One-Carbon Units - Tiny Transfer Titans
- Definition: One-carbon (1C) units are single carbon atoms or groups (e.g., methyl, methylene) transferred in metabolic reactions. They are vital for biosynthesis.
- Common 1C Units: Methyl ($-CH_3$), Methylene ($-CH_2-$), Methenyl ($-CH=$), Formyl ($-CHO$), Formimino ($-CH=NH$).
- Key Sources:
- Serine (major contributor)
- Glycine
- Histidine
- Tryptophan
- Formate
- Metabolic Importance: Essential for synthesizing:
- Purine nucleotides (adenine, guanine)
- Thymidylate (dTMP), a DNA precursor
- Methionine (regeneration from homocysteine)
⭐ Serine is the major source of one-carbon units, particularly donating to THF.
oka
Folate's Forms - Carbon Carrier Crew
Folic acid (pteroylglutamic acid) is converted to active Tetrahydrofolate (THF) by Dihydrofolate Reductase (DHFR), requiring 2 NADPH for the overall conversion.
- Reaction: Folic Acid $\xrightarrow{DHFR}$ DHF $\xrightarrow{DHFR}$ THF.
- DHFR inhibitors: Methotrexate (anticancer), Trimethoprim (antibiotic).
THF carries various one-carbon (C1) units (e.g., $-CH_3$, $-CH_2-$, $-CHO$) attached to N5, N10, or both. These interconvertible forms constitute the 'folate pool'.
- N5-Methyl-THF: Most reduced. For methionine synthesis.
- N5,N10-Methylene-THF: For dTMP synthesis, serine $\leftrightarrow$ glycine.
- N5,N10-Methenyl-THF: Intermediate in C1 interconversions.
- N10-Formyl-THF: For purine synthesis (C2, C8 atoms).
- N5-Formimino-THF: From histidine catabolism.
- 📌 Key forms: Methyl, Methylene, Methenyl, Formyl.

⭐ N5,N10-methylene THF is crucial for dTMP synthesis (from dUMP by thymidylate synthase), a key target for cancer chemotherapy (e.g., 5-Fluorouracil).
SAM's Story - Methyl Mastermind
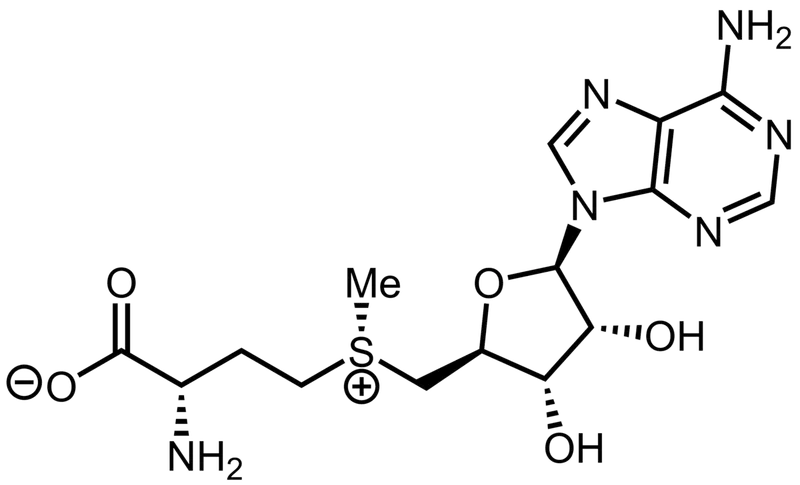 cycle and methyl donation pathways)
cycle and methyl donation pathways)
- S-Adenosylmethionine (SAM): Primary methyl ($CH_3$) donor; "activated methionine." Essential for metabolic pathways.
- Synthesis:
- From L-Methionine and ATP.
- Methionine + ATP $\xrightarrow{\text{Methionine Adenosyltransferase (MAT)}}$ SAM + $PP_i + P_i$.
- 📌 Methionine Always Transfers to SAM (MAT).
- Role - The Methyl Mastermind (Activated Methyl Cycle):
- Principal methyl donor for transmethylation, crucial for:
- DNA/RNA Methylation: Gene expression, chromatin.
- Neurotransmitter Synthesis: E.g., Norepinephrine $\rightarrow$ Epinephrine.
- Creatine Synthesis: Muscle energy storage.
- Melatonin Synthesis: Sleep cycle hormone.
- Phosphatidylcholine Synthesis: Membrane lipid.
- Principal methyl donor for transmethylation, crucial for:
- Fate after Methyl Donation:
- SAM (-$CH_3$) $\rightarrow$ S-Adenosylhomocysteine (SAH), an inhibitor of methyltransferases.
- SAH + $H_2O \xrightarrow{\text{SAH Hydrolase}}$ L-Homocysteine + Adenosine.
- Regeneration of Methionine from Homocysteine: Sustains SAM levels.
⭐ SAM is the universal methyl donor for many biological methylations, impacting biomolecule synthesis and epigenetic regulation.
Clinical Capsules - Transfer Turmoil
- Folate Deficiency:
- Causes: Poor diet, malabsorption, drugs (methotrexate, phenytoin).
- Manifestations: Megaloblastic anemia, neural tube defects.
- Vitamin B12 Deficiency:
- Causes: Pernicious anemia, vegan diet, malabsorption.
- Manifestations: Megaloblastic anemia, neurological deficits (methionine synthase ↓, methylmalonyl CoA mutase ↓ → MMA ↑).
⭐ The 'methyl-folate trap' in Vitamin B12 deficiency causes functional folate deficiency; THF is trapped as N5-methyl-THF despite normal folate.
- Hyperhomocysteinemia:
- Causes: Genetic (CBS, MTHFR defects), nutritional (↓B6, B12, folate).
- Significance: ↑ Cardiovascular disease risk.
- Key Drugs:
- Methotrexate, Trimethoprim: Inhibit DHFR.
- 5-Fluorouracil: Inhibits thymidylate synthase_
High‑Yield Points - ⚡ Biggest Takeaways
- Tetrahydrofolate (THF) is the primary carrier of one-carbon units like formyl, methenyl, methylene, methyl.
- S-Adenosylmethionine (SAM) is the major methyl group donor in numerous biological reactions.
- Vitamin B12 is essential for methionine synthase (homocysteine to methionine) and methylmalonyl-CoA mutase.
- Folate deficiency leads to megaloblastic anemia and increases risk of neural tube defects.
- Vitamin B12 deficiency causes a "folate trap", leading to functional folate deficiency.
- Dihydrofolate reductase (DHFR), targeted by methotrexate, regenerates THF an essential step in folate metabolism.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

