TAT, improved patient management, decentralized testing.
- Significant drawbacks: Higher per-test cost, potential for operator error, rigorous QC essential.
- IQC and EQA are mandatory for POCT quality assurance.
- Critical in ER, ICU, OT, and resource-limited settings.
- Proper training and adherence to protocols are paramount for accuracy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

