IPP Basics & Assessment - Ground Zero Prep
- Goal: Diagnose & treat pain via minimally invasive techniques.
- Indications: Chronic pain refractory to conservative Rx (neuropathic, MSK, cancer).
- Contraindications (Absolute): Infection at site, uncorrected coagulopathy (INR > 1.5, Plt < 50k), true allergy, patient refusal.
- Patient Assessment:
- History: 📌 OLD CARTS (Onset, Location, Duration, Character, Aggravating/Relieving, Radiation, Timing, Severity).
- Exam: Focused neuro/MSK. Pain scales (VAS, NRS).
- Labs/Imaging: Coags, relevant imaging (MRI/CT/X-ray).
- Informed Consent.
- Safety Essentials: "Time-out", Asepsis, Image guidance (US/Fluoroscopy), Radiation safety (ALARA).
⭐ A "Time Out" (correct patient, site, procedure) is MANDATORY before needle insertion.
Major Nerve Blocks - Pinpoint Relief
- Principle: Targeted delivery of local anesthetics (LA) ± corticosteroids near specific nerves or nerve plexuses for diagnosis or therapy.
- Guidance is Key: Fluoroscopy or Ultrasound essential for precision and safety.
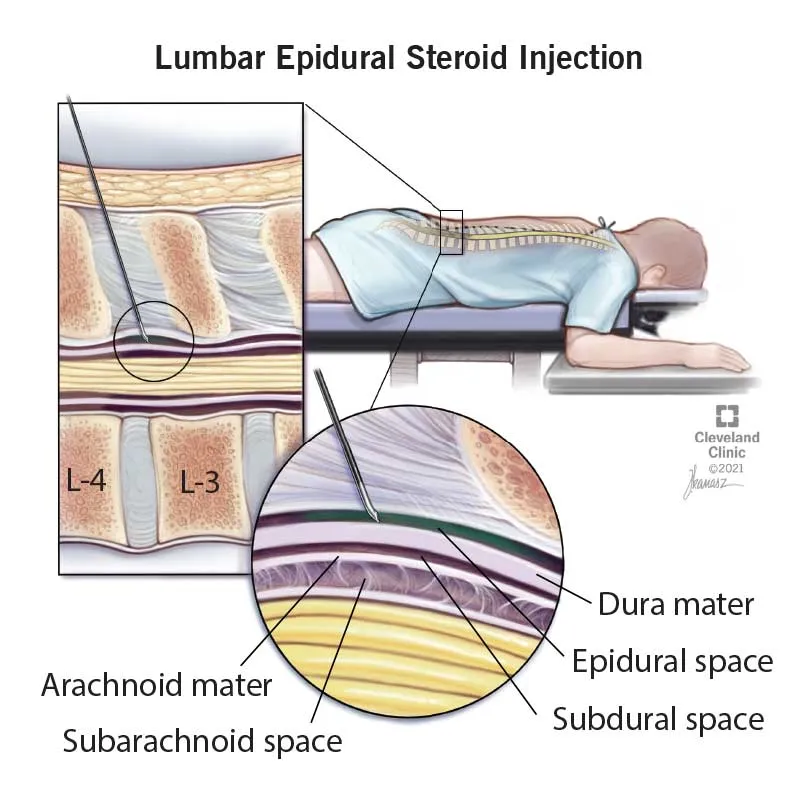
- Key Procedures & Indications:
- Epidural Steroid Injections (ESI): For radiculopathy, spinal stenosis.
- Approaches: Interlaminar, Transforaminal (TFESI - more specific).
- Facet Joint Interventions: For facet-mediated axial pain.
- Diagnostic: Medial Branch Block (MBB).
- Therapeutic: Radiofrequency Ablation (RFA) of medial branches.
- Sympathetic Blocks: For CRPS, visceral pain.
- Examples: Stellate ganglion, Lumbar sympathetic, Celiac plexus.
- Major Peripheral Nerve Blocks: For specific neuralgias (e.g., occipital, genicular).
- Epidural Steroid Injections (ESI): For radiculopathy, spinal stenosis.
- Common Agents: LAs (Bupivacaine, Lidocaine), Steroids (Triamcinolone).
- Risks: Infection, hematoma, nerve injury, LA toxicity.
⭐ For facet joint pain, a positive response to two diagnostic medial branch blocks (MBBs) with >80% pain relief is typically required before proceeding to RFA.
Advanced Pain Therapies - Beyond Blocks
- Radiofrequency Ablation (RFA)
- Mechanism: Thermal neurolysis via high-frequency current.
- Types: Conventional (lesion at 80-90°C), Pulsed (non-destructive, neuromodulatory), Cooled (larger lesions).
- Indications: Facet joint arthropathy, sacroiliitis, trigeminal neuralgia.
- Spinal Cord Stimulation (SCS)
- Mechanism: Gate control theory modulation; paresthesia overlaps pain area.
- Indications: Failed Back Surgery Syndrome (FBSS), Complex Regional Pain Syndrome (CRPS), refractory neuropathic pain.
- Trial period essential before permanent implant.
- Intrathecal Drug Delivery Systems (IDDS)
- Mechanism: Direct delivery of microdoses to CSF.
- Indications: Severe cancer pain, intractable chronic non-malignant pain, spasticity (baclofen).
- Common drugs: Morphine, ziconotide, baclofen.
- Peripheral Nerve Stimulation (PNS)
- Targets specific peripheral nerves for mononeuropathies (e.g., occipital neuralgia).

⭐ Ziconotide, an N-type calcium channel blocker, is a non-opioid analgesic used in intrathecal pumps and does NOT cause respiratory depression.
Imaging & Pharmacology - See & Soothe
- Imaging Modalities:
- Fluoroscopy: Real-time X-ray, needle guidance. AP, lateral, oblique views. Contrast (Iohexol) confirms spread. ⚠️ Radiation.
- Ultrasound (USG): Real-time, no radiation. Visualizes nerves, vessels, soft tissues. Linear (superficial) & curvilinear (deep) probes.
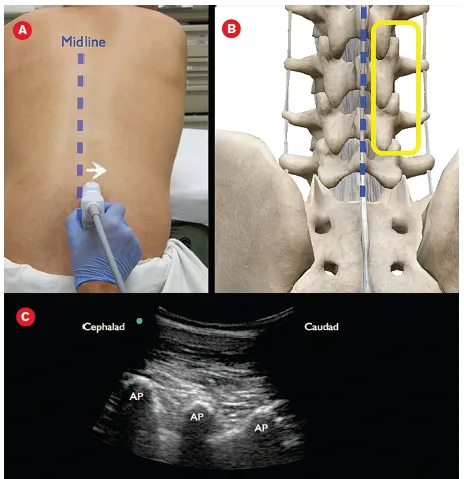
- Pharmacological Agents:
- Local Anesthetics (LAs): Reversibly block Na+ channels.
- Amides (Lidocaine, Bupivacaine; 📌 two "i"s): Longer action. Max Lidocaine: 7 mg/kg (with epi).
- Esters (Procaine, Chloroprocaine; 📌 one "i"): Shorter action, ↑allergy (PABA).
- Corticosteroids: Potent anti-inflammatory.
- Particulate (Methylprednisolone): Longer acting, ⚠️ embolic risk (avoid intravascular).
- Non-particulate (Dexamethasone): Safer for high-risk vascular areas (transforaminal).
- Contrast Media: Non-ionic iodinated (Iohexol) confirms placement, rules out intravascular uptake.
⭐ For Local Anesthetic Systemic Toxicity (LAST), esp. Bupivacaine cardiotoxicity, give Intralipid 20% (1.5 mL/kg bolus).
- Local Anesthetics (LAs): Reversibly block Na+ channels.
High‑Yield Points - ⚡ Biggest Takeaways
- Celiac plexus block: key for upper abdominal cancer pain (e.g., pancreatic).
- Stellate ganglion block: for upper limb CRPS, Raynaud's disease.
- Lumbar sympathetic block: for lower limb CRPS, phantom limb pain.
- Epidural Steroid Injections (ESI): for radicular pain; transforaminal approach common.
- Radiofrequency Ablation (RFA) of medial branches: for facet joint pain.
- Spinal Cord Stimulation (SCS): for Failed Back Surgery Syndrome (FBSS), refractory CRPS.
- Intrathecal pumps: for severe refractory cancer pain or chronic non-malignant pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

