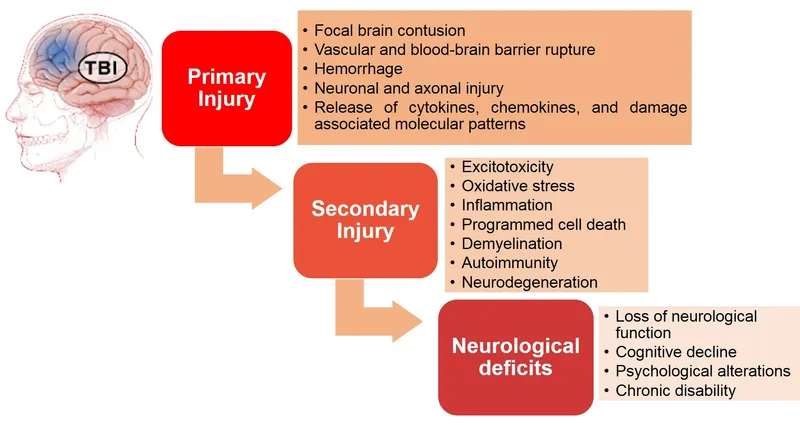
TBI Pathophysiology - Brain Under Siege
- Primary Injury:
- Irreversible mechanical damage occurring at impact (e.g., contusion, laceration, Diffuse Axonal Injury (DAI)).
- Secondary Injury:
- Develops minutes to days post-injury; a key therapeutic target, as it is potentially preventable or reversible.
- Exacerbated by:
- Systemic insults: Hypotension (SBP < 90 mmHg), Hypoxia (PaO2 < 60 mmHg).
- Intracranial events: Increased Intracranial Pressure (ICP), cerebral edema (vasogenic & cytotoxic), cerebral ischemia.
- Cellular damage cascade: Excitotoxicity (e.g., glutamate), inflammation, free radical production, apoptosis.
- Monro-Kellie Doctrine:
- The skull is a rigid box; the sum of intracranial volumes (brain parenchyma, blood, Cerebrospinal Fluid (CSF)) is constant.
- An increase in one component must be compensated by a decrease in another, otherwise ICP rises.
- Cerebral Perfusion:
- Cerebral autoregulation is often impaired in TBI.
- Cerebral Perfusion Pressure ($CPP = MAP - ICP$); target range is typically 50-70 mmHg.
⭐ Cushing's Triad: Represents a late and ominous sign of critically increased ICP and impending brainstem herniation. It consists of:
- Hypertension (often with a widened pulse pressure)
- Bradycardia
- Irregular respirations (e.g., Cheyne-Stokes breathing)
Preoperative Management - TBI Triage Time
- Airway: Secure early (RSI if GCS ≤8). Avoid hypoxia (SpO₂ >94%) & maintain normocapnia (PaCO₂ 35-45 mmHg).
- Breathing: Optimize oxygenation; mechanical ventilation often needed.
- Circulation:
- Maintain SBP >100 mmHg (adults), age-adjusted for pediatrics.
- Aggressive fluid resuscitation (isotonic crystalloids: NS, RL).
- Target CPP >60-70 mmHg; $CPP = MAP - ICP$.
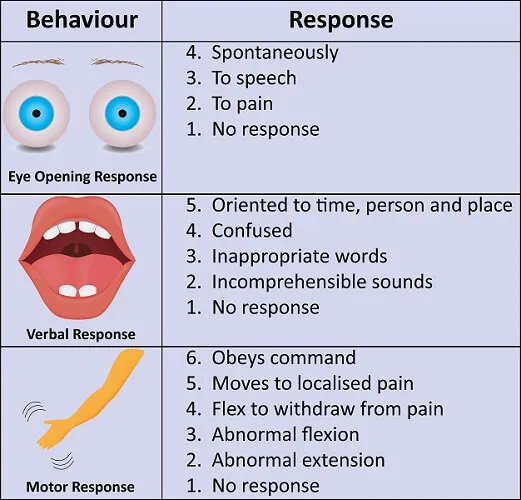
- Disability: Neurological assessment (GCS, pupils).
- Exposure/Environment: Prevent hypothermia (target >36°C). Control glucose.
⭐ High-Yield: Indications for ICP monitoring in severe TBI (GCS 3-8 with abnormal CT) OR (GCS 3-8 with normal CT but 2+ of: age >40 yrs, SBP <90 mmHg, or motor posturing).
📌 Mnemonic (ABCDE): Airway, Breathing, Circulation, Disability, Exposure/Environment control for secondary injury prevention during the "Golden Hour".
Intraoperative Anesthesia - Neuro-Protective Shield
- Primary Goals: Maintain CPP (50-70 mmHg), control ICP (<22 mmHg), ensure cerebral oxygenation.
- Induction Agents:
- Propofol (↓ICP; caution: hypotension).
- Etomidate (hemodynamic stability).
- Lidocaine (1.5 mg/kg) IV to blunt intubation response.
- Maintenance Strategy:
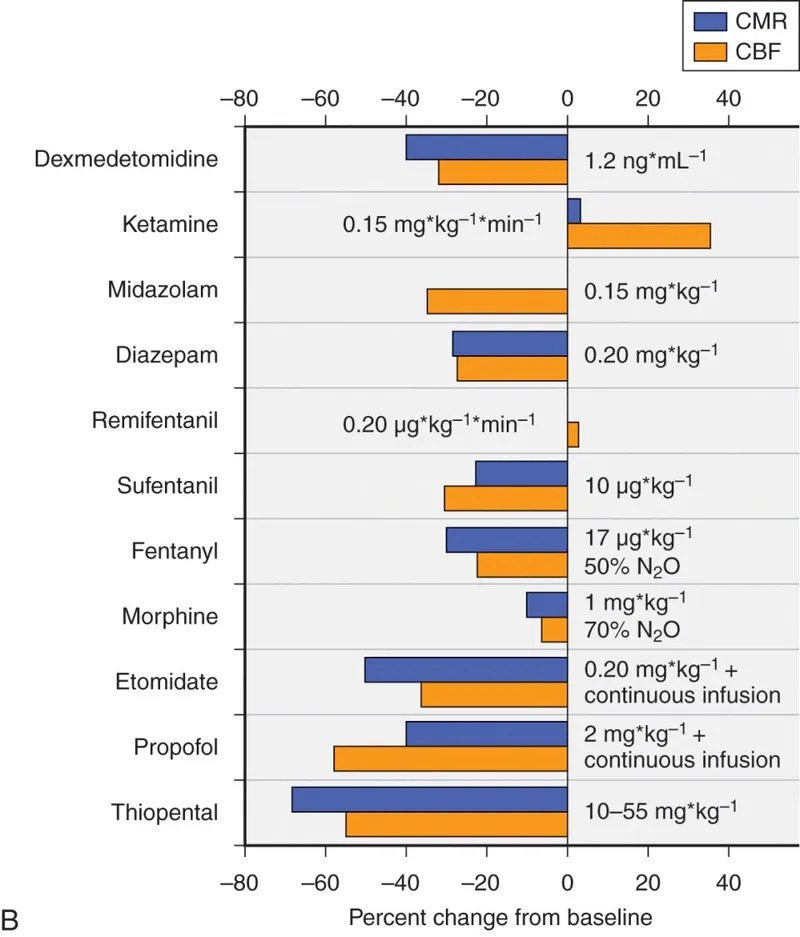
- TIVA (Propofol + Remifentanil): Preferred for ↓CMRO2, ↓CBF, ↓ICP.
- Volatiles (Isoflurane, Sevoflurane <1 MAC): Use cautiously; dose-dependent ↑CBF/ICP.
- Muscle Relaxants: Non-depolarizing (e.g., Rocuronium). Avoid suxamethonium if ↑ICP suspected.
- Ventilation: Target normocapnia (PaCO2 35-40 mmHg).
⭐ The cautious and transient use of hyperventilation to PaCO2 30-35 mmHg for acute ICP rise.
- Fluid Management: Isotonic crystalloids (e.g., Normal Saline). Avoid hypotonic solutions.
- Key Adjuncts:
- Maintain normothermia (36-37.5°C).
- Strict glucose control (target 140-180 mg/dL).
Postoperative Care - Recovery & Risks
- ICU Management: Neuro-ICU ideal.
- Maintain CPP > 60-70 mmHg, ICP < 20-22 mmHg.
- Normoxia (PaO2 > 100 mmHg), normocapnia (PaCO2 35-40 mmHg).
- Normothermia, euglycemia.
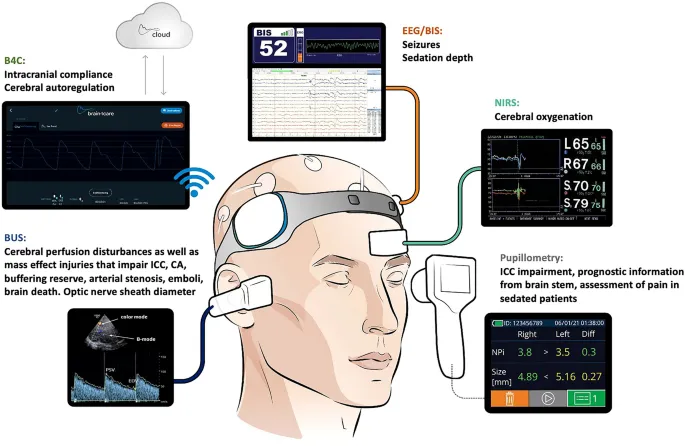
- Neuromonitoring: Continuous ICP, CPP; serial GCS, pupils.
- Sedation & Analgesia: Titrate carefully (e.g., propofol, opioids).
- Ventilation & Extubation:
- Lung-protective ventilation.
- Cautious extubation: assess neuro status, airway reflexes; risk of ICP ↑.
- Key Risks & Management:
- Cerebral Edema: Mannitol (0.25-1 g/kg), hypertonic saline.
- Seizures: Prophylaxis (e.g., Phenytoin, Levetiracetam).
- Infections (VAP, meningitis), DVT prophylaxis.
- Electrolyte disturbances (SIADH, CSW).
⭐ Prophylactic anticonvulsants (e.g., Phenytoin for 7 days) reduce early post-traumatic seizures (PTS) in high-risk TBI.
High‑Yield Points - ⚡ Biggest Takeaways
- Maintain CPP > 60-70 mmHg and ICP < 20-22 mmHg.
- Avoid hypotension (SBP < 90 mmHg) and hypoxia (PaO2 < 60 mmHg).
- Mild hyperventilation (PaCO2 30-35 mmHg) is temporary for ↑ ICP; avoid prolonged use.
- Mannitol (0.25-1 g/kg) or hypertonic saline (e.g., 3%) reduce ICP.
- Propofol/barbiturates ↓ CMRO2, ICP; risk hypotension, monitor hemodynamics.
- Optimize head position (midline, elevated 30°), avoid neck compression.
- Ketamine: cautiously used if CPP maintained; can ↑ ICP in some patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more