CSF Physiology - Brain Juice Flow
- Formation: Primarily choroid plexus (ventricles); minorly ependymal lining.
- Circulation Path:
- Lateral Ventricles → Foramen of Monro
- → 3rd Ventricle → Aqueduct of Sylvius
- → 4th Ventricle → Foramina Luschka & Magendie
- → Subarachnoid Space → Arachnoid Villi (absorption).
- Total Volume: Adults ~150 mL; Neonates ~10-60 mL.
- Key Functions: Buoyancy, protection, waste clearance, chemical stability.
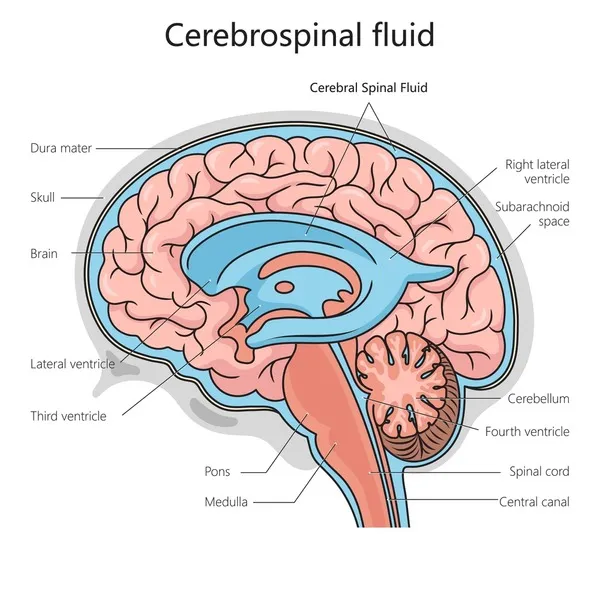
⭐ CSF is primarily produced by the choroid plexus in the ventricles at a rate of about 0.35 mL/min or 500 mL/day.
CSF Collection - Tapping the Spine
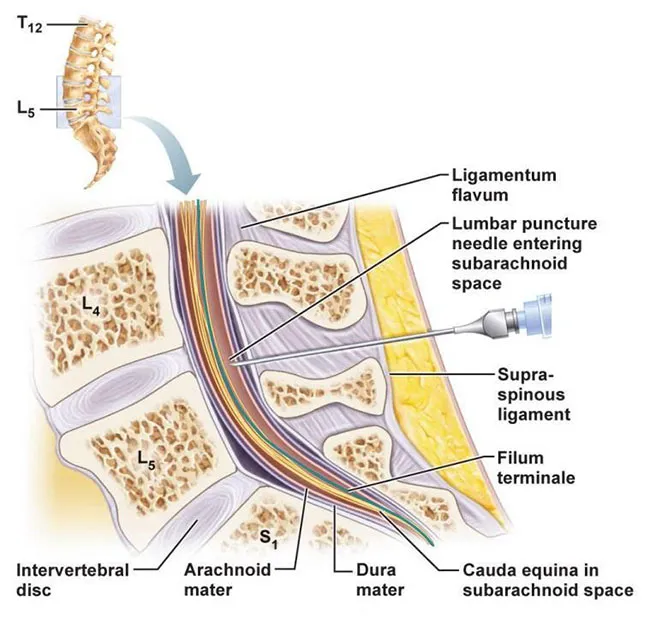
- Procedure: Lumbar Puncture (LP).
- Site (Adults): L3-L4 or L4-L5 interspace (below conus medullaris).
- Site (Infants/Children): L4-L5 or L5-S1.
- Position: Lateral decubitus (fetal position) or sitting upright, leaning forward.
- Needle: Passes skin, subcutaneous tissue, supraspinous ligament, interspinous ligament, ligamentum flavum, epidural space, dura mater, arachnoid mater into subarachnoid space.
⭐ The L3-L4 or L4-L5 interspace is the most common site for lumbar puncture in adults, passing through the ligamentum flavum with a characteristic 'pop'.
- Pressure: Opening pressure measured with manometer (70-180 mm H₂O or 5-15 mmHg).
- Collection: 3-4 sterile tubes, 1-2 mL each (Tube 1: Chemistry/Serology; Tube 2: Microbiology; Tube 3: Cell count/Cytology).
Normal CSF - Crystal Clear Code
- Appearance: Crystal clear, colorless (like water)
- Opening Pressure: 70-180 mm H₂O (or cm H₂O)
- Cells (WBC): 0-5 cells/µL (all mononuclear - lymphocytes, monocytes)
- Protein: 15-45 mg/dL
- Glucose: 50-80 mg/dL (or 2/3 of blood glucose)
- Chloride: 118-132 mEq/L
- Gram Stain & Culture: Sterile
⭐ Normal CSF glucose is approximately 60% of the plasma glucose level (typically 50-80 mg/dL), and a significantly decreased CSF/serum glucose ratio (<0.4) is a hallmark of bacterial meningitis.
📌 Mnemonic: Crystal Clear Cells 0-5, Protein 15-45, Glucose 50-80 (2/3rd of plasma).
Meningitis CSF - Infection Detectives
Key CSF changes guide diagnosis:
- Bacterial: Turbid. PMNs >1000/µL. Protein >100 mg/dL. Glucose <40 mg/dL. Gram stain +.
- Viral: Clear. Lymphocytes 10-1000/µL. Protein N/↑ (50-100 mg/dL). Glucose Normal.
- Tuberculous (TBM): Pellicle. Lymphocytes 100-500/µL. Protein ↑↑ (100-500+ mg/dL). Glucose ↓↓ (<20 mg/dL). AFB/PCR/ADA.
- Fungal: Viscous. Lymphocytes 20-500/µL. Protein ↑ (50-200 mg/dL). Glucose ↓ (<40 mg/dL). India Ink/CrAg.
⭐ In tuberculous meningitis, CSF typically shows lymphocytic pleocytosis, markedly elevated protein, very low glucose, and pellicle/cobweb formation on standing.
Other CSF Clues - Beyond Infections
- Subarachnoid Hemorrhage (SAH):
- Xanthochromia (yellowish supernatant).
- Persistently ↑RBCs (no clearing in serial tubes).
-
⭐ Xanthochromia (yellowish discoloration of CSF supernatant) due to bilirubin indicates a subarachnoid hemorrhage occurred at least 2-4 hours prior, distinguishing it from a traumatic tap.
- Multiple Sclerosis (MS):
- Oligoclonal bands (OCBs) in CSF, absent in serum.
- ↑IgG index (>0.7).
- Guillain-Barré Syndrome (GBS):
- Albuminocytologic dissociation: Markedly ↑protein, normal/mildly ↑WBCs (peaks 1-2 wks).
- Malignancy (Carcinomatous meningitis):
- Malignant cells on cytology.
- Often ↑protein, ↓glucose.
- Traumatic Tap:
- Blood clears in subsequent tubes. No xanthochromia.
High‑Yield Points - ⚡ Biggest Takeaways
- Normal CSF: Clear, colorless, pressure 70-180 mm H₂O.
- Xanthochromia (yellow CSF) indicates old hemorrhage or very high protein.
- ↑ Protein with normal cells (albuminocytologic dissociation) is classic for Guillain-Barré syndrome.
- ↓ Glucose (<40 mg/dL or <2/3rd blood glucose) suggests bacterial, tubercular, or fungal meningitis.
- Pleocytosis: Neutrophils in bacterial meningitis; lymphocytes in viral, TB, fungal meningitis.
- Oligoclonal bands (IgG) in CSF (not serum) suggest multiple sclerosis.
- India Ink for Cryptococcus; Ziehl-Neelsen for TB.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

