Upper Limb Blocks - Nerve Navigator Intro
- Regional anesthesia for upper extremity surgery and pain management.
- Indications: Procedures on shoulder, arm, forearm, hand.
- Techniques: Single-shot or continuous catheter.
- Benefits: Opioid-sparing, ↓PONV, improved recovery.
- Risks: Nerve injury, LAST, hematoma, infection. ⚠️ Pneumothorax (supraclavicular).
- Ultrasound guidance standard for precision and safety.
⭐ Supraclavicular block: "Spinal of the arm" for comprehensive brachial plexus blockade.
Brachial Plexus - Anatomy Highway
- Roots (C5, C6, C7, C8, T1): Between Anterior & Middle Scalenes.
- Trunks (Superior, Middle, Inferior): Posterior triangle of neck, above clavicle.
- Divisions (Anterior/Posterior each): Deep to clavicle, enter axilla.
- Cords (Lateral, Posterior, Medial): Axilla; named by relation to axillary artery.
- Branches (Terminal & Collateral): Innervate the upper limb.
📌 Mnemonic: Randy Travis Drinks Cold Beer.
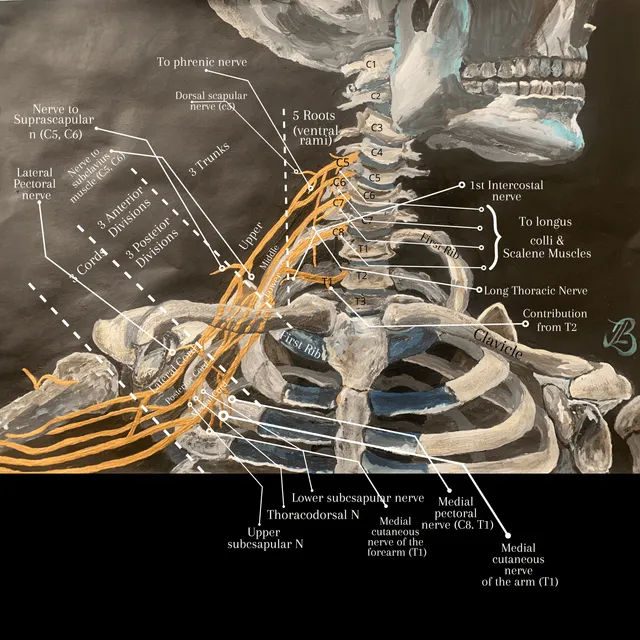
⭐ Upper Trunk (C5,C6) injury results in Erb's Palsy (waiter's tip deformity).
Above the Clavicle - High & Mighty Blocks
- Interscalene Block (ISB):
- Targets: Roots/Trunks (C5-C7).
- Landmark: Interscalene groove.
- Use: Shoulder, clavicle, proximal humerus. 📌 InterScalene for Shoulder.
- ⚠️ High phrenic nerve palsy risk; ulnar sparing.
- Supraclavicular Block (SCB):
- Targets: Trunks/Divisions. 📌 Spinal of the arm.
- Landmark: Above clavicle midpoint.
- Use: Arm, forearm, hand (below shoulder).
- ⚠️ Highest pneumothorax risk; phrenic palsy (~50%).

⭐ Phrenic nerve palsy (nearly 100%) is an expected side effect of Interscalene block due to nerve proximity at this level of the brachial plexus.
Below Clavicle & Axilla - Lowdown & Localized
-
Infraclavicular Block
- Targets: Cords (Lateral, Posterior, Medial).
- Approach: Inferior to clavicle, medial to coracoid.
- Covers: Arm, elbow, forearm, hand. Phrenic sparing.
- Catheter: Good stability.
- USG: Cords around axillary artery.
-
Axillary Block
- Targets: Branches (Median, Ulnar, Radial, Musculocutaneous).
- Approach: Axilla, around axillary artery.
- Covers: Forearm, hand.
- ⚠️ Musculocutaneous nerve (MCN) often requires separate block in coracobrachialis.
- USG: Nerves around axillary artery ("honeycomb").

⭐ Axillary block is a common choice for distal upper limb surgery, especially if avoiding phrenic nerve palsy is critical.
Distal Delights - Forearm & Wrist Wizards

- Elbow:
- Median N: Medial to brachial artery.
- Ulnar N: Ulnar groove.
- Radial N: Lateral to biceps tendon.
- Wrist: (Hand/finger anesthesia)
- Median N: B/w Palmaris Longus & FCR.
- Ulnar N: Lat. to FCU, Med. to ulnar artery.
- Sup. Radial N: Anatomical snuffbox.
⭐ Wrist blocks: Ideal for carpal tunnel release, trigger finger; spares forearm motor function.
Tech & Tox - Tools & Troubleshooters
- Tools:
- Ultrasound (USG): Preferred for ↑success, ↓complications. In-plane/out-of-plane views.
- Nerve Stimulator: Motor response at <0.5 mA (e.g., 0.2-0.4 mA). Echogenic needles.
- Local Anesthetics (LAs): Lignocaine, Bupivacaine.
- Adjuvants: Epinephrine (↑duration), Dexamethasone.
- Troubleshooters (Tox):
- LAST (Local Anesthetic Systemic Toxicity): CNS (tinnitus, seizures), CVS (arrhythmias, arrest).
⭐ Lipid Emulsion 20%: Bolus 1.5 mL/kg, then 0.25 mL/kg/min infusion.
- Nerve injury, Hematoma, Infection.
- ⚠️ Pneumothorax (esp. Supraclavicular block).
- LAST (Local Anesthetic Systemic Toxicity): CNS (tinnitus, seizures), CVS (arrhythmias, arrest).

High‑Yield Points - ⚡ Biggest Takeaways
- Interscalene block: High incidence of phrenic nerve palsy; ideal for shoulder surgery.
- Supraclavicular block: "Spinal of the arm"; highest pneumothorax risk; covers arm, elbow, forearm, hand.
- Infraclavicular block: Spares phrenic nerve; good for distal arm/hand surgery; stable for catheters.
- Axillary block: Safest from pneumothorax; best for forearm/hand; musculocutaneous nerve often needs separate block.
- Bier's block (IVRA): Uses double tourniquet; risk of LAST with tourniquet failure; for short procedures.
- Ultrasound guidance is standard for ↑success and ↓complications like nerve injury or LAST (Local Anesthetic Systemic Toxicity).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

