Intro & Risk Factors - Delirium Drama Unveiled
Postoperative Delirium (POD): Acute confusional state. Fluctuating course, inattention, disorganized thinking/altered consciousness. Common, serious. ↑Morbidity, ↑mortality, ↑length of stay (LOS), ↑costs, potential long-term cognitive decline.
Risk Factors:
- Predisposing (Patient-Specific):
- Age >65 years
- Pre-existing cognitive impairment (e.g., dementia)
- History of delirium
- Sensory impairment (vision/hearing)
- Multiple comorbidities / Frailty
- Alcohol/substance use history
- Precipitating (Perioperative/Hospital):
- Type of surgery (major, emergency, cardiac, orthopedic)
- Culprit drugs: 📌 BOA (Benzodiazepines, Opioids, Anticholinergics)
- Uncontrolled pain
- Infections (UTI, pneumonia)
- Metabolic disturbances (hypoxia, electrolytes)
- Sleep deprivation, ICU environment
- Use of physical restraints, catheters
⭐ > Advanced age (>65 years) is a primary non-modifiable risk factor for POD.
Pathophysiology & Etiology - Neuro-Chaos Culprits
- Multifactorial Origin: Patient vulnerability (e.g., advanced age, prior cognitive impairment) meets precipitating factors (e.g., major surgery, specific drugs, infection).
- Neurotransmitter Dysregulation:
- Acetylcholine (ACh) ↓: Central cholinergic deficiency; critical for attention & memory.
- Dopamine (DA) ↑: Often reciprocal to ACh levels; linked to agitation & psychosis.
- Others: Serotonin, GABA, norepinephrine imbalances contribute.
- Neuroinflammation:
- Systemic inflammation (e.g., post-surgery, sepsis) → ↑pro-inflammatory cytokines (IL-1β, IL-6, TNF-α).
- Microglial cell activation & blood-brain barrier (BBB) disruption ensue.
- Network Disruption: Impaired brain connectivity & functional integration among neural networks.
- Other Contributing Factors: Cerebral hypoxia, metabolic derangements (electrolytes, glucose), ↑cortisol (stress response).
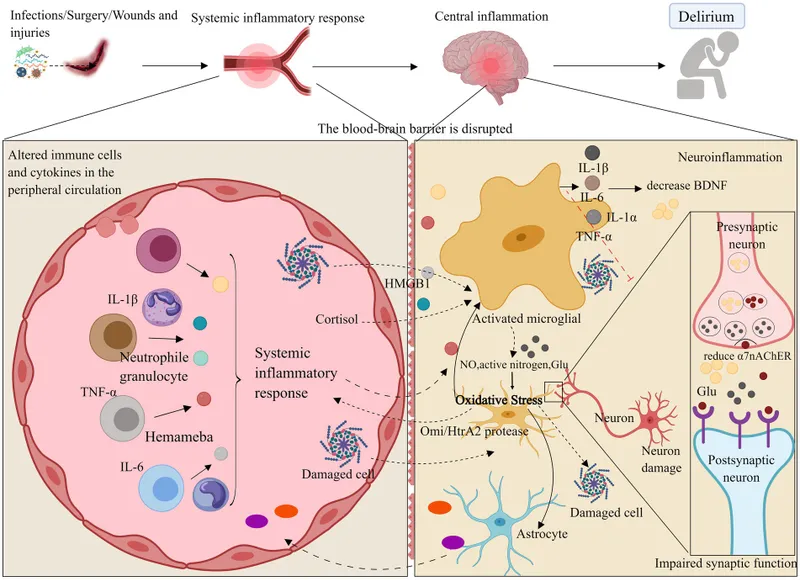
⭐ Central cholinergic deficiency is a cornerstone theory in the pathophysiology of postoperative delirium, highlighting the importance of acetylcholine in maintaining normal cognitive function.
Clinical Features & Diagnosis - Confusion Clue Hunt
- Core Features: Acute onset, fluctuating course, inattention, disorganized thinking, altered level of consciousness.
- Associated Symptoms:
- Perceptual disturbances (hallucinations, illusions)
- Sleep-wake cycle disruption
- Psychomotor changes (agitation or retardation)
- Emotional lability
- Diagnosis: Primarily clinical.
- Standardized tools:
- CAM (Confusion Assessment Method) - most common.
- CAM-ICU for ventilated patients.
- 4AT
- Key: Rule out mimics (hypoxia, hypoglycemia, sepsis, stroke, drug effects).
- 📌 DELIRIUMS Mnemonic: Drugs, Electrolyte imbalance, Lack of drugs (withdrawal), Infection, Reduced sensory input/Retention, Intracranial, Urinary/fecal retention, Myocardial/Pulmonary.
- Standardized tools:
⭐ CAM diagnostic algorithm requires: 1) Acute onset & fluctuating course AND 2) Inattention, PLUS EITHER 3) Disorganized thinking OR 4) Altered level of consciousness.
Prevention & Management - Mind Menders' Manual
Prevention: 📌 Multicomponent Interventions
- Optimize pain management: Multimodal, opioid-sparing.
- Medication review: Avoid/minimize high-risk drugs (e.g., benzodiazepines, anticholinergics).
- Promote sleep: Maintain sleep-wake cycles, minimize nighttime disruptions.
- Early mobilization & activity.
- Sensory aids: Ensure use of glasses, hearing aids.
- Cognitive orientation: Frequent reorientation, familiar environment.
- Hydration & nutrition: Maintain.
- Prevent/treat infection, hypoxia, electrolyte imbalances.
Management Flowchart:
Pharmacological (Judicious Use):
- Haloperidol: 0.5-1 mg IV/IM/PO (max 3-5 mg/24h). ⚠️ Monitor QTc.
- Atypical antipsychotics (e.g., Risperidone 0.25-0.5 mg, Olanzapine 2.5-5 mg).
- Dexmedetomidine: Option for ICU delirium, especially if ventilated; less respiratory depression.
⭐ Benzodiazepines are generally contraindicated in non-alcohol/sedative withdrawal delirium as they can worsen it.
High‑Yield Points - ⚡ Biggest Takeaways
- Postoperative delirium: acute, fluctuating mental status change, especially in elderly post-surgery.
- Core features: inattention, disorganized thinking, altered consciousness, and perceptual disturbances.
- Key risks: advanced age, prior cognitive impairment, polypharmacy, major surgery (cardiac/orthopedic).
- Prevention: Multicomponent non-pharmacological strategies are paramount (reorientation, sleep, mobilization).
- Management: Treat underlying cause(s); low-dose antipsychotics for severe agitation; strictly avoid benzodiazepines.
- Prognosis: Linked to ↑morbidity, ↑mortality, prolonged hospital stay, and potential long-term cognitive decline.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

