PCA Basics - Pain Power to Patients
- PCA: Method where patients self-administer small, preset IV analgesic doses (usually opioids) via a programmable pump.
- Aim: Improved pain control, ↑ patient autonomy, reduced delays.
- Key Settings:
- Demand Dose (Bolus): Patient-triggered.
- Lockout Interval: Prevents overdose (e.g., 5-15 min).
- Basal/Background Infusion (Optional): Continuous rate.
- (Sometimes) 1 or 4-hour limits.

⭐ PCA generally provides superior analgesia and higher patient satisfaction compared to traditional intermittent opioid injections.
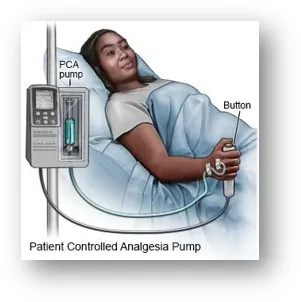
PCA Setup - Buttons & Boluses
- Patient Demand Button: Allows patient self-administration of analgesia.
- Bolus Dose: Pre-set amount of opioid (e.g., Morphine 1-2 mg, Fentanyl 10-20 mcg) delivered when button pressed.
- Lockout Interval: Mandatory delay (5-15 minutes) after a bolus before the next dose can be given. Prevents rapid re-dosing.
- Background/Basal Infusion: Optional continuous low-dose infusion; use cautiously.
- Dose Limits: Maximum drug amount allowed in a set period (e.g., 1-hour or 4-hour limits).
⭐ The lockout interval is a critical safety feature in PCA pumps, preventing over-sedation from too-frequent dosing.
PCA Drugs - Opioid Options
- Morphine:
- Standard choice, hydrophilic.
- Active metabolites (M6G, M3G); caution: renal impairment.
- Onset: 5-10 min IV.
- Fentanyl:
- Highly potent (80-100x morphine), lipophilic.
- Onset: 1-2 min IV, short duration.
- Inactive metabolites.
⭐ Fentanyl is often preferred over morphine for PCA in patients with renal impairment due to its inactive metabolites.
- Hydromorphone:
- Alternative to morphine, potent (5-7x morphine).
- Less histamine; ↓ nausea/pruritus vs morphine.
- Safer in renal dysfunction than morphine.
- Tramadol:
- Atypical weak opioid; SNRI activity.
- For mild-moderate pain.
- Analgesic ceiling effect; risk of seizures.
PCA Pros & Pitfalls - Upsides & Uh-Ohs
-
Upsides:
- Superior analgesia, ↑ patient satisfaction.
- Potentially ↓ total opioid dose, less sedation.
- Patient autonomy in pain control.
-
Uh-Ohs (Pitfalls):
- ⚠️ Respiratory depression - major concern.
- Common side effects: N/V, pruritus.
- Errors: device programming, patient misuse.
- Not for all: needs patient cognition/dexterity.
⭐ PCA by proxy (unauthorized activation by anyone other than the patient) is a major safety hazard, significantly increasing the risk of respiratory depression.
Special Scenarios & Alerts - Tailored PCA Tactics
- Pediatrics: Weight-based dosing (morphine 0.01-0.02 mg/kg), strict monitoring.
- Obstetrics (Labor): Epidural PCA; IV remifentanil option.
- Elderly: ↓ dose, ↑ lockout; monitor CNS.
- Obese: Ideal Body Weight (IBW)/Adjusted Body Weight (ABW) dosing; OSA risk.
- Opioid-Tolerant: ↑ doses; multimodal analgesia.
- Renal/Hepatic Impairment: Fentanyl/hydromorphone preferred. Adjust dose.
- Sleep Apnea (OSA): ⚠️ High risk! Monitor SpO2/EtCO2. Avoid basal.
⭐ Key absolute contraindications to PCA include patient refusal, inability to understand the device, or allergy to the prescribed opioid.
High‑Yield Points - ⚡ Biggest Takeaways
- PCA enables patient-controlled delivery of opioids (e.g., morphine, fentanyl).
- Essential parameters: bolus dose, lockout interval; basal infusion is optional.
- Provides superior pain relief and high patient satisfaction.
- Major risk: respiratory depression, especially with basal rates or programming errors.
- Monitor: respiratory rate, sedation score, pain score; naloxone for reversal.
- Avoid in young children, cognitively impaired, or patients unable to operate the device properly.
- Demand-only PCA is generally safer than PCA with continuous background infusion regarding respiratory risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

