Glycogen Basics - Sugar Stash Central
- Storage form of glucose; readily mobilizable.
- Main Sites: Liver (maintains blood glucose) & Skeletal Muscle (energy for contraction).
- Structure: Branched polymer of $\alpha$-D-glucose units.
- Linear chains: $\alpha$-1,4 glycosidic bonds.
- Branch points: $\alpha$-1,6 glycosidic bonds (every 8-12 residues).
- Cytosolic granules.

⭐ Liver glycogen can be depleted after 12-18 hours of fasting; muscle glycogen varies with exercise.
Glycogenesis - Building the Branches
- Enzyme: Branching Enzyme (Amylo-$\alpha(1,4)\rightarrow \alpha(1,6)$-transglucosylase).
- Mechanism:
- Transfers a block of ~7 glucose units from a linear chain (donor chain $\ge$11 residues long).
- Source: Non-reducing end of an $α-1,4$ linked chain.
- Destination: Interior site on the same or another chain, forming an $α-1,6$ bond.
- New branch point: Must be $\ge$4 residues away from other existing branches. 📌 Branch: 11 to give, 4 to live.
- Result: ↑ Glycogen solubility; ↑ number of non-reducing ends for rapid glucose synthesis & breakdown.
> ⭐ Andersen Disease (Type IV Glycogen Storage Disease) results from branching enzyme deficiency. This leads to abnormal glycogen with very long outer unbranched chains, causing hepatosplenomegaly and progressive liver cirrhosis, often fatal in early childhood.
Glycogenolysis - Tapping the Tank
Breakdown of stored glycogen to glucose-1-phosphate (G1P) & free glucose. Mainly in liver & muscle.
- Key Enzymes:
- Glycogen Phosphorylase: Rate-limiting; cleaves α-1,4 bonds. Needs PLP (Vit B6). Product: G1P.
- Debranching Enzyme (bifunctional):
- 4:4 Transferase: Moves 3 glucose units from a branch.
- α-1,6-Glucosidase: Hydrolyzes α-1,6 bond, releasing free glucose.
- Regulation (Hormonal & Allosteric):
- Activators: Glucagon (liver), Epinephrine (liver/muscle), AMP (muscle), Ca²⁺ (muscle).
- Inhibitors: Insulin, ATP, G6P (muscle), Glucose (liver).
- Lysosomal Degradation: Acid α-glucosidase (acid maltase). Deficiency → Pompe Disease (GSD II).

⭐ McArdle disease (GSD V), muscle glycogen phosphorylase deficiency, causes exercise intolerance & painful cramps.
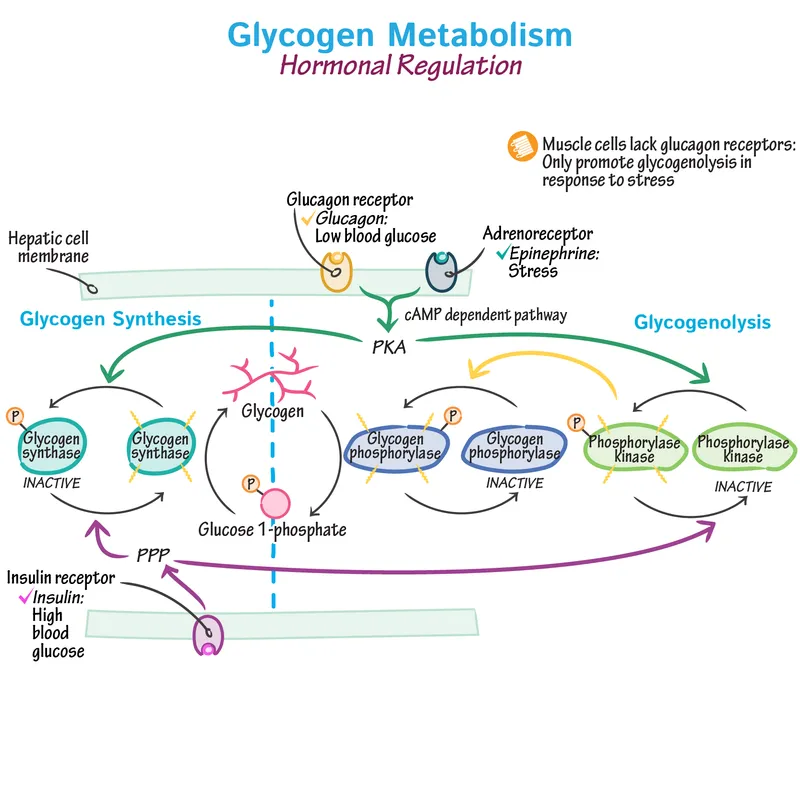
Regulation - The Control Panel
Coordinated control of Glycogen Synthase (GS) & Glycogen Phosphorylase (GP) prevents futile cycling.
- Covalent Modification (Primary):
- Dephosphorylation (Insulin, PP1): Activates GS, Inactivates GP → ↑ Glycogen Synthesis.
- Phosphorylation (Glucagon, Epinephrine via PKA): Inactivates GS, Activates GP → ↑ Glycogen Breakdown.
- Allosteric Modifiers:
- GS: Activated by G6P (signals glucose abundance).
- GP (Muscle): Activated by AMP (low energy), Ca²⁺ (contraction); Inhibited by ATP, G6P.
- GP (Liver): Inhibited by Glucose (signals glucose abundance).
⭐ Insulin promotes glycogen synthesis by activating Protein Phosphatase-1 (PP1), which dephosphorylates (activates) glycogen synthase and dephosphorylates (inactivates) glycogen phosphorylase.
GSDs - Storage Sicknesses
- Mostly Autosomal Recessive.
- Type I (Von Gierke): G6Pase def. Hepatomegaly, fasting hypoglycemia, lactic acidosis.
- Type II (Pompe): Acid maltase def. Cardiomegaly, muscle weakness. 📌 Pompe affects Pump.
- Type III (Cori): Debranching enzyme def. Milder Type I, muscle weakness.
- Type V (McArdle): Muscle phosphorylase def. Exercise intolerance, cramps. 📌 McArdle affects Muscle.
⭐ Type I (Von Gierke): Severe fasting hypoglycemia, lactic acidosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Glycogen synthesis: Glycogen synthase (rate-limiting), uses UDP-glucose; branching enzyme (α-1,6 bonds).
- Glycogenolysis: Glycogen phosphorylase (rate-limiting); debranching enzyme (removes branches), yields glucose-1-P.
- Regulation: Insulin ↑synthesis; glucagon (liver) & epinephrine (muscle/liver) ↑breakdown.
- Liver glycogen maintains blood glucose; muscle glycogen for local energy (lacks G6Pase).
- Von Gierke's (Type I): G6Pase deficiency; severe fasting hypoglycemia.
- McArdle's (Type V): Muscle glycogen phosphorylase deficiency; exercise intolerance, cramps.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

