EEG & Processed EEG - Brain's Electrical Symphony
EEG: Brain's electrical activity. Processed EEG (pEEG) simplifies anesthesia depth monitoring.
- EEG Waves (📌 BAT-D: Beta→Alpha→Theta→Delta)
- Beta (>13 Hz): Awake, alert; initial anesthetic ↑.
- Alpha (8-13 Hz): Relaxed; light anesthesia.
- Theta (4-8 Hz): Light sleep/anesthesia.
- Delta (0.5-4 Hz): Deep sleep/anesthesia.
- Anesthetic EEG Effects: ↑Beta → Alpha/Theta → Delta → Burst Suppression → Isoelectric.
- Key Patterns:
- Burst Suppression: Deep anesthesia, cerebral compromise.
- Isoelectric EEG: Profound CNS depression.
- Processed EEG (BIS, Entropy, SedLine):
- Principle: Single index for hypnosis.
- GA Targets: BIS/Entropy 40-60; SedLine PSI 25-50.
- Limitations: EMG, drug-specific effects.
⭐ Bispectral Index (BIS) values between 40 and 60 generally indicate an appropriate level of hypnosis for general anesthesia, reducing the risk of intraoperative awareness.

Evoked Potentials - Nerve Signal Sentinels
Evoked Potentials (EPs) assess neural pathway integrity via electrical responses to stimulation.
- Significant Changes: Alert if:
-
10% ↑ in latency (conduction time)
-
50% ↓ in amplitude (signal strength)
-
- Types & Characteristics:
| Feature | SSEP (Somatosensory) | BAEP (Brainstem Auditory) | MEP (Motor) |
|---|---|---|---|
| Pathway | Dorsal column-medial lemniscus | Auditory pathway (CN VIII to cortex) | Corticospinal tract |
| Stimulus | Peripheral nerve (median, ulnar, tibial) | Click sounds (earphones) | Transcranial (electrical/magnetic) |
| Recording | Scalp (cortex), spinal cord | Scalp (vertex, mastoid) | Muscles, spinal cord |
| Uses | Spinal surgery, carotid | Posterior fossa surgery, acoustic neuroma | Spinal, aortic, brain surgery |
| Anesthetic Sensitivity | Less sensitive; NMBs affect muscle potentials | Relatively resistant | High sensitivity: volatiles, NMBs |
⭐ Motor Evoked Potentials (MEPs) are highly sensitive to volatile anesthetics and neuromuscular blocking agents; Total Intravenous Anesthesia (TIVA) is often the preferred anesthetic technique when MEPs are monitored.
Cerebral Circulation & Oxygen - Flow & Fuel Gauge

-
Transcranial Doppler (TCD)
- Principle: Doppler effect (blood flow velocity).
- Windows: Transtemporal, transorbital, suboccipital, submandibular.
- Parameters:
Parameter Significance MFV Mean Flow Velocity; e.g., MCA 55±12 cm/s. PI Pulsatility Index; $PI = (SV - DV) / MV$; reflects CVR. Normal 0.6-1.1. - Uses: Vasospasm (post-SAH), emboli, cerebrovascular reactivity, brain death.
-
Cerebral Oximetry (NIRS)
- Principle: Near-infrared light (Beer-Lambert law) for regional cerebral oxygen saturation (rSO2).
- Values: Normal rSO2 ~60-75%.
- Desaturation: Drop >20-25% from baseline or absolute rSO2 <50%.
- Factors: PaO2, PaCO2, MAP, Hb, cerebral metabolic rate.
- Limitations: Scalp contamination, extracranial saturation.
⭐ rSO2 drop >20-25% from baseline or absolute <50% is critical, requiring intervention to prevent ischemia.
ICP Monitoring - Pressure Under Watch
- Indications: Severe TBI (GCS ≤8), SAH, large strokes, hydrocephalus.
- Monroe-Kellie Doctrine: Fixed intracranial volume (Brain + Blood + CSF). ↑ one component → ↓ others or ↑ICP.
- Methods:
- EVD (External Ventricular Drain): Gold standard; measures ICP & drains CSF.
- Intraparenchymal probes (e.g., Codman, Camino; fiberoptic/strain-gauge).
- Values & Thresholds:
- Normal ICP: <15 mmHg (adult, supine).
- Intracranial Hypertension (ICH): ICP >20-22 mmHg for >5 minutes.
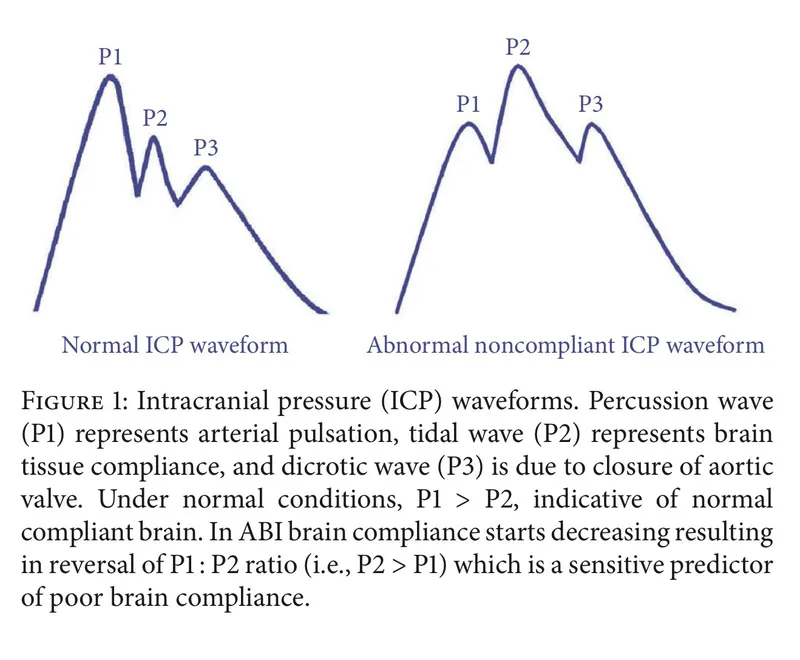
- ICP Waveforms:
- P1 (percussion), P2 (tidal/brain compliance), P3 (dicrotic). P2 > P1 (ominous) indicates ↓ compliance.
- Lundberg Waves: 📌 A (Awful plateau, >40-50 mmHg, pathological), B (Bad precursors), C (Common rhythmic).
- Cerebral Perfusion Pressure (CPP):
- Formula: $CPP = MAP - ICP$.
- Target: 50-70 mmHg (adults).
- ↑ICP Management: Tiered approach (see flowchart). Goal: ↓ICP, maintain CPP.
⭐ The External Ventricular Drain (EVD) is considered the gold standard for Intracranial Pressure (ICP) monitoring as it allows for both continuous pressure measurement and therapeutic drainage of cerebrospinal fluid (CSF).
High‑Yield Points - ⚡ Biggest Takeaways
- EEG detects cerebral ischemia, seizures, and monitors anesthetic depth (e.g., burst suppression).
- Evoked Potentials (SSEPs, BAEPs, VEPs) assess specific neural pathway integrity during surgery.
- Transcranial Doppler (TCD) measures CBFV, detecting vasospasm and microemboli.
- NIRS (Cerebral Oximetry) monitors regional cerebral oxygen (rSO2), detecting cerebral hypoxia.
- ICP monitoring is vital; maintain CPP >60 mmHg (CPP = MAP - ICP).
- BIS guides anesthetic depth (target 40-60), reducing awareness.
- MEPs assess motor tract integrity; sensitive to volatile anesthetics and relaxants.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

