Lactose Intolerance - Milk Mayhem
- Lactase (β-galactosidase) deficiency → maldigestion of lactose (glucose + galactose).
- Types:
- Primary: Adult-type hypolactasia. Genetically programmed ↓ lactase. Most common. Autosomal Recessive (AR).
- Secondary: Gut mucosal injury (e.g., gastroenteritis, celiac disease, IBD).
- Congenital: Rare, AR. Neonatal onset.
- Developmental: Preterm infants (< 34 wks gestation).
- Pathophysiology: Undigested lactose → osmotic diarrhea. Colonic bacterial fermentation → gas ($H_2$, $CO_2$, $CH_4$), short-chain fatty acids → bloating, flatulence, cramps.
- Clinical Features: Dose-dependent abdominal pain, bloating, diarrhea, flatulence post-lactose ingestion.
- Diagnosis:
- Lactose Hydrogen Breath Test: ↑ $H_2$ in breath post-lactose (gold standard).
- Lactose Tolerance Test: Blood glucose ↑ < 20 mg/dL over baseline after 50g oral lactose.
- Stool pH < 5.5; reducing substances (+).
- Management: Dietary lactose restriction/avoidance. Lactase enzyme supplements. Calcium supplementation (if dairy avoided).
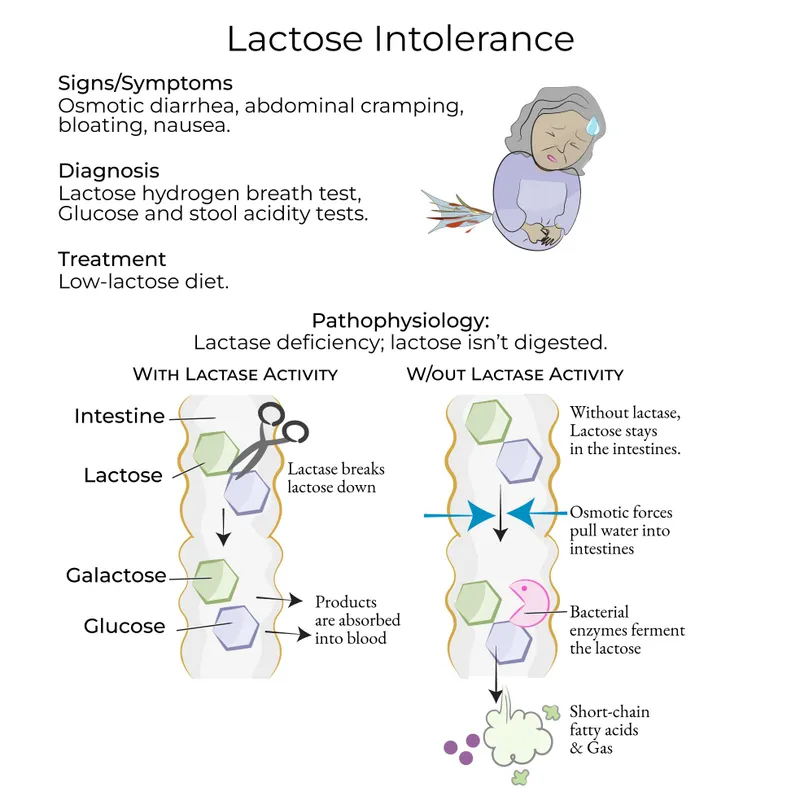
⭐ Primary lactase deficiency (adult-type hypolactasia) is the most common form, typically developing after weaning due to genetic downregulation of lactase activity_._
Galactosemia - Sweet Poison
- Autosomal recessive disorders of galactose metabolism. Galactose from lactose (milk sugar) breakdown.
- Types & Deficiencies:
- Classic (Type I): Galactose-1-Phosphate Uridyltransferase (GALT) deficiency. Most common & severe.
- Accumulation: Galactose-1-phosphate (toxic), Galactitol.
- Type II: Galactokinase (GALK) deficiency.
- Accumulation: Galactose, Galactitol (cataracts).
- Type III: UDP-Galactose-4-Epimerase (GALE) deficiency. Variable severity.
- Classic (Type I): Galactose-1-Phosphate Uridyltransferase (GALT) deficiency. Most common & severe.
- Clinical Features (Classic GALT): Onset with milk feeding.
- Jaundice, hepatomegaly, vomiting, FTT.
- Cataracts (galactitol accumulation).
- Neurological: Lethargy, hypotonia, developmental delay.
- ⭐ > Neonates with GALT deficiency are at high risk for E. coli sepsis.
- Diagnosis:
- Newborn screening (GALT activity).
- ↑ Blood galactose, ↑ RBC galactose-1-phosphate.
- Reducing substances in urine (non-glucose).
- Enzyme assays, genetic testing.
- Management: Lifelong galactose-free diet (avoid milk, dairy). Soy-based formula.
- Prognosis: Early diagnosis & treatment crucial. Long-term complications (speech, ovarian failure) can occur despite diet.

Differential Diagnosis - Milk vs. Galactose
Lactose Intolerance
- Enzyme Defect: ↓ Lactase (β-galactosidase) at intestinal brush border.
- Onset: Variable: childhood to adulthood (primary); any age (secondary to gut damage).
- Pathophysiology: Undigested lactose ferments in colon → gas (H₂, CO₂, CH₄), acidic osmotic diarrhea.
- Clinical Features: GI symptoms post-lactose: bloating, abdominal cramps, flatulence, watery/frothy diarrhea. No systemic toxicity.
- Urine Reducing Substances: Negative.
- Diagnostic Clue: Positive hydrogen breath test (↑ H₂).
- Management: Dietary lactose restriction; lactase enzyme supplements.
Galactosemia (Classic - GALT Deficiency)
- Enzyme Defect: ↓ Galactose-1-Phosphate Uridyltransferase (GALT). Autosomal recessive.
- Onset: Neonatal period (days after initiating milk feeds).
- Pathophysiology: Accumulation of Galactose-1-Phosphate (cellular toxin) & Galactitol (osmotic damage, e.g., cataracts).
- Clinical Features: Severe, systemic: Failure to thrive (FTT), jaundice, hepatomegaly, vomiting, diarrhea, infantile cataracts, lethargy, hypotonia, intellectual disability.
⭐ High risk of neonatal E. coli sepsis in GALT deficiency.
- Urine Reducing Substances: Positive (due to galactose); test before glucose oxidase.
- Diagnostic Clue: ↓ GALT activity in RBCs; detected on newborn screening.
- Management: Strict, lifelong galactose-free diet (eliminate all milk, dairy, and galactose sources).
High‑Yield Points - ⚡ Biggest Takeaways
- Lactose intolerance: Caused by lactase deficiency, leading to diarrhea and bloating post-lactose; diagnosed by hydrogen breath test.
- Classic galactosemia: Due to GALT deficiency, causing galactose-1-phosphate accumulation; presents with failure to thrive, jaundice, hepatomegaly, cataracts, E. coli sepsis.
- Galactokinase deficiency: Results in infantile cataracts from galactitol accumulation.
- Galactosemias show non-glucose reducing substances in urine.
- Management for both involves dietary restriction: lactose-free or galactose-free_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

