Physiology & RA Choices - Bump & Block Basics
- Physiological Changes (Pregnancy & RA):
- CV: ↑CO, ↓SVR. Aortocaval compression (LUD vital!).
- Resp: ↓FRC, ↑O₂ demand (rapid desaturation risk).
- GI: ↓Gastric emptying, ↓LES tone (↑aspiration risk).
- Nervous: ↑LA sensitivity (↓dose ~30%); engorged epidural veins (↓epidural volume).
- RA Advantages (Obstetrics):
- Maternal: Superior analgesia, awake patient, ↓aspiration, ↓opioids.
- Fetal: Minimal drug transfer, better uteroplacental perfusion (normotension).
- Indications: Labor analgesia (epidural, CSE); C-section (spinal, epidural, CSE).
- Contraindications (Absolute): 📌 I CHOP: Infection (site), Coagulopathy (Plt < 80,000/µL)/Severe Hypovolemia, ↑ICP, Patient refusal.
- Techniques & Levels:
- Epidural: Slower, titratable. Labor: T10-L1. C-section: T4.
- Spinal: Rapid, dense. C-section: T4.
- CSE: Spinal speed + epidural flexibility.
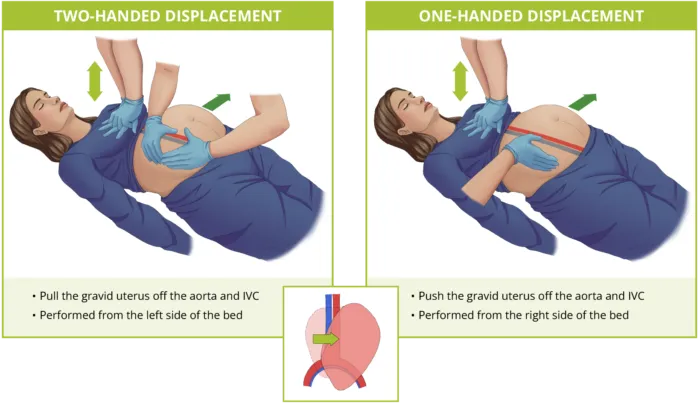
⭐ Aortocaval compression by the gravid uterus causes supine hypotension syndrome; left uterine displacement (LUD) is crucial.
Pharmacology of RA - Mommy's Magic Mix
Local Anesthetics (LAs):
- Bupivacaine: Potent, long-acting; racemic ↑cardiotoxicity.
- Levobupivacaine: S-enantiomer of bupivacaine, ↓cardiotoxicity.
- Ropivacaine: ↓cardiotoxicity & ↓motor block vs Bupivacaine.
- Lidocaine: Fast onset, short duration; for surgical epidurals.
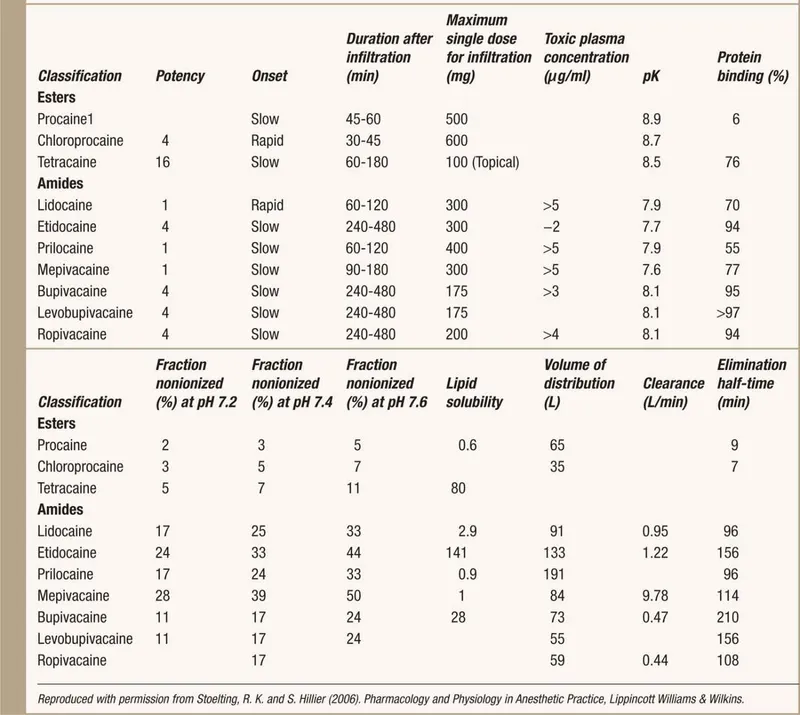
- Properties: pKa (onset), Lipid Sol. (potency/duration), Protein Bind. (duration).
- Differential Block: Sensory > Motor.
- Cardiac Toxicity: Bupivacaine > Ropivacaine/Levobupivacaine.
- Placental Transfer & Ion Trapping: LAs cross placenta; fetal acidosis → LA accumulation in fetus.
⭐ Levobupivacaine and Ropivacaine have a better safety profile (less cardiotoxic) than racemic Bupivacaine.
Neuraxial Opioids:
- Lipophilic (fast onset, short duration): Fentanyl (Epidural 50-100 mcg, IT 10-25 mcg), Sufentanil (Epidural 5-20 mcg, IT 1-5 mcg).
- Hydrophilic (slow onset, long duration): Morphine (IT 50-150 mcg).
- Benefits: Synergy with LAs (↓LA dose).
- Side Effects: 📌 Pruritus (common), N/V, Resp. Depression (early-lipo, delayed-hydro).
Adjuvants:
- Epinephrine: Test dose marker (15 mcg), prolongs block (e.g., 1:200,000 / 5 mcg/mL).
- Clonidine ($\alpha_2$-agonist): Prolongs analgesia (Epidural 75-150 mcg).
Patient-Controlled Epidural Analgesia (PCEA):
- Concept: Patient-controlled epidural boluses for labor.
- Advantages: ↑Maternal satisfaction, ↓motor block, ↓total drug.
- Typical Mix: Bupivacaine 0.0625%-0.125% + Fentanyl 1-2 mcg/mL.
Complications & Special Cases - Wobbly Walk & Woes
-
Maternal Hypotension: Common. Prevent: LUD, IV fluid co-load. Manage: Phenylephrine 50-100 mcg IV.
-
PDPH (Post-Dural Puncture Headache): Postural headache. Prevent: Atraumatic needles. Manage: Conservative; EBP (15-20 mL blood).
-
High/Total Spinal: Rapid ↑ block, respiratory distress, ↓BP. Manage: ABCs, intubate if needed.
-
LAST (Local Anesthetic Systemic Toxicity): 📌 SAMS (Slurred speech, Agitation, Metallic taste, Seizures). Manage: Stop LA, ACLS, Intralipid 20% (1.5 mL/kg bolus, 0.25 mL/kg/min infusion).
⭐ For LAST management, lipid emulsion therapy (Intralipid 20%) should be initiated early along with standard ACLS protocols, avoiding vasopressin, CCBs, beta-blockers or lidocaine for arrhythmias.

-
Neuro Complications: Rare. Nerve injury, epidural hematoma/abscess (urgent MRI).
-
Failed Block: Troubleshoot: reposition, supplemental LA, convert to GA.
-
Special Cases:
- Preeclampsia: Platelets >80,000/µL for neuraxial.
- Cardiac disease: Careful titration.
- Coagulopathy: Contraindication if significant for neuraxial anesthesia.
High‑Yield Points - ⚡ Biggest Takeaways
- Epidural analgesia is the gold standard for labor pain relief.
- Spinal anesthesia is preferred for elective Cesarean sections due to rapid onset and dense block.
- Combined Spinal-Epidural (CSE) offers rapid onset of spinal with prolonged analgesia via epidural catheter.
- Hypotension is the most common side effect of neuraxial anesthesia; manage with IV fluids and vasopressors.
- Bupivacaine is commonly used; ropivacaine and levobupivacaine offer ↑ cardiac safety.
- PDPH is a key complication; manage conservatively, then epidural blood patch.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

