Preeclampsia: Definition & Dx - Spotting the Signs
- New HTN >20 wks gestation + Proteinuria OR End-organ dysfunction.
- Diagnostic Criteria:
| Feature | Criteria |
|---|---|
| HTN | BP ≥140/90 mmHg (x2, 4h apart) OR ≥160/110 mmHg (once) |
| Proteinuria | ≥300mg/24h; P:C ratio ≥0.3; Dipstick 2+ |
| Severe Features (HTN + any of these, even no proteinuria): | |
| Thrombocytopenia | Platelets <100,000/µL |
| Renal Insufficiency | Cr >1.1mg/dL / doubling |
| Liver Dysfunction | AST/ALT >2x ULN; RUQ/epigastric pain |
| Pulmonary Edema | Present |
| Cerebral/Visual | New headache, visual changes |
- 📌 HELLP: Hemolysis, EL (Elevated Liver enzymes), LP (Low Platelets).
⭐ Postpartum preeclampsia can occur, usually within 48h but up to 6 weeks.
Pathophysiology: Preeclampsia - Systemic Storm
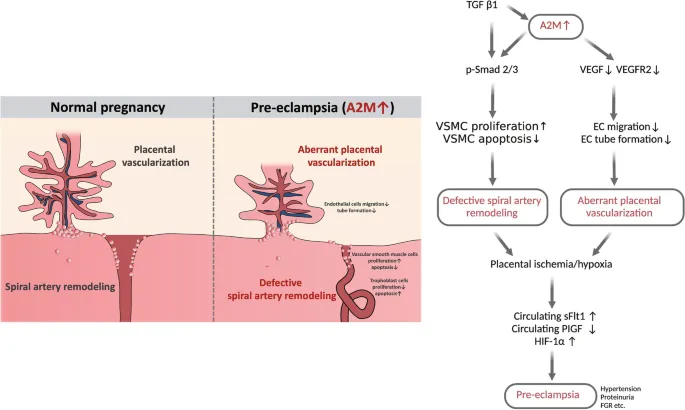
- Abnormal Placentation: Defective spiral artery remodeling by cytotrophoblasts → placental hypoperfusion & ischemia.
- Release of anti-angiogenic factors (sFlt-1, sEng) & pro-inflammatory mediators.
- Endothelial Dysfunction: Systemic maternal endothelial cell activation/damage → ↑vascular permeability, ↓vasodilation (↓NO, ↑endothelin).
- Vasospasm: Generalized vasoconstriction → hypertension, reduced organ perfusion (kidney, liver, brain, placenta).
⭐ Imbalance between thromboxane A2 (vasoconstrictor, platelet aggregator) and prostacyclin (vasodilator, platelet inhibitor) is a key feature, with ↑Thromboxane A2 / ↓Prostacyclin ratio.
This leads to a multi-systemic disorder characterized by hypertension and end-organ damage.
Complications: Maternal & Fetal - Double Danger
- Maternal:
- CNS: Eclampsia (seizures), CVA (stroke), PRES (Posterior Reversible Encephalopathy Syndrome)
- CV: Severe HTN, pulmonary edema, cardiac failure
- Hematologic: HELLP (📌 Hemolysis, Elevated Liver enzymes, Low Platelets), DIC
- Renal: AKI (Acute Kidney Injury), oliguria
- Hepatic: Subcapsular hematoma, rupture
- Respiratory: ARDS (Acute Respiratory Distress Syndrome), laryngeal edema
- Fetal:
- Placental insufficiency: IUGR (Intrauterine Growth Restriction), oligohydramnios
- Abruptio placentae
- Prematurity & sequelae
- HIE (Hypoxic Ischemic Encephalopathy), IUFD (Intrauterine Fetal Demise)
⭐ HELLP syndrome: major risk for mother & fetus. Suspect with RUQ pain, N/V, malaise in preeclampsia.
Anesthesia: Preeclampsia - Navigating Safely
- Goal: Maternal-fetal safety, stable hemodynamics, prevent eclampsia.
- Pre-anesthetic: Airway (edema!), platelets (neuraxial if >70-80k/µL), BP control (SBP <160, DBP <110 mmHg).
- Neuraxial (Epidural/Spinal): Preferred. Gradual onset aids BP stability. Avoid if coagulopathy.
- General Anesthesia (GA):
- For severe thrombocytopenia (<70k), urgent C/S, failed/contraindicated regional.
- Risks: Difficult intubation (anticipate!), hypertensive response, aspiration.
- Mgmt: RSI, short-acting agents, attenuate pressor response (Labetalol).
- Key: Continue $MgSO_4$ (potentiates NMBs). Judicious IV fluids (pulmonary edema risk).
⭐ $MgSO_4$ is the primary anticonvulsant; it also decreases MAC of volatile anesthetics and potentiates neuromuscular blockade.
"""
Eclampsia & HELLP Mgmt - Crisis Control Now
-
Eclampsia:
- Immediate: ABCs, Left lateral. Prevent injury.
- Seizure control: MgSO4
- Loading: 4-6g IV (15-20 min).
- Maintenance: 1-2g/hr IV.
- Antidote: Ca Gluconate 1g IV.
- BP control: If SBP ≥160 / DBP ≥110 mmHg (Labetalol, Hydralazine).
- Definitive: Prompt delivery post-stabilization.
-
HELLP Syndrome:
- Diagnosis (📌 HELLP):
- Hemolysis: LDH >600 U/L.
- Elevated Liver enzymes: AST/ALT >2x ULN or >70 U/L.
- Low Platelets: <100,000/mm³.
- Management:
- Stabilize: MgSO4 (prophylaxis), BP control.
- Corticosteroids: If <34 wks (fetal lungs); may aid maternal PLT.
- Delivery: Definitive. Prompt if >34 wks or unstable.
- Diagnosis (📌 HELLP):
⭐ For HELLP syndrome, delivery is indicated regardless of gestational age with maternal multi-organ dysfunction or non-reassuring fetal status. """
High‑Yield Points - ⚡ Biggest Takeaways
- Preeclampsia: New-onset hypertension (>140/90 mmHg) after 20 weeks gestation + proteinuria or end-organ dysfunction.
- Eclampsia: Preeclampsia + new-onset grand mal seizures.
- Magnesium sulfate (MgSO4): Key for seizure prophylaxis and treatment; monitor for toxicity.
- Definitive management: Prompt delivery of the fetus and placenta.
- Neuraxial anesthesia (epidural/spinal) is preferred if platelets >75,000/µL and no coagulopathy.
- HELLP syndrome (Hemolysis, Elevated Liver enzymes, Low Platelets) is a critical variant requiring urgent multidisciplinary care and often prompt delivery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

