Regional Anesthesia

On this page
🎯 The Precision Medicine Revolution: Regional Anesthesia Mastery
Regional anesthesia transforms surgical care by delivering targeted pain control while preserving consciousness and minimizing systemic effects-a precision tool that demands mastery of neuroanatomy, pharmacology, and procedural technique. You'll build from foundational nerve architecture through drug selection principles, then advance to clinical pattern recognition that guides technique optimization for specific surgical scenarios. By integrating evidence-based protocols with complication management strategies, you'll develop the systematic approach needed to deliver superior perioperative outcomes and position yourself at the forefront of modern anesthetic practice.
Master regional anesthesia principles, and you possess the foundation for precision pain management that transforms surgical outcomes while minimizing systemic complications.
🎯 The Precision Medicine Revolution: Regional Anesthesia Mastery
🧠 Neuroanatomical Command Center: The Foundation Architecture
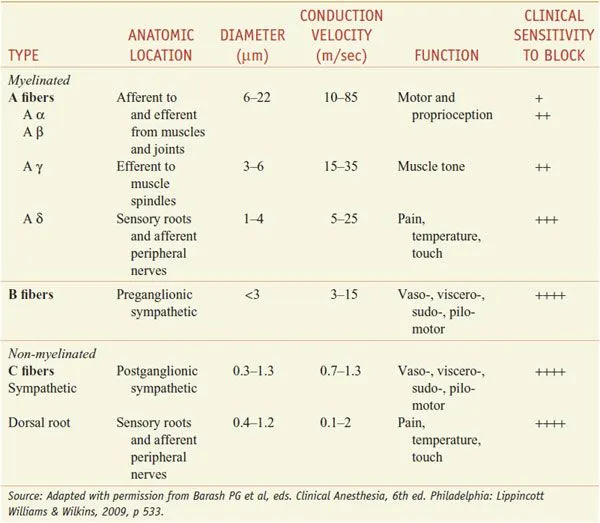
The neuroanatomical foundation centers on three critical fiber types with distinct anesthetic susceptibilities. A-delta fibers (2-5 μm diameter) carry sharp pain and succumb to local anesthetics at 0.5-1.0 mg/mL concentrations. C-fibers (0.4-1.2 μm diameter) transmit dull, aching pain and require 1.5-2.0 mg/mL concentrations for complete blockade. A-alpha motor fibers (12-20 μm diameter) resist blockade until concentrations reach 2.5-3.0 mg/mL, explaining why sensory block precedes motor paralysis.
📌 Remember: SPAM - Sensory (A-delta), Pain (C-fibers), Autonomic (B-fibers), Motor (A-alpha) - in order of increasing diameter and decreasing anesthetic sensitivity
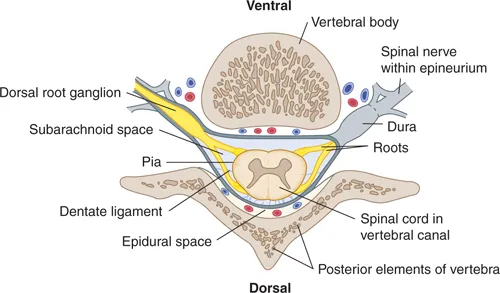
Spinal cord organization follows precise laminar architecture where Rexed laminae I-II process nociceptive input, laminae III-IV handle tactile sensation, and laminae VIII-IX control motor function. Local anesthetics block sodium channels with pKa values determining onset speed - lidocaine (pKa 7.9) achieves 50% ionization at physiologic pH, while bupivacaine (pKa 8.1) requires 15-20 minutes for complete diffusion across nerve membranes.
⭐ Clinical Pearl: Differential block occurs predictably - autonomic block extends 2-6 dermatomes above sensory level, sensory block 2-4 dermatomes above motor block, with 98% reliability in properly positioned patients
The blood-brain barrier and blood-nerve barrier create distinct pharmacokinetic compartments. Systemic absorption follows predictable patterns: intercostal blocks achieve peak plasma levels within 10-15 minutes, epidural injection peaks at 20-30 minutes, while peripheral nerve blocks demonstrate delayed absorption over 45-60 minutes. Understanding these kinetics prevents Local Anesthetic Systemic Toxicity (LAST), which occurs when plasma levels exceed 5 μg/mL for bupivacaine or 10 μg/mL for lidocaine.
| Nerve Fiber Type | Diameter (μm) | Myelination | Function | Block Concentration (mg/mL) | Onset Time (min) |
|---|---|---|---|---|---|
| A-alpha | 12-20 | Heavy | Motor | 2.5-3.0 | 15-30 |
| A-beta | 5-12 | Heavy | Touch/Pressure | 1.5-2.5 | 10-20 |
| A-delta | 2-5 | Light | Sharp Pain | 0.5-1.0 | 5-15 |
| B-fibers | 1-3 | Light | Autonomic | 0.25-0.5 | 3-10 |
| C-fibers | 0.4-1.2 | None | Dull Pain | 1.5-2.0 | 5-15 |
Understanding neuroanatomical architecture reveals why epidural anesthesia produces segmental block patterns while spinal anesthesia creates predictable dermatomal levels based on specific gravity and injection volume. This foundation enables precise clinical applications where anatomical knowledge translates directly into therapeutic success and complication avoidance.
Connect neuroanatomical mastery through pharmacological principles to understand how drug selection and dosing create targeted, reversible nerve blockade with predictable onset and duration patterns.
🧠 Neuroanatomical Command Center: The Foundation Architecture
⚗️ Pharmacological Precision Engine: Drug Selection Mastery
Local anesthetic pharmacology centers on sodium channel blockade with use-dependent inhibition - channels must open for drug binding, explaining why nerve stimulation enhances block onset and inflamed tissues resist anesthesia. Lipophilicity determines potency and duration: bupivacaine (lipophilicity coefficient 3420) provides 4-8 hour duration compared to lidocaine (coefficient 366) lasting 1-2 hours. Protein binding correlates directly with duration - bupivacaine (95% protein bound) versus lidocaine (65% protein bound) explains the 4-fold duration difference.
📌 Remember: PLOD - Potency (lipophilicity), Latency (pKa), Onset (concentration), Duration (protein binding) - the four pillars determining local anesthetic clinical profile
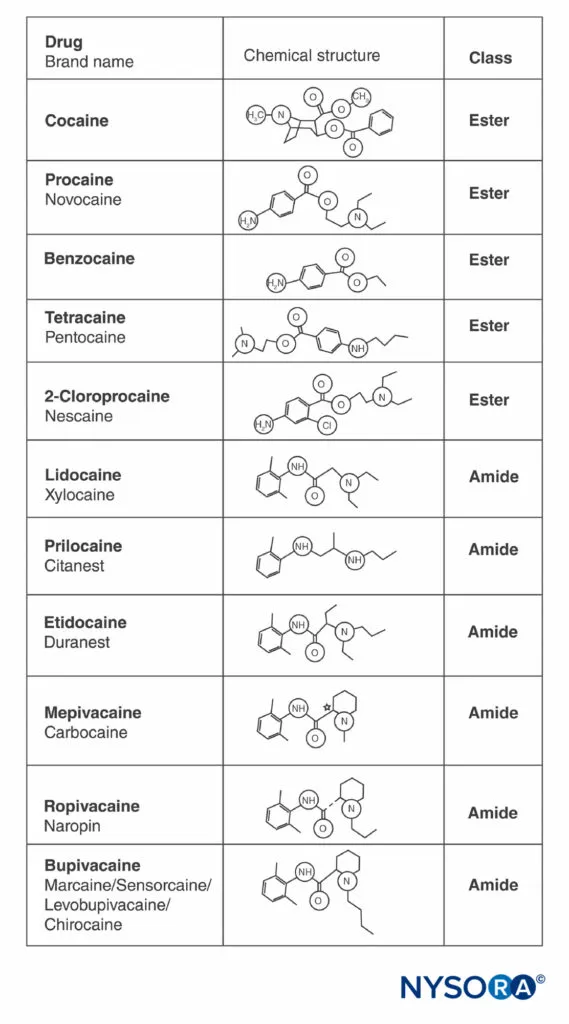
Ester versus amide classification determines metabolism pathways and allergic potential. Ester anesthetics (procaine, chloroprocaine) undergo plasma cholinesterase hydrolysis with half-lives of 30-60 seconds, while amide anesthetics (lidocaine, bupivacaine) require hepatic metabolism with half-lives of 90-120 minutes. True allergic reactions occur in <0.1% of patients and almost exclusively involve ester anesthetics due to para-aminobenzoic acid (PABA) metabolites.
Maximum safe dosing prevents systemic toxicity with strict weight-based calculations. Lidocaine maximum: 4.5 mg/kg plain or 7 mg/kg with epinephrine. Bupivacaine maximum: 2.5 mg/kg plain or 3 mg/kg with epinephrine. Epinephrine (1:200,000 concentration) reduces systemic absorption by 30-50% while extending duration by 50-100% through vasoconstriction and alpha-2 receptor activation.
⭐ Clinical Pearl: Cardiac toxicity threshold for bupivacaine occurs at plasma levels >4 μg/mL, while CNS toxicity begins at 2-3 μg/mL - explaining why neurological symptoms precede cardiac collapse in 85% of LAST cases
Adjuvant medications enhance block quality and duration through synergistic mechanisms. Dexmedetomidine (0.5-1 μg/kg) extends peripheral nerve block duration by 40-60% via alpha-2 receptor agonism and hyperpolarization-activated cation channel modulation. Clonidine (1-2 μg/kg) provides similar duration extension with additional sedation and 30% reduction in breakthrough pain. Dexamethasone (4-8 mg) prolongs single-shot blocks by 6-12 hours through anti-inflammatory effects and sodium channel modulation.
| Drug | Class | pKa | Onset (min) | Duration (hr) | Max Dose (mg/kg) | Protein Binding (%) |
|---|---|---|---|---|---|---|
| Lidocaine | Amide | 7.9 | 5-15 | 1-2 | 4.5 (7 w/epi) | 65 |
| Bupivacaine | Amide | 8.1 | 15-30 | 4-8 | 2.5 (3 w/epi) | 95 |
| Ropivacaine | Amide | 8.1 | 15-25 | 6-10 | 3.0 | 94 |
| Chloroprocaine | Ester | 8.7 | 5-10 | 0.5-1 | 11 | 0 |
| Mepivacaine | Amide | 7.6 | 10-20 | 2-4 | 4.5 | 77 |
💡 Master This: Baricity determines spinal anesthetic distribution - hyperbaric solutions (glucose 5-8%) follow gravity, isobaric solutions remain at injection level, while hypobaric solutions migrate cephalad, enabling predictable dermatomal control based on patient positioning and specific gravity calculations
Continuous infusion pharmacology requires steady-state calculations and accumulation awareness. Bupivacaine 0.125% at 8-12 mL/hr maintains therapeutic levels without plasma accumulation in healthy adults. Ropivacaine 0.2% at 6-10 mL/hr provides equivalent analgesia with reduced motor block and 40% lower cardiotoxicity risk due to faster sodium channel dissociation kinetics.
Understanding pharmacological precision enables rational drug selection where molecular properties predict clinical outcomes and safety profiles. This knowledge transforms regional anesthesia from empirical practice into evidence-based precision medicine with predictable results and minimized complications.
Connect pharmacological mastery through clinical pattern recognition to understand how drug selection and anatomical targeting create reproducible anesthetic outcomes across diverse surgical procedures and patient populations.
⚗️ Pharmacological Precision Engine: Drug Selection Mastery
🎯 Clinical Pattern Recognition Matrix: Diagnostic Excellence Framework
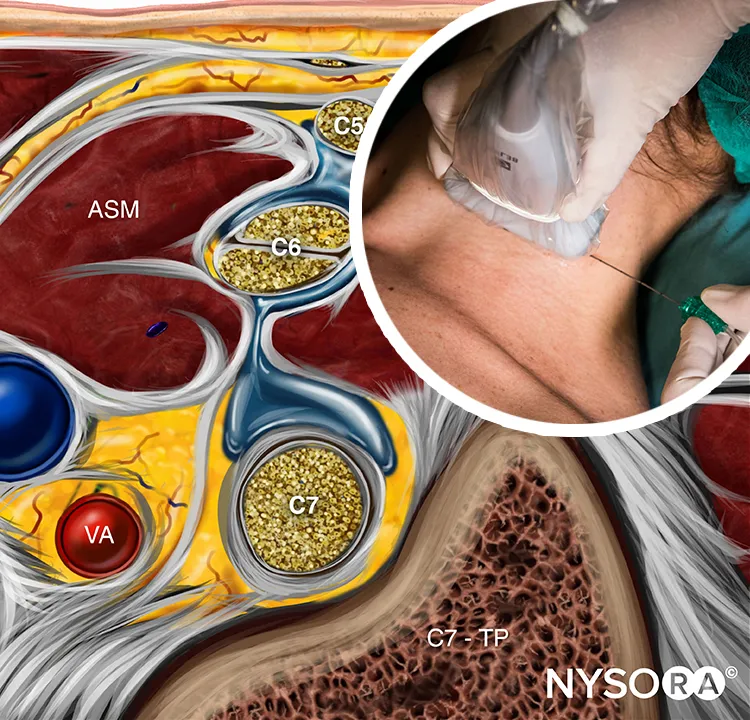
Block selection algorithms follow surgical site mapping with dermatomal correlation and motor preservation requirements. Upper extremity surgery demands brachial plexus targeting with approach selection based on surgical level: interscalene blocks for shoulder/proximal humerus (C5-C7 distribution), supraclavicular blocks for mid-humerus to fingertips (complete plexus), and axillary blocks for elbow/forearm procedures (terminal nerve branches). Success rates exceed 95% when anatomical approach matches surgical dermatomal requirements.
📌 Remember: SCAN - Shoulder (interscalene), Clavicle (supraclavicular), Arm (infraclavicular), Nerves (axillary) - matching brachial plexus approach to surgical site for optimal coverage
Neuraxial versus peripheral decision trees integrate patient factors, surgical requirements, and postoperative goals. Spinal anesthesia suits procedures <3 hours with T10 or lower dermatomal requirements, achieving 100% success rates with 5-15 minute onset. Epidural anesthesia enables titrated levels, extended duration, and postoperative analgesia but requires 20-30 minute onset and carries 5-10% failure rates. Combined spinal-epidural (CSE) provides immediate onset with extended duration capability for complex procedures requiring >4 hour anesthesia.
Contraindication recognition prevents catastrophic complications through systematic risk assessment. Absolute contraindications include patient refusal, infection at injection site, severe coagulopathy (INR >1.5, platelets <50,000), and severe hypovolemia. Relative contraindications require risk-benefit analysis: mild coagulopathy, sepsis without local infection, severe spinal deformity, and previous back surgery with hardware placement.
⭐ Clinical Pearl: Anticoagulation timing follows strict guidelines - warfarin discontinued 5 days (INR <1.5), clopidogrel stopped 7 days, rivaroxaban held 72 hours, with neuraxial catheter removal requiring normal coagulation and 12-hour anticoagulant delay post-removal
Ultrasound pattern recognition revolutionizes peripheral nerve identification with real-time visualization and 90-95% success rates. Hyperechoic structures (bone, fascia) appear bright white, hypoechoic structures (muscle, nerves) appear dark gray, and anechoic structures (blood vessels, local anesthetic) appear black. Nerve identification requires honeycomb internal architecture with hyperechoic perineurium and hypoechoic fascicles.
| Block Type | Success Rate (%) | Onset Time (min) | Duration (hr) | Motor Block | Complications (%) |
|---|---|---|---|---|---|
| Spinal | 98-100 | 5-15 | 2-4 | Complete | 1-3 |
| Epidural | 90-95 | 20-30 | 2-6 | Variable | 3-5 |
| Interscalene | 95-98 | 15-25 | 12-18 | Shoulder/arm | 2-4 |
| Supraclavicular | 92-96 | 10-20 | 10-16 | Hand/forearm | 1-2 |
| Femoral | 90-95 | 20-30 | 8-12 | Quadriceps | <1 |
💡 Master This: Test dose protocols prevent intravascular injection - lidocaine 45 mg with epinephrine 15 μg produces heart rate increase >20 bpm within 60 seconds if intravascular, while motor weakness within 5 minutes indicates intrathecal placement during epidural attempts
Anatomical landmark correlation with surface anatomy enables accurate needle placement without imaging guidance. Tuffier's line (intercristal line) identifies L4-L5 interspace in 85% of patients, while C7 spinous process (vertebra prominens) guides cervical epidural approaches. Brachial plexus surface landmarks include cricoid cartilage level for interscalene approach and subclavian artery pulsation for supraclavicular targeting.
Physiological monitoring confirms block adequacy through objective assessment. Pinprick sensation tests A-delta fiber function, cold sensation evaluates C-fiber blockade, and motor testing assesses A-alpha fiber interruption. Sympathetic blockade manifests as skin temperature increase >2°C, Horner's syndrome (interscalene blocks), or hypotension (neuraxial blocks) within 15-30 minutes.
Understanding clinical pattern recognition transforms regional anesthesia from technical procedure into diagnostic art where systematic assessment guides optimal technique selection and real-time problem-solving ensures consistent success across diverse clinical scenarios.
Connect pattern recognition mastery through systematic comparison frameworks to understand how technique variations and patient factors influence block selection and outcome optimization in complex clinical situations.
🎯 Clinical Pattern Recognition Matrix: Diagnostic Excellence Framework
⚖️ Systematic Discrimination Engine: Technique Optimization Matrix
Neuraxial technique discrimination centers on procedure duration, surgical level, and postoperative requirements with mathematical precision. Spinal anesthesia dominates procedures <3 hours with T10 or lower requirements, achieving 98-100% success with single injection simplicity. Epidural anesthesia suits procedures >3 hours, upper abdominal surgery, or postoperative analgesia requirements, providing titrated control at the cost of 20-30 minute onset and 5-10% failure rates. Combined spinal-epidural offers immediate onset with duration flexibility for complex procedures requiring >4 hours with uncertain timing.
📌 Remember: STEP - Spinal (short procedures), Titrated (epidural), Extended (CSE), Peripheral (specific regions) - matching anesthetic technique to surgical and patient requirements
Peripheral versus neuraxial decision algorithms integrate surgical site, patient comorbidities, and anticoagulation status with quantitative thresholds. Peripheral nerve blocks excel when neuraxial contraindications exist (coagulopathy, infection, patient refusal) or unilateral procedures benefit from preserved contralateral function. Success rates for ultrasound-guided peripheral blocks reach 90-95% with reduced systemic effects and preserved hemodynamic stability.
Anticoagulation discrimination follows strict timing protocols based on drug pharmacokinetics and bleeding risk assessment. Neuraxial procedures require normal coagulation: warfarin stopped 5 days (INR <1.5), rivaroxaban held 72 hours, enoxaparin discontinued 24 hours (therapeutic dose) or 12 hours (prophylactic dose). Peripheral blocks tolerate mild anticoagulation but deep blocks (psoas, paravertebral) carry similar bleeding risks to neuraxial techniques.
| Technique | Onset (min) | Duration (hr) | Success Rate (%) | Contraindications | Bleeding Risk |
|---|---|---|---|---|---|
| Spinal | 5-15 | 2-4 | 98-100 | Coagulopathy, infection | High |
| Epidural | 20-30 | 2-6 | 90-95 | Coagulopathy, infection | High |
| Peripheral | 15-30 | 8-18 | 90-95 | Local infection | Low-Moderate |
| IV Regional | 5-10 | 0.5-1 | 95-98 | Severe PVD, sickle cell | Low |
| Topical | 30-60 | 1-2 | 70-80 | Allergy, broken skin | Minimal |
⭐ Clinical Pearl: Pregnancy physiology alters regional anesthesia requirements - 30% dose reduction for neuraxial blocks due to epidural vein engorgement, increased sensitivity from progesterone effects, and aortocaval compression requiring left uterine displacement after 20 weeks gestation
Block-specific discrimination matches anatomical approach to surgical requirements with dermatomal precision. Interscalene blocks provide excellent shoulder analgesia but cause 100% phrenic nerve block and incomplete ulnar coverage. Supraclavicular blocks offer complete arm anesthesia with <5% phrenic nerve involvement but carry pneumothorax risk in inexperienced hands. Axillary blocks avoid pneumothorax and phrenic nerve block but provide incomplete coverage for shoulder/upper arm procedures.
Continuous versus single-shot discrimination depends on postoperative pain duration and functional recovery goals. Continuous peripheral nerve catheters reduce opioid consumption by 60-80% and improve patient satisfaction for major orthopedic procedures but require catheter management and infection prevention protocols. Single-shot blocks suit outpatient procedures with predictable pain duration and simplified management.
💡 Master This: Local anesthetic concentration determines sensory versus motor block intensity - bupivacaine 0.125% provides pure sensory block, 0.25% produces mild motor weakness, while 0.5% causes complete motor paralysis, enabling tailored block characteristics based on surgical and recovery requirements
Rescue technique algorithms address failed or inadequate blocks through systematic troubleshooting. Incomplete spinal anesthesia may require patient repositioning, supplemental sedation, or conversion to general anesthesia based on block height and surgical requirements. Failed peripheral blocks benefit from ultrasound confirmation, alternative approaches, or neuraxial backup depending on time constraints and patient factors.
Complication risk stratification guides technique selection through evidence-based risk assessment. Neuraxial hematoma risk increases 100-fold with therapeutic anticoagulation, while peripheral nerve injury occurs in <0.1% of ultrasound-guided blocks compared to 2-4% with nerve stimulator techniques. LAST incidence varies from 0.01% (peripheral blocks) to 0.1% (intercostal blocks) based on injection site vascularity.
Understanding systematic discrimination enables optimal technique selection where quantitative patient assessment and evidence-based algorithms guide individualized anesthetic plans that maximize surgical success while minimizing complications through precision medicine principles.
Connect systematic discrimination through evidence-based treatment algorithms to understand how technique optimization and complication management create superior patient outcomes with measurable quality improvements and enhanced safety profiles.
⚖️ Systematic Discrimination Engine: Technique Optimization Matrix
🏥 Evidence-Based Treatment Command: Outcome Optimization Protocols
Treatment algorithm optimization follows evidence-based protocols that integrate patient factors, surgical requirements, and institutional capabilities with quantitative outcome measures. Enhanced Recovery After Surgery (ERAS) protocols incorporating regional anesthesia reduce hospital length of stay by 1-2 days, opioid consumption by 50-70%, and postoperative complications by 30-40% across multiple surgical specialties. Standardized block protocols achieve >95% success rates with <2% complication rates when systematic approaches replace individualized variations.
Multimodal analgesia integration optimizes pain control while minimizing opioid-related complications through synergistic drug combinations and regional techniques. Acetaminophen (1000 mg q6h) provides baseline analgesia with 30% opioid-sparing effect. NSAIDs (ibuprofen 400 mg q6h, ketorolac 30 mg q6h) reduce inflammatory pain and opioid requirements by 25-40%. Regional blocks eliminate surgical nociception while preserving consciousness and avoiding systemic side effects.
📌 Remember: RAMP - Regional (primary), Acetaminophen (baseline), Multimodal (NSAIDs), PRN opioids (rescue) - the evidence-based hierarchy for optimal postoperative analgesia
Continuous peripheral nerve catheter protocols provide extended analgesia with superior outcomes compared to systemic opioids for major orthopedic procedures. Bupivacaine 0.125% at 8-12 mL/hr maintains effective analgesia for 48-72 hours with minimal motor block. Patient-controlled regional analgesia (PCRA) with 5 mL boluses and 30-minute lockout improves patient satisfaction while reducing nursing workload and medication errors.
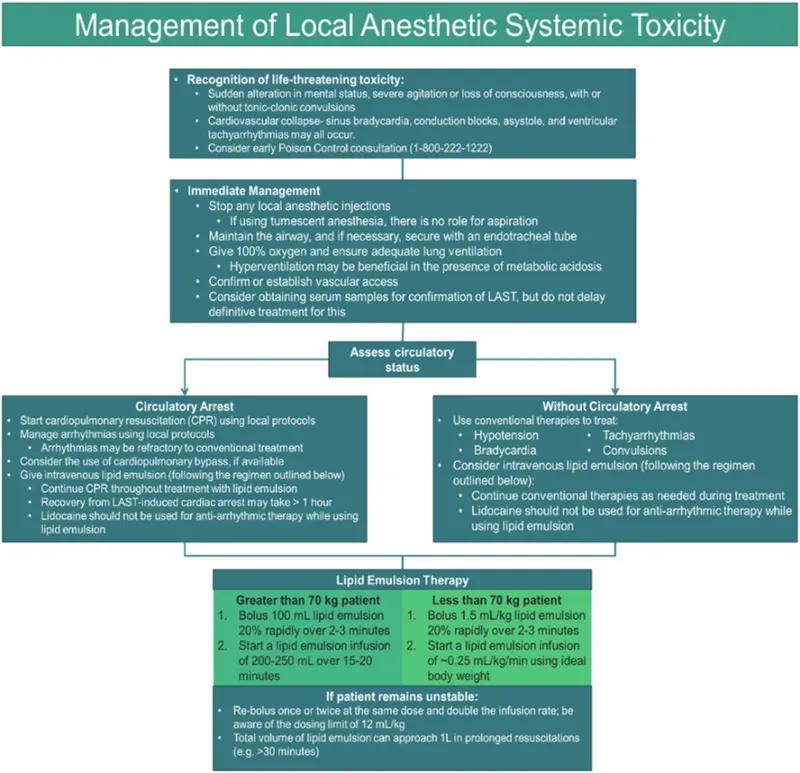
Complication management algorithms address adverse events through systematic recognition and evidence-based interventions. Local Anesthetic Systemic Toxicity (LAST) requires immediate recognition (perioral numbness, tinnitus, seizures) and lipid emulsion therapy (1.5 mL/kg 20% intralipid bolus, then 0.25 mL/kg/min infusion). High spinal anesthesia demands airway management, vasopressor support (phenylephrine 100-200 μg boluses), and atropine for bradycardia.
| Complication | Incidence (%) | Recognition | Treatment | Prevention |
|---|---|---|---|---|
| LAST | 0.01-0.1 | CNS/CV symptoms | Lipid emulsion | Dose limits, aspiration |
| Pneumothorax | 0.5-6 | Chest pain, dyspnea | Chest tube | Ultrasound guidance |
| Nerve Injury | 0.02-2 | Persistent deficit | Neurology consult | Avoid paresthesias |
| Epidural Hematoma | 0.0001 | Back pain, weakness | Emergency surgery | Coagulation assessment |
| Infection | 0.1-1 | Fever, erythema | Antibiotics | Sterile technique |
⭐ Clinical Pearl: Ultrasound guidance reduces complications by 50-70% and improves success rates by 10-15% compared to landmark techniques, with cost-effectiveness demonstrated through reduced block failures, decreased procedure time, and improved patient outcomes
Postoperative monitoring protocols ensure patient safety while optimizing recovery. Neurological assessments every 2-4 hours detect early complications, while pain scores and functional assessments guide analgesic adjustments. Catheter site inspection twice daily prevents infection, and systematic documentation enables quality assurance and continuous improvement.
Discharge planning integration coordinates regional anesthesia with outpatient management to optimize recovery and prevent complications. Patient education regarding expected block duration, safety precautions, and emergency contacts reduces anxiety and improves satisfaction. Structured follow-up at 24-48 hours identifies complications and assesses recovery progress.
💡 Master This: Regional anesthesia protocols integrated with ERAS pathways achieve triple aim healthcare goals - improved patient experience (reduced pain, faster recovery), better population health (reduced opioid dependence), and lower costs (shorter stays, fewer complications) with measurable outcomes across multiple quality domains
Technology integration enhances protocol implementation through decision support systems, electronic documentation, and real-time monitoring. Smart pumps with drug libraries prevent dosing errors, while electronic health records provide clinical decision support and automated alerts for contraindications or drug interactions.
Understanding evidence-based treatment protocols transforms regional anesthesia from individual technique into systematic care delivery where standardized approaches achieve superior outcomes, enhanced safety, and improved efficiency through continuous quality improvement and evidence-based practice.
Connect treatment optimization through advanced integration concepts to understand how regional anesthesia interfaces with emerging technologies, personalized medicine, and healthcare system transformation to create next-generation perioperative care.
🏥 Evidence-Based Treatment Command: Outcome Optimization Protocols
🔗 Advanced Integration Nexus: Next-Generation Perioperative Architecture
Artificial intelligence integration revolutionizes block planning and outcome prediction through machine learning algorithms that analyze thousands of patient variables simultaneously. AI-powered ultrasound systems achieve >98% nerve identification accuracy compared to 85-90% human performance, while predictive algorithms forecast block success probability based on patient anatomy, operator experience, and technique variables. Real-time guidance systems provide needle trajectory optimization and injection volume recommendations with millimeter precision.
📌 Remember: SMART - Smart imaging (AI ultrasound), Machine learning (outcome prediction), Augmented reality (guidance), Real-time (monitoring), Telemedicine (remote consultation) - the five pillars of next-generation regional anesthesia
Personalized medicine algorithms tailor anesthetic selection and dosing based on genetic polymorphisms, pharmacokinetic modeling, and individual patient characteristics. CYP2D6 genetic variants affect local anesthetic metabolism in 7-10% of patients, requiring dose adjustments to prevent toxicity or inadequate anesthesia. Pharmacogenomic testing enables precision dosing that optimizes efficacy while minimizing adverse effects through individualized drug selection.
Augmented reality (AR) systems overlay anatomical structures onto real-time ultrasound images, enabling novice practitioners to achieve expert-level accuracy in nerve identification and needle placement. AR guidance reduces learning curve from 50-100 procedures to 10-20 procedures while maintaining >95% success rates. Virtual reality training provides risk-free practice with haptic feedback and performance analytics that accelerate skill acquisition.
Internet of Things (IoT) integration creates comprehensive monitoring ecosystems where smart catheters, wearable sensors, and mobile applications provide continuous patient assessment and early complication detection. Smart infusion pumps automatically adjust flow rates based on pain scores and activity levels, while pressure sensors detect catheter displacement or occlusion in real-time.
| Technology | Current Capability | Future Potential | Implementation Timeline | Cost Impact |
|---|---|---|---|---|
| AI Ultrasound | 98% nerve ID | Automated injection | 2-3 years | 20% reduction |
| AR Guidance | Real-time overlay | Predictive modeling | 3-5 years | 30% efficiency |
| Smart Catheters | Pressure monitoring | Drug delivery control | 1-2 years | 15% cost savings |
| Genetic Testing | Metabolism prediction | Personalized dosing | 5-10 years | Variable |
| Robotics | Needle guidance | Autonomous injection | 10+ years | Unknown |
⭐ Clinical Pearl: Blockchain technology ensures secure data sharing and immutable documentation of regional anesthesia procedures, enabling multi-institutional research, quality improvement, and medicolegal protection while maintaining patient privacy and data integrity
Nanotechnology applications create targeted drug delivery systems that enhance local anesthetic efficacy while reducing systemic exposure. Liposomal bupivacaine extends duration to 72+ hours through controlled release mechanisms, while nanoparticle carriers enable site-specific delivery with minimal systemic absorption. Smart polymers respond to pH changes or enzymatic activity to modulate drug release based on tissue conditions.
Robotic assistance provides superhuman precision in needle placement with sub-millimeter accuracy and tremor elimination. Robotic ultrasound maintains optimal probe positioning while automated injection systems deliver precise volumes at calculated rates. Force feedback prevents tissue damage while ensuring adequate penetration for successful nerve blockade.
Predictive analytics integrate multiple data streams to forecast complications and optimize outcomes before problems manifest. Machine learning models analyze vital signs, laboratory values, imaging data, and procedure variables to predict LAST risk, block failure probability, and recovery trajectories with >90% accuracy.
💡 Master This: Digital twin technology creates virtual patient models that simulate anesthetic responses and predict outcomes before actual procedures, enabling risk-free planning, technique optimization, and complication prevention through computational modeling and real-time data integration
Sustainability integration addresses environmental impact through eco-friendly practices and resource optimization. Reusable ultrasound probe covers, biodegradable catheters, and reduced packaging minimize medical waste while maintaining sterility standards. Energy-efficient equipment and optimized workflows reduce carbon footprint without compromising patient care.
Global health applications adapt advanced technologies for resource-limited settings through simplified interfaces, portable equipment, and cost-effective solutions. Smartphone-based ultrasound and AI-assisted guidance democratize regional anesthesia expertise while telemedicine support provides quality assurance and continuing education in underserved regions.
Understanding advanced integration reveals how regional anesthesia evolves from traditional techniques into intelligent systems that predict, adapt, and optimize patient care through technology convergence and data-driven insights that transform perioperative medicine into precision healthcare delivery.
Connect advanced integration mastery through rapid reference tools to understand how emerging technologies and evidence-based protocols synthesize into practical clinical frameworks that enable immediate implementation and continuous improvement in daily practice.
🔗 Advanced Integration Nexus: Next-Generation Perioperative Architecture
🎯 Clinical Mastery Arsenal: Rapid Excellence Framework
Essential Threshold Arsenal provides instant reference for critical clinical decisions with evidence-based parameters that prevent complications and optimize outcomes. Maximum safe doses: lidocaine 4.5 mg/kg (7 mg/kg with epinephrine), bupivacaine 2.5 mg/kg (3 mg/kg with epinephrine), ropivacaine 3 mg/kg. LAST recognition thresholds: plasma bupivacaine >4 μg/mL causes cardiac toxicity, >2 μg/mL produces CNS symptoms. Lipid emulsion dosing: 1.5 mL/kg bolus, then 0.25 mL/kg/min infusion for LAST treatment.
📌 Remember: DOSES - Determine weight, Optimal concentration, Safety limits, Epinephrine effects, Systemic monitoring - the five-step protocol for safe local anesthetic administration
Rapid Block Selection Matrix enables instant technique optimization based on surgical requirements and patient factors. Upper extremity: interscalene (shoulder), supraclavicular (arm), axillary (hand). Lower extremity: femoral (anterior thigh), sciatic (posterior leg), ankle (foot). Truncal: TAP (abdominal wall), ESP (thoracic), PEC (breast). Success rates >95% with appropriate technique selection and ultrasound guidance.
Complication Recognition Algorithms provide systematic assessment and immediate intervention protocols. High spinal signs: difficulty speaking, upper extremity weakness, respiratory distress - treat with airway support, vasopressors, atropine. Pneumothorax symptoms: chest pain, dyspnea, decreased breath sounds - obtain chest X-ray, consider chest tube if >20% collapse. Nerve injury indicators: persistent numbness >24 hours, motor weakness, burning pain - neurology consultation within 48 hours.
| Emergency | Recognition | Immediate Action | Definitive Treatment | Prevention |
|---|---|---|---|---|
| LAST | Perioral numbness, seizures | Lipid emulsion, airway | ICU monitoring | Dose limits |
| High Spinal | Upper extremity weakness | Vasopressors, ventilation | Supportive care | Proper dosing |
| Pneumothorax | Chest pain, dyspnea | Oxygen, chest X-ray | Chest tube | US guidance |
| Hematoma | Back pain, weakness | Emergency MRI | Surgical evacuation | Coagulation check |
| Infection | Fever, site erythema | Blood cultures | Antibiotics | Sterile technique |
⭐ Clinical Pearl: Hydrodissection technique confirms correct needle placement - 1-2 mL saline injection should separate tissue planes and surround target nerve before local anesthetic administration, preventing intraneural injection and nerve damage
Continuous Catheter Management Protocol optimizes extended analgesia while preventing complications. Initial bolus: 20-30 mL of 0.25% bupivacaine for dense block. Maintenance infusion: 0.125% bupivacaine at 8-12 mL/hr with 5 mL boluses every 30 minutes PRN. Daily assessment: catheter site inspection, neurological examination, pain scores, local anesthetic consumption.
Quality Metrics Dashboard enables continuous improvement through systematic outcome measurement. Target benchmarks: block success rate >95%, patient satisfaction >8/10, complication rate <2%, procedure time <30 minutes. Monthly reviews identify improvement opportunities and maintain performance standards through data-driven feedback.
Emergency Drug Calculations provide instant dosing for critical situations. Lipid emulsion: 1.5 mL/kg (105 mL for 70 kg patient) bolus, then 0.25 mL/kg/min (17.5 mL/min) infusion. Phenylephrine: 100-200 μg boluses for hypotension. Atropine: 0.5-1 mg for bradycardia. Epinephrine: 10-100 μg for severe hypotension or cardiac arrest.
💡 Master This: Regional anesthesia excellence requires systematic preparation, evidence-based protocols, and continuous learning - master these essential tools and critical thresholds to deliver consistent outcomes, prevent complications, and optimize patient care through precision medicine and clinical expertise
Mobile Reference Integration enables point-of-care access to critical information through smartphone applications and digital resources. Dosing calculators, anatomy references, ultrasound images, and emergency protocols provide instant guidance during procedures and crisis management. Regular updates ensure current evidence and best practices remain immediately accessible.
Understanding the clinical mastery arsenal transforms regional anesthesia practice from technique-based procedures into systematic excellence where evidence-based protocols, critical thresholds, and rapid decision frameworks enable consistent success, complication prevention, and optimal patient outcomes through precision medicine and continuous improvement.
🎯 Clinical Mastery Arsenal: Rapid Excellence Framework
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























