Overview & Classification - The Initial Rundown
Complications are classified by:
- Scope of Effect:
- Systemic: Affecting entire body (e.g., LAST, high spinal).
- Local: At injection site (e.g., nerve injury, hematoma).
- Timing of Onset:
- Immediate: During or soon after block.
- Delayed: Hours to weeks later.
Common risk factors (📌 PPA):
- Patient: Coagulopathy, pre-existing neuropathy, systemic illness.
- Procedure: Technique, multiple attempts, needle type.
- Anesthetic: Drug choice, total dose, vasoconstrictors.
⭐ Most complications are preventable with meticulous technique and careful patient selection.
Local Anesthetic Systemic Toxicity (LAST) - When LAs Go Rogue
- Definition: Systemic adverse reaction due to high blood concentrations of local anesthetic.
- Pathophysiology: Dose-dependent Na+ channel blockade in CNS & cardiovascular system (CVS).
- Susceptible LAs: Bupivacaine > Ropivacaine > Lidocaine (potency & cardiotoxicity).
- CNS Symptoms:
- Early: Tinnitus, metallic taste, perioral numbness, dizziness, visual disturbances, muscle twitching, agitation.
- Late: Seizures, unconsciousness, coma, respiratory arrest.
- 📌 Mnemonic for CNS signs (LAST): Lips numb/tingling, Agitation/Auditory changes, Seizures/Slurred speech, Twitching.
- CVS Symptoms: Initial hypertension/tachycardia → bradycardia, hypotension, ventricular arrhythmias (VT/VF), asystole, cardiac arrest.
- Risk Factors:
- High dose or rapid injection.
- Site of injection (vascularity): IV > Tracheal > Intercostal > Caudal > Epidural > Brachial plexus > Sciatic/Femoral > Subcutaneous.
- Patient factors: Extremes of age, pregnancy, cardiac/hepatic/renal dysfunction, low protein.
- Prevention:
- Use lowest effective dose.
- Aspirate before & during injection.
- Incremental injection (3-5 mL, wait 15-30s).
- Ultrasound guidance.
- Test dose for epidurals.
- Adhere to maximum recommended doses (e.g., Bupivacaine ~2 mg/kg).
- Management:
- STOP LA injection immediately.
- Call for help (get LAST kit).
- ABCs: Maintain Airway (100% O2), ensure adequate Breathing (ventilate if needed), support Circulation.
- Seizure control: Benzodiazepines (e.g., Midazolam 0.05-0.1 mg/kg IV). Avoid large doses of propofol if CVS unstable.
- Lipid Emulsion Therapy (Intralipid 20%): Administer at first sign of severe LAST (arrhythmias, refractory seizures, rapid progression).
- Bolus: 1.5 mL/kg (lean body mass) over 1 minute.
- May repeat bolus 1-2 times for persistent CVS instability.
- Infusion: 0.25 mL/kg/min.
- Continue infusion for at least 10 minutes after hemodynamic stability.
- Maximum total dose: approx. 10-12 mL/kg in the first 30 minutes.
⭐ Lipid emulsion therapy (Intralipid 20%) is a critical and specific antidote for severe Local Anesthetic Systemic Toxicity (LAST).
Neurological Complications (PDPH, Nerve Injury, CES, TNS) - Brain & Nerve Blues
-
Post-Dural Puncture Headache (PDPH)
- Patho: CSF leak → ↓ICP.
- Symptoms: Postural headache (↑upright), neck stiffness, nausea, photophobia, tinnitus.
- Risk Factors: 📌 NEEDLE: Needle (large/cutting Quincke 22G > pencil-point Whitacre 27G), Experience↓, Earlier PDPH, Dural punctures (multiple), Low CSF (young, female, pregnancy).
- Prevention: Small (25-27G), pencil-point (Whitacre, Sprotte); bevel parallel dural fibers.
- Treatment: Conservative (hydration, analgesics, caffeine); Epidural Blood Patch (EBP).
⭐ Pencil-point needles (Whitacre, Sprotte) ↓ PDPH vs. cutting (Quincke).

-
Direct Nerve Injury
- Mechanism: Needle trauma, intraneural injection, LA neurotoxicity.
- Symptoms: Persistent paresthesia, motor/sensory deficit.
- Prevention: Ultrasound, nerve stimulator; avoid injection on paresthesia/high pressure.
-
Cauda Equina Syndrome (CES) ⚠️
- Symptoms: 📌 SADDLE: Saddle anesthesia, Anal tone↓, Dysfunction (bowel/bladder), Lower limb weakness, Emergency.
- Causes: High LA conc., maldistribution, hematoma. (Old: microcatheters).
-
Transient Neurological Symptoms (TNS)
- Symptoms: Buttock/lower limb pain/dysaesthesia post-spinal.
- LA: Lidocaine. Self-limiting.
Hematoma, Infection & Catheter Issues - Site-Specific Setbacks
- Spinal/Epidural Hematoma: Neurological emergency!
- Risks: Coagulopathy, anticoagulants (check specific timing guidelines!), traumatic tap, indwelling catheter.
- Symptoms: 📌 PAIN (Progressive deficit, Acute onset, Incontinence, Numbness), severe back/radicular pain, progressive motor/sensory deficits, bowel/bladder dysfunction.
- Dx: Urgent MRI.
- Rx: Neurosurgical consultation for decompressive laminectomy within 8-12 hours.
- Infection (Epidural Abscess, Meningitis):
- Risks: Poor asepsis, immunocompromise, prolonged catheterization.
- Sx: Fever, localized back pain/tenderness, erythema, neuro deficits.
- Dx: MRI, CSF analysis. Rx: Antibiotics, surgical drainage (if abscess).
- Catheter Issues: Breakage, knotting, migration, occlusion, shearing.
- Allergic Reactions: Rare with amides; esters (PABA metabolite) more common.
- Backache: Common, usually musculoskeletal, transient.
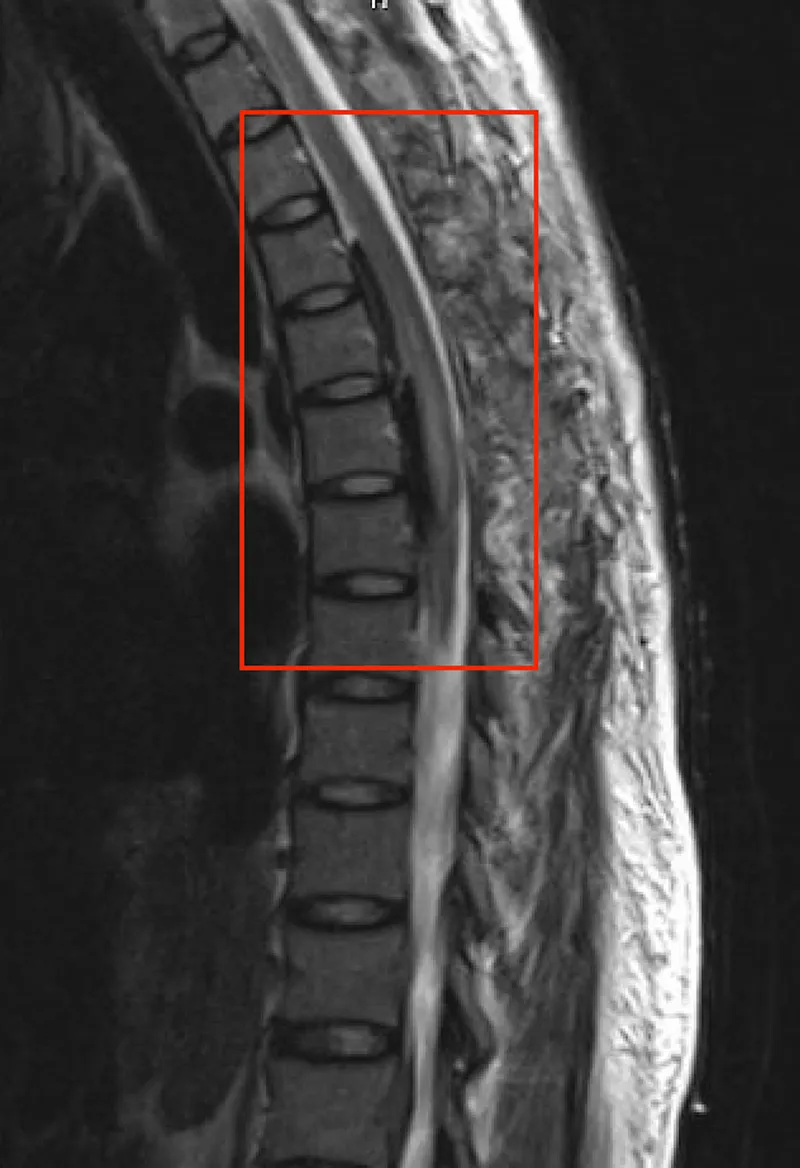
⭐ Spinal epidural hematoma is a neurological emergency requiring prompt diagnosis (MRI) and surgical decompression, ideally within 8-12 hours, to maximize chances of neurological recovery.
High‑Yield Points - ⚡ Biggest Takeaways
- LAST: CNS excitation (seizures) then depression, CVS toxicity (arrhythmias). Treat with lipid emulsion.
- PDPH: Postural headache, worse upright. Epidural blood patch for severe, persistent cases.
- Nerve Injury: Paresthesia, motor deficits from direct trauma, hematoma, or chemical irritation.
- Epidural Hematoma/Abscess: Back pain, fever, progressive neurological deficits. Urgent MRI and intervention.
- Total Spinal Anesthesia: Apnea, profound hypotension, unconsciousness. Immediate airway management.
- Pneumothorax: Risk with supraclavicular/intercostal blocks. Sudden dyspnea, chest pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

