Truncal Blocks Fundamentals - Core Canvas
- Definition: Regional anesthesia techniques targeting nerves supplying the chest and abdominal wall.
- Goals: Provide analgesia/anesthesia for thoracic and abdominal surgeries, reduce opioid consumption, facilitate early mobilization.
- Advantages: Opioid-sparing, improved respiratory function, reduced PONV, enhanced recovery.
- Relevant Anatomy:
- Innervation:
- Thoracic wall: Intercostal nerves (T1-T11).
- Abdominal wall: Lower intercostal (T7-T11), Subcostal (T12), Ilioinguinal & Iliohypogastric (L1) nerves.
- Key Fascial Planes:
- Transversus Abdominis Plane (TAP)
- Rectus Sheath
- Erector Spinae Plane (ESP)
- Pecs I & II planes
- Serratus Anterior Plane (SAP)
- Innervation:
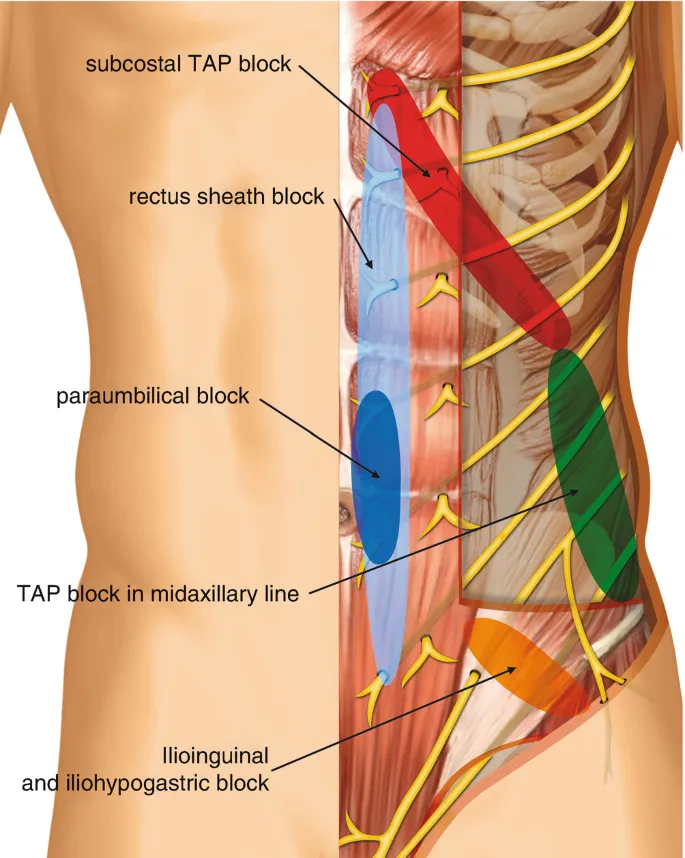
⭐ The concept of 'fascial plane blocks,' where local anesthetic is injected between fascial layers to reach multiple nerves, has revolutionized truncal anesthesia, offering safer and more effective pain management strategies compared to epidural analgesia for many procedures.
Thoracic Wall Blocks - Chest Shielders
Key thoracic wall blocks for chest analgesia.
Comparison of Thoracic Wall Blocks:
| Block | Nerves/Plane | Indications | Sono Cue | LA Vol. |
|---|---|---|---|---|
| PVB | Spinal n. (paravertebral space) | Thoracotomy, mastectomy, rib # | TP, pleura | 15-20 mL |
| ICNB | Intercostal n. (subcostal) | Rib #, neuralgia | Rib, pleura, VAN | 3-5 mL/lvl |
| Pecs I | Pectoral n. (Pmaj/Pmin plane) | Implants, pacemakers | P. major/minor | 10 mL |
| Pecs II | Pecs I + Lat. pect., intercostobrachial (Pmin/SA plane) | Mastectomy, axillary sx | P. minor, SA | 20 mL |
| SAPB | Lat. cut. intercostals (T2-T9) (Superficial/Deep to SA) | Mastectomy, thoracotomy, rib # | 📌 'Serratus Sandwich' | 20-30 mL |

⭐ SAPB often spares long thoracic nerve, preserving serratus anterior function (no winged scapula).
Abdominal Wall Blocks - Belly Blockade
📌 'TAPestry of Nerves' for TAP block coverage (T6-L1).
| Block | Target (Nerves/Plane) | Indications | Sono Cue | LA Vol/Side |
|---|---|---|---|---|
| TAP (Lat) | T6-L1 (IO/TA plane) | Laparotomy, C-section, hernia | "Double fascia" | 15-20 mL |
| RSB | T9-T11 (Post. Rectus Sheath) | Midline incision, umbilical hernia | Lens-shape post. rectus | 10-15 mL |
| II/IHNB | II/IH N. (IO/TA plane, medial ASIS) | Inguinal hernia, orchidopexy | Nerves IO/TA | 5-10 mL |
| QLB (Post) | T4-L1 (Post. to QL) | Hip, abd. wall, visceral pain | LA post. QL | 20-30 mL |

⭐ Posterior QLB often provides some visceral analgesia unlike TAP blocks.
Technique, LAs & Complications - SafeGuard Systems
- Technique: USG essential for accuracy & safety. Strict asepsis, needle visualization (in-plane/out-of-plane), hydrodissection.
- LAs (Varying Onset/Duration/Toxicity):
- Bupivacaine $0.25-0.5%$; Ropivacaine $0.2-0.5%$ (long-acting).
- Lidocaine $1-2%$ (w/ epinephrine, intermediate-acting).
- Complications:
- LAST: 📌 CNS (agitation, seizures) then CVS distress (arrhythmias, arrest). Mgmt: Stop LA, ABCs.
- Intralipid $20%$: 1.5 mL/kg bolus (1 min), then 0.25 mL/kg/min infusion. Repeat bolus if needed. 
- Others: Pneumothorax, nerve injury, hematoma, infection, block failure.
- LAST: 📌 CNS (agitation, seizures) then CVS distress (arrhythmias, arrest). Mgmt: Stop LA, ABCs.
- Contraindications: Patient refusal, active site infection, true LA allergy, severe coagulopathy.
⭐ The use of Intralipid for LAST is a Class I recommendation by ASRA. 
High‑Yield Points - ⚡ Biggest Takeaways
- TAP block (Transversus Abdominis Plane) targets T6-L1 nerves for somatic abdominal pain relief post-surgery.
- Rectus Sheath Block is ideal for midline abdominal incisions and umbilical hernia repair.
- Ilioinguinal/Iliohypogastric blocks are standard for inguinal hernia repair analgesia.
- Paravertebral Blocks (PVB) provide unilateral, segmental somatic and sympathetic blockade for thoracic/abdominal procedures.
- Erector Spinae Plane (ESP) block offers multi-dermatomal analgesia; a simpler alternative to PVB.
- Quadratus Lumborum (QL) block provides visceral and somatic analgesia for abdominal and hip surgery.
- Key risks include Local Anesthetic Systemic Toxicity (LAST) and pneumothorax (especially with PVB).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

