NP: Definition & Mechanisms - Nerve Zingers Defined
- Definition (IASP): Pain caused by a lesion or disease of the somatosensory nervous system. Characterized by burning, shooting, or electric shock-like sensations.
- Common Etiologies:
- Metabolic: Diabetic Neuropathy (most frequent).
- Infectious: Post-Herpetic Neuralgia (PHN), HIV neuropathy.
- Compressive/Traumatic: Radiculopathy, Trigeminal Neuralgia (TN).
- Post-Surgical Pain, Phantom Limb Pain, Chemotherapy-Induced Peripheral Neuropathy (CIPN).
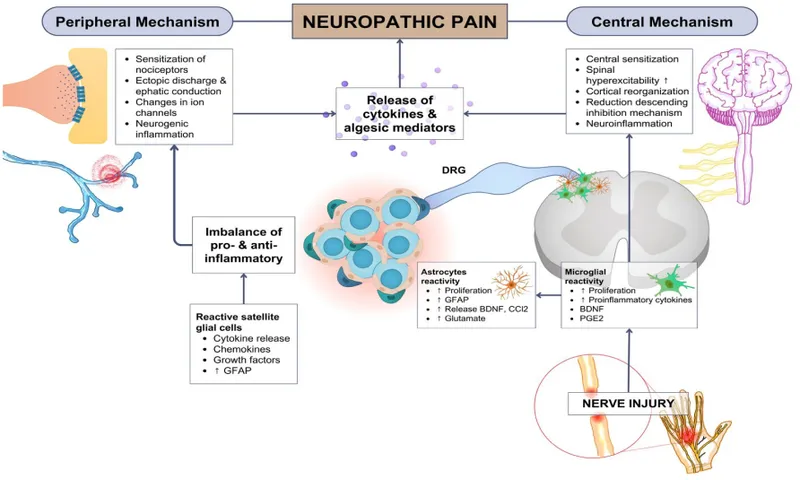
- Key Pathophysiological Mechanisms:
- Peripheral Sensitization: Lowered nociceptor activation threshold and increased responsiveness (e.g., altered ion channel expression like Nav1.7).
- Central Sensitization: Enhanced excitability of CNS neurons (spinal cord, brain); involves NMDA receptors, wind-up, and Long-Term Potentiation (LTP).
- Ectopic Discharges: Spontaneous, aberrant firing from damaged primary afferent neurons.
- Disinhibition: Reduced function of inhibitory pathways (e.g., GABAergic, glycinergic).
- Structural Reorganization: e.g., Aβ fibers sprouting into superficial dorsal horn laminae.
⭐ Allodynia (pain evoked by a stimulus that does not normally provoke pain) is a hallmark feature frequently tested. 📌 Nerve fibers: Aδ (fast, sharp "zingers") & C fibers (slow, burning/aching).
NP: Clinical Features & Diagnosis - Spotting the Signs
-
Characteristic Symptoms:
- Spontaneous pain: Burning (common), shooting, electric shock-like, stabbing.
- Evoked pain: Allodynia (pain from non-painful stimuli like light touch), hyperalgesia (↑ pain response to noxious stimuli).
- Paresthesia (pins & needles, tingling), dysesthesia (unpleasant abnormal sensation, e.g., crawling).
-
Clinical Examination:
- Focus: Identify lesion/disease affecting somatosensory system.
- Sensory testing: Assess for positive signs (allodynia, hyperalgesia) & negative signs (hypoesthesia, hypoalgesia).
- Look for autonomic signs (e.g., skin color/temperature changes).
-
Screening Tools:
Tool Score for NP Key Features DN4 ≥4/10 7 symptom, 3 examination items LANSS ≥12/24 5 symptom, 2 examination items PainDETECT ≥19/38 Patient-reported, 7 weighted sensory items
⭐ The 'Leeds Assessment of Neuropathic Symptoms and Signs' (LANSS) scale helps differentiate neuropathic from nociceptive pain.
- Diagnostic Flow:
- Key Investigations (when indicated):
- Nerve Conduction Studies (NCS) & Electromyography (EMG).
- Quantitative Sensory Testing (QST).
NP: Management Strategies - Taming the Tingles
Stepwise approach is key. Always consider non-pharmacological therapies adjunctively.
Pharmacological Agents:
| Class | MOA Highlights | Examples | Key SEs / Notes (Doses are typical starting/max) |
|---|---|---|---|
| TCAs | NE & 5-HT reuptake ↓ | Amitriptyline (10-25 mg hs, up to 150 mg) | Anticholinergic (dry mouth, constipation), sedation, cardiotoxicity. Start low. |
| SNRIs | NE & 5-HT reuptake ↓ | Duloxetine (30-60 mg/day, max 120 mg), Venlafaxine | Nausea, dizziness, insomnia, HTN. Good for comorbid depression/anxiety. |
| Gabapentinoids | Bind α2-δ Ca²⁺ channels, ↓ NT release | Gabapentin (start 300 mg, max 3600 mg/day), Pregabalin (start 75 mg BD, max 600 mg/day) | Sedation, dizziness, peripheral edema, weight gain. Renal dose adjustment. |
| Opioids | Weak µ-agonist; NE/5-HT reuptake ↓ (Tramadol) | Tramadol (50-100 mg q4-6h, max 400 mg/day), Morphine (refractory) | Nausea, constipation, sedation, dependence risk. Tramadol: seizure risk. |
| Topical Agents | Local Na⁺ channel blockade | Lidocaine 5% patch | Local skin reactions (erythema, rash). For localized NP. Max 3 patches/12h. |
Non-Pharmacological:
- TENS (Transcutaneous Electrical Nerve Stimulation)
- Physiotherapy, exercise
- Psychological therapies (CBT, mindfulness)
Interventional & Other Third-Line Options (Refractory Pain):
- Nerve blocks (local anesthetic +/- steroid)
- Spinal Cord Stimulation (SCS)
- Intrathecal drug delivery
- Other Antiepileptics (e.g., Carbamazepine for Trigeminal Neuralgia; Lamotrigine)
High‑Yield Points - ⚡ Biggest Takeaways
- Neuropathic pain results from lesion or disease of the somatosensory nervous system.
- Key symptoms include allodynia (pain from non-painful stimuli) and hyperalgesia.
- Examples: Diabetic neuropathy, postherpetic neuralgia (PHN), trigeminal neuralgia.
- First-line pharmacotherapy: Gabapentinoids (e.g., pregabalin), TCAs (e.g., amitriptyline), SNRIs (e.g., duloxetine).
- Carbamazepine is the drug of choice specifically for trigeminal neuralgia.
- Opioids are generally considered second or third-line options.
- Topical agents like lidocaine or capsaicin can be useful for localized neuropathic pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

