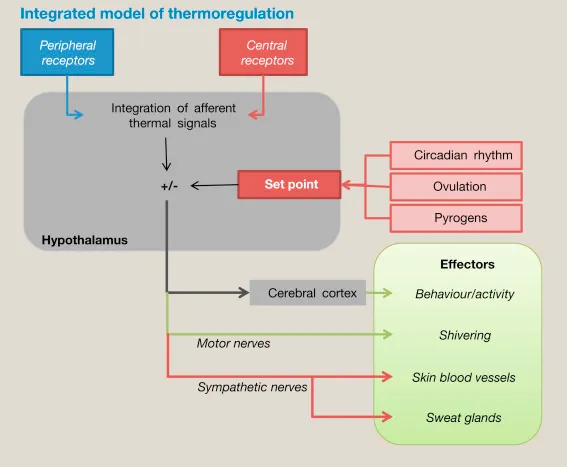
Thermoregulation & Post-Op Impact - Body's Thermostat
- Hypothalamus: Central "thermostat" regulating core body temperature (normal: 36.5-37.5°C).
- Mechanisms: Vasoconstriction/shivering (↑ heat production/conservation), vasodilation/sweating (↑ heat loss).
- Anesthesia's disruption:
- Impairs central hypothalamic regulation.
- Causes peripheral vasodilation, promoting heat loss.
- Decreases metabolic heat production.
- Surgical factors: Environmental exposure, cold IV fluids, open body cavities exacerbate heat loss.
- Consequence: High risk of Inadvertent Perioperative Hypothermia (IPH).
⭐ General anesthesia significantly widens the interthreshold range (core temperatures triggering autonomic responses like shivering/sweating) from ~0.2°C to as much as 4°C.
Postoperative Hypothermia - The Big Chill
- Core body temperature < 36°C (96.8°F).
- Causes: Cold OR, anaesthesia (vasodilation, ↓thermoregulation), cold IV fluids, open cavities.
- Phases:
- Redistribution (core → periphery): Rapid initial drop.
- Linear decline: Heat loss > production.
- Plateau: Vasoconstriction, shivering (if unblocked).
- Consequences:
- Cardiovascular: Arrhythmias, ischemia, ↑BP.
- Coagulation: ↑Bleeding (platelet/enzyme dysfunction).
- Wound: ↑Infection risk, impaired healing.
- Drug metabolism: Prolonged effects (e.g., relaxants).
- Shivering: ↑O2 consumption (~300-500%), ↑cardiac work, discomfort.
- Prevention & Management:
- Pre-warming, OR temp > 21°C.
- Active warming: Forced-air (most effective), warm IV fluids.
- Treat shivering: Meperidine (12.5-25mg IV), clonidine.
⭐ Mild hypothermia (34-36°C) significantly increases surgical site infection rates and adverse cardiac outcomes.
![Image of forced-air warming device applied to a postoperative patient]
Postoperative Hyperthermia/Fever - Feeling Hot Hot Hot
- Core temperature > 38°C (100.4°F) post-surgery.
- Causes (The 5 Ws) 📌:
- Wind (POD 1-2): Atelectasis, pneumonia.
- Water (POD 3-5): UTI.
- Wound (POD 5-7): Surgical Site Infection (SSI).
- Walking (POD 5+): DVT/PE.
- Wonder Drugs: Drug fever, transfusion reactions, Malignant Hyperthermia (MH).
- Malignant Hyperthermia: Rare; suspect with high fever, rigidity, ↑ETCO₂. Dantrolene.
- Non-infectious: Surgical stress (common <48h, <38.5°C), pancreatitis.
- Workup: Guided by timing/signs. CBC, cultures, CXR.
- Management: Treat cause; antipyretics.

⭐ Most early fevers (<48h post-op) are non-infectious, due to surgical stress (cytokine release).
Temperature Monitoring Techniques - Keeping Tabs
- Core Sites (Reflect true body core temp):
- Gold Standard: Pulmonary artery.
- Reliable: Distal esophagus, nasopharynx, tympanic (brain temp).
- Slower response: Bladder, rectal.
- 📌 PENTBR: Pulmonary Artery, Esophagus, Nasopharynx, Tympanic, Bladder, Rectal.
- Peripheral Sites (Screening, less accurate):
- Skin, axillary.
⭐ Tympanic membrane temperature closely reflects brain temperature due to shared blood supply from carotid artery.
High-Yield Points - ⚡ Biggest Takeaways
- Postoperative hypothermia (<36°C) ↑ risks of SSIs, cardiac events, and impaired wound healing.
- Shivering dramatically ↑ O2 consumption (up to 500%) and myocardial stress.
- Core temperature monitoring (e.g., esophageal, tympanic) is crucial, not peripheral.
- Forced-air warming is the most effective active rewarming technique.
- Malignant hyperthermia can present postoperatively; treat urgently with dantrolene.
- Postoperative fever often indicates infection; investigate promptly.
- Treat postoperative shivering with meperidine, clonidine, or tramadol.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more