Pancreas Powerhouse - Exocrine Essentials
- Acinar Cell Enzymes:
- Amylase: Starch digestion.
- Lipase (+ Colipase): Fat (TG) digestion.
- Proteases (inactive zymogens): Trypsinogen, Chymotrypsinogen etc.
- Enteropeptidase activates Trypsinogen → Trypsin (activates others).
- Ductal Cell Secretions:
- Bicarbonate ($HCO_3^-$): Neutralizes acid; pH ~7.8 for enzymes.
- Water.
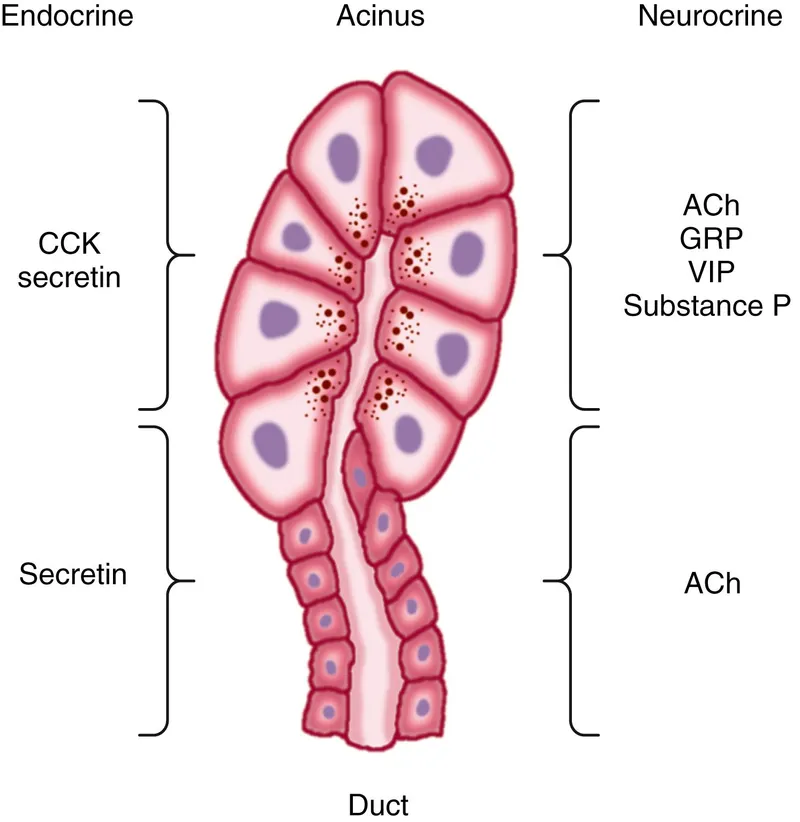
- Regulation:
- Secretin: ↑ $HCO_3^-$ (H+ stimulus).
- CCK: ↑ Enzymes (fat/protein stimulus).
- Vagus (Ach): Stimulatory.
⭐ Enteropeptidase, a duodenal brush border enzyme, is essential for initiating pancreatic proteolytic enzyme activation by converting trypsinogen to trypsin.
Digestion Dips - EPI Unmasked
- Exocrine Pancreatic Insufficiency (EPI): Impaired nutrient digestion (fats, proteins, carbs) from insufficient pancreatic enzyme secretion.
- Leading Causes:
- Chronic Pancreatitis (most common in adults; alcohol, idiopathic)
- Cystic Fibrosis (most common in children; CFTR gene mutation)
- Pancreatic duct obstruction (e.g., tumors, stones)
- Pancreatic resection/surgery (e.g., Whipple procedure)
- Key Symptoms:
- Steatorrhea (greasy, foul-smelling, bulky, floating stools)
- Unintentional weight loss, signs of malnutrition
- Abdominal pain, bloating, excessive flatus
- Symptoms of fat-soluble vitamin (A, D, E, K) deficiency
⭐ Clinically significant steatorrhea and maldigestion typically manifest only after >90% of pancreatic secretory capacity is lost, highlighting the pancreas's large functional reserve.
Lab Sleuths - Uncovering Pancreatic Function
Diagnosing exocrine pancreatic insufficiency (EPI), guiding therapy.
- Direct Tests (Highest sensitivity/specificity, Invasive):
- Secretin-Cholecystokinin (CCK) Test: Measures duodenal aspirate (volume, bicarbonate, enzymes) post-hormonal stimulation.
- Bicarbonate < 80 mEq/L strongly suggests EPI.
- Secretin-Cholecystokinin (CCK) Test: Measures duodenal aspirate (volume, bicarbonate, enzymes) post-hormonal stimulation.
- Indirect Tests (Widely used, Non-invasive):
- Fecal Elastase-1 (FE-1): Pancreas-specific enzyme.
- For moderate-severe EPI. Unaffected by PERT.
- Normal: > 200 µg/g stool.
- Mild-moderate EPI: 100-200 µg/g.
- Severe EPI: < 100 µg/g.
- Serum Trypsinogen (Immunoreactive Trypsinogen - IRT):
- ↓ levels in advanced EPI (e.g., cystic fibrosis).
- ↑ in acute pancreatitis or early chronic pancreatitis.
- Fecal Fat Assessment (Steatorrhea):
- Qualitative: Sudan III stain (rapid screen).
- Quantitative: 72-hr collection (gold standard for malabsorption); >7g fat/day abnormal.
- Fecal Elastase-1 (FE-1): Pancreas-specific enzyme.
- Breath Tests (Non-invasive, assess specific enzyme activity):
- $^{\text{13}}$C-Mixed Triglyceride Breath Test:
- Measures exhaled $^{\text{13}}$CO$_2$ after $^{\text{13}}$C-triglyceride ingestion.
- Reflects lipase activity & fat digestion.
- $^{\text{13}}$C-Mixed Triglyceride Breath Test:
⭐ Fecal Elastase-1 is a widely used indirect test for EPI due to its high specificity, sensitivity (especially for moderate to severe cases), convenience, and the fact that its measurement is not affected by concurrent pancreatic enzyme replacement therapy.
Inflammation Indicators - Acute & Chronic Alerts
- Acute Pancreatitis: Serum Amylase & Lipase key.
- Levels >3x ULN (Upper Limit of Normal) highly suggestive.
- Magnitude of ↑ not disease severity correlate.
- CRP (C-Reactive Protein) for severity assessment.
| Feature | Serum Amylase | Serum Lipase |
|---|---|---|
| Onset (Acute Pancreatitis) | 2-12 hrs | 4-8 hrs |
| Peak (Acute Pancreatitis) | ~24 hrs | ~24 hrs |
| Normalizes | 3-7 days | 8-14 days (longer window) |
| Specificity | Lower (↑ mumps, renal failure) | Higher (more pancreas-specific) |
| Sensitivity (Acute Pancreatitis) | Good | Better (esp. alcoholic pancreatitis) |
High‑Yield Points - ⚡ Biggest Takeaways
- Serum amylase and lipase diagnose acute pancreatitis; lipase is more specific with a longer half-life.
- Fecal elastase-1 is a sensitive and specific non-invasive marker for exocrine pancreatic insufficiency (EPI).
- The Secretin-CCK stimulation test remains the gold standard for assessing exocrine function, though invasive.
- Immunoreactive trypsinogen (IRT) is crucial for newborn screening of cystic fibrosis.
- Amylase isoenzymes (P-type vs S-type) differentiate pancreatic from salivary hyperamylasemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

