Mask Ventilation Basics - Seal the Deal
- Purpose: Provide temporary oxygenation & ventilation non-invasively; bridge to advanced airway.
- Indications: Apnea, respiratory insufficiency, pre-oxygenation before intubation, procedural sedation.
- Technique - The Seal:
- Mask Size: Covers mouth & nose; bridge of nose to just above chin (avoiding eye compression).
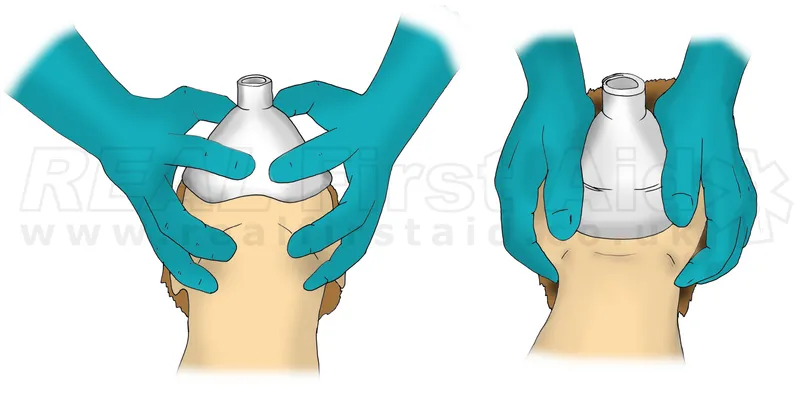
- Grip (📌 E-C Clamp):
- 'C'-shape: Thumb & index finger press mask firmly onto face.
- 'E'-shape: Remaining 3 fingers lift mandible (jaw thrust), extending atlanto-occipital joint.
- Two-person technique often superior, especially for difficult seals (e.g., beards, edentulous).
- Goals: Visible chest rise, $SpO_2$ > 90%, presence of end-tidal $CO_2$ (ETCO2).
- Common Problems: Inadequate seal (air leak), airway obstruction (tongue, soft tissues), insufficient tidal volume.
⭐ Inability to maintain oxygen saturation > 90% using a face mask or failure to prevent/reverse signs of inadequate ventilation despite optimal attempts constitutes failed mask ventilation (a component of a difficult airway).
Gear Up - Tools of Trade
- Face Masks:
- Transparent, anatomical; sizes 0-6. Cushioned rim.
- Fit: Nasal bridge to mentum; airtight seal.
- Connector: 22mm female.

- Oropharyngeal Airways (OPA):
- Types: Guedel, Berman. Color-coded.
- Action: Lifts tongue off posterior pharynx.
- Size: Mouth corner to mandible angle.
- 📌 Guedel: Good airway.
- Nasopharyngeal Airways (NPA):
- Use: Conscious pt; OPA difficult/trismus.
- Size: Nares to tragus. Lubricate. Bevel to septum.
- ⚠️ Avoid: Basal skull fracture, coagulopathy.
- Self-Inflating Bag (Ambu):
- Positive pressure ventilation. Non-rebreathing valve.
- FiO2: ~21% (air); up to 100% (O2 + reservoir).
⭐ OPA sizing: Critical. Too large: obstructs larynx/trauma. Too small: ineffective.
Mastering the Mask - Grip & Tricks
- Goal: Effective seal & patent airway for BMV.
- Grips:
-
One-Hand (C-E): Thumb/index ('C') on mask; 3 fingers ('E') lift jaw.
-
Two-Hand (V-E/Thenar Eminence): Both hands on mask, strong jaw thrust. Needs assistant. Best for DMV.
-
- Key Maneuvers & Adjuncts:
- Head-tilt/chin-lift (if no C-spine injury).
- Jaw thrust: Lifts tongue, opens airway.
⭐ Jaw thrust is crucial to relieve upper airway obstruction during mask ventilation.
- OPA/NPA airways: Bypass soft tissue obstruction.
- Troubleshooting & Improving Ventilation:
- Reposition. Optimize jaw thrust.
- Use two-person technique.
- Avoid high pressure (gastric insufflation > 20 cm H₂O).
- DMV Predictors (📌 MOANS):
- Mask Seal (beard, NGT, anomaly)
- Obesity (BMI > 30)/Obstruction (OSA)
- Age (> 55 yrs)
- No Teeth (edentulous)
- Stiff Lungs (asthma)/Sleep Apnea
DMV SOS - Spotting Trouble
Difficult Mask Ventilation (DMV) is inadequate alveolar oxygenation using a face mask. Early identification of risk factors is crucial.
📌 BONES Mnemonic for DMV Predictors:
- Beard: Impedes mask seal.
- Obesity: BMI > 30 kg/m².
- No teeth (Edentulous): Poor mask fit.
- Elderly: Age > 55 years (loss of tissue elasticity).
- Snoring/OSA/Stiff Lungs: Indicates potential obstruction or ↑ resistance.
If DMV is suspected or encountered:
⭐ The inability to maintain SpO₂ > 92% with 100% O₂ and optimal technique defines DMV.
High‑Yield Points - ⚡ Biggest Takeaways
- C-E grip is crucial for an effective mask seal.
- Use MOANS mnemonic to predict Difficult Mask Ventilation (DMV).
- Two-person mask ventilation often overcomes DMV challenges.
- OPA/NPA adjuncts help maintain airway patency during mask ventilation.
- Ramping position optimizes airway alignment in obese patients.
- Limit peak inspiratory pressures to <20 cmH2O to prevent gastric insufflation.
- Thorough pre-oxygenation (denitrogenation) is vital before mask ventilation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

